Ms. Thu's condition had persisted for two years. Doctors initially diagnosed epilepsy and prescribed anti-seizure medication, but her symptoms did not improve. Initially, her eyelid would twitch mildly, but the frequency gradually increased, spreading to her cheek and the corner of her mouth, causing her eye to close tightly and her face to distort for tens of seconds to several minutes.
A 3 Tesla MRI scan at Tam Anh General Hospital, TP HCM, revealed three points of vascular compression on the facial nerve (cranial nerve 7) in the cerebellopontine angle. The images showed an arterial loop directly contacting and pulsating against the nerve root. Doctor Mai Hoang Vu, from the Department of Neurosurgery - Spine, Neuroscience Center, explained that cranial nerve 7 controls facial muscle movement. When a blood vessel lies close to and continuously pulsates against a nerve root over an extended period, the myelin sheath protecting the nerve fiber can be damaged. This damage leads to unstable electrical impulses, causing involuntary spasms on one side of the face.
According to Doctor Vu, hemifacial spasm caused by vascular compression is often mistaken for epilepsy. However, this condition typically has an insidious onset, gradually worsens over time, and is not accompanied by any disturbance of consciousness. If the underlying cause is not addressed, hemifacial spasm due to neurovascular conflict tends to progress. Prolonged compression continuously irritates the nerve, leading to more frequent spasms, muscle fatigue, headaches, sleep disturbances, and a reduced quality of life for the patient.
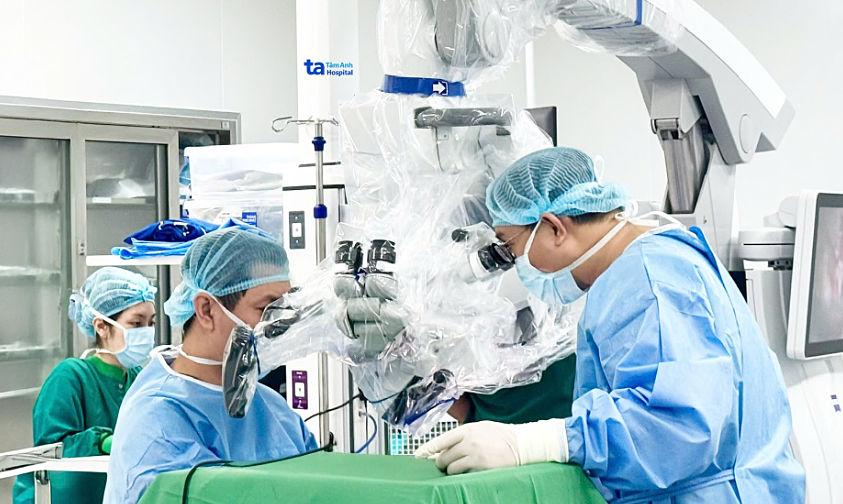 |
Doctors performing microvascular decompression surgery on Ms. Thu using a K.Zeiss Kinevo 900 surgical microscope. *Photo: Tam Anh General Hospital*
Following a consultation, Ms. Thu was scheduled for microvascular decompression surgery. Surgeons created a small bone window behind her ear to access the cerebellopontine angle. With the aid of an AI-integrated surgical microscope, they clearly observed individual nerve fibers and tiny blood vessels, accurately identifying the point of conflict. The blood vessel was then carefully separated from the nerve. Afterward, a specialized pad was placed to prevent re-contact, minimizing the risk of damage to adjacent structures.
Throughout the surgery, an intraoperative neurophysiological monitoring (IONM) system was used to record the facial nerve's responses. This system provided alerts upon detecting any abnormalities, enabling surgeons to make timely adjustments, thereby increasing the recovery rate and reducing the risk of complications such as facial weakness or paralysis and hearing loss.
Following the surgery, Ms. Thu's spasms diminished and completely resolved within a few days. Her face regained its balance, and no abnormal twitching occurred during her daily activities. She received postoperative monitoring and was scheduled for regular follow-up appointments to assess facial nerve function and ensure no recurrence.
According to Doctor Vu, medical treatment or botulinum toxin injections can provide temporary symptom relief but do not address the underlying cause of the compression. Microvascular decompression surgery is currently the definitive treatment method, offering a high cure rate.
Doctors advise against complacency when symptoms such as eyelid twitching, twitching at the corner of the mouth, or intermittent facial distortion appear, especially if these symptoms gradually worsen over time. Patients should visit a hospital with a neurology department to undergo a specialized MRI scan, determine the cause, and receive timely intervention.
Trong Nghia
| Readers can submit questions about neurological diseases here for doctors to answer |












