Answer:
For postpartum disc herniation, it is recommended to visit a multispecialty hospital. A doctor will conduct a thorough examination and develop an individualized treatment protocol. This approach often involves coordination among musculoskeletal, physical therapy and rehabilitation, and orthopedic trauma departments to achieve optimal treatment results.
Postpartum disc herniation occurs when the discs between vertebrae are damaged, causing the nucleus pulposus to protrude and compress nerve roots or the spinal cord. This condition commonly affects areas under significant stress during pregnancy and childcare, such as the cervical and lumbar spine. It arises from physiological and structural changes, along with lifestyle habits during pregnancy and the postpartum period.
During pregnancy, women often experience weight gain, which increases pressure on the spine, particularly in the lumbar region, leading to disc compression. Changes in maternal posture also shift the spinal axis from its natural alignment, contributing to disc herniation.
The immense pressure on the lumbar region during childbirth can damage discs and cause herniation. Elevated levels of relaxin and progesterone hormones, which relax the pelvic ligaments for delivery, also loosen ligaments and connective tissues around the spine. This reduces their ability to stabilize and protect the discs.
After childbirth, core muscles supporting the spine, such as the abdominal and back muscles, often stretch and weaken. This makes many new mothers susceptible to disc herniation while caring for their infants, leading to pain, restricted movement, poor sleep quality, and psychological impact.
Several methods can help treat postpartum disc herniation:
Maintaining correct posture when holding or breastfeeding your baby is crucial. Avoid bending, sudden movements, twisting, and lifting heavy objects to reduce pressure on the spine and discs. Combining this with adequate rest helps the body recover and alleviates herniation.
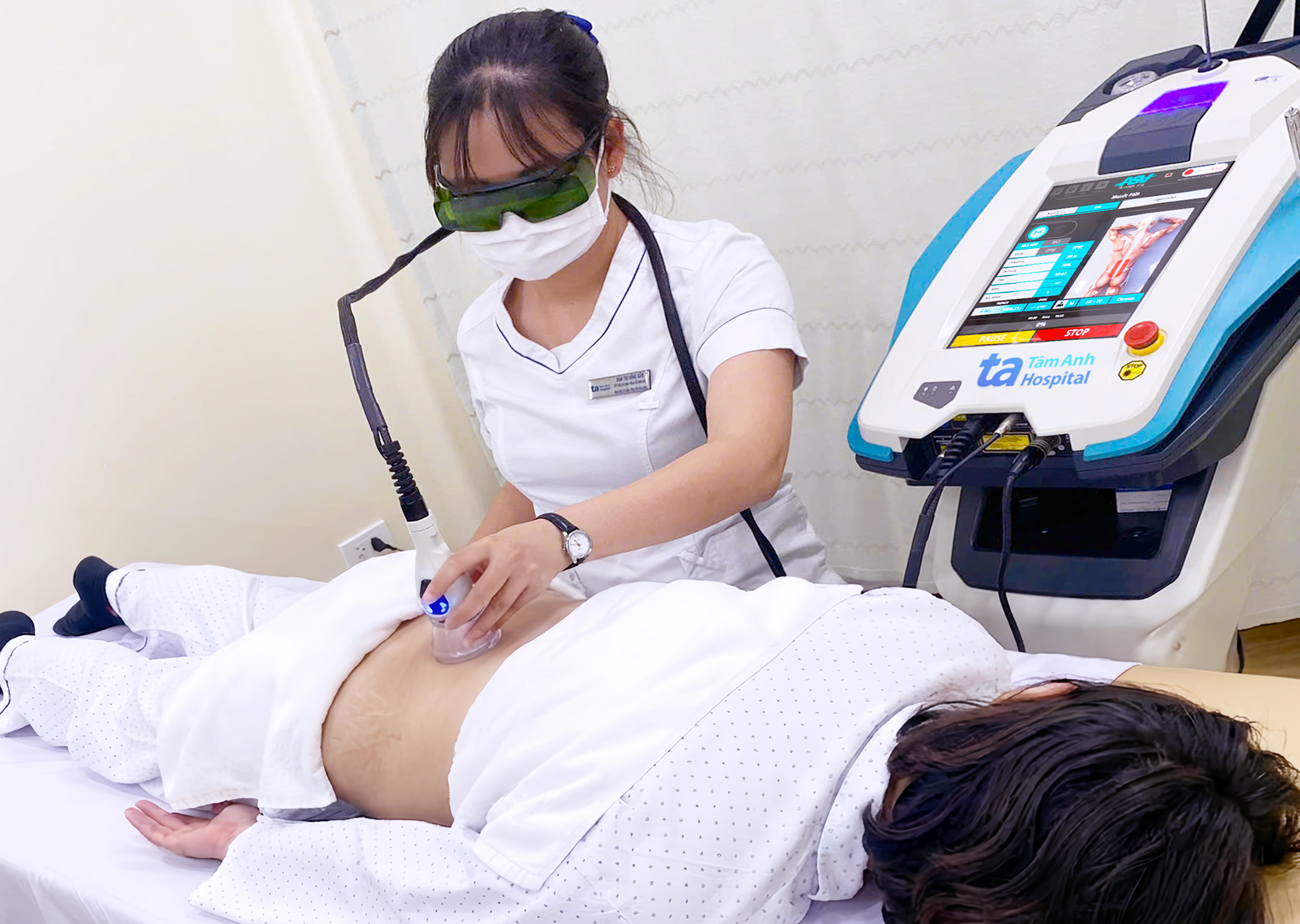 |
Treating postpartum disc herniation with laser therapy. Illustration: Tam Anh General Hospital |
Physical therapy and rehabilitation can reduce nerve compression, alleviate pain, improve circulation, and support tissue recovery. Based on age, weight, pain level, and herniation severity, physical therapy specialists recommend suitable methods. These may include soft tissue therapy, pain-reducing exercises, muscle relaxation, or the use of machines such as shockwave, ultrasound, shortwave, microwave, thermal magnetic field, electrotherapy, or laser therapy.
Patients should seek care at hospitals with specialized physical therapy and rehabilitation departments for expert consultation and supervised exercise. Avoiding unverified facilities is important, as incorrect spinal manipulation can worsen herniation and cause dangerous injuries.
Following an exercise regimen tailored by a physical therapy specialist helps strengthen abdominal, back, and pelvic floor muscles, which support the spine. This maintains pain relief at home and prevents recurrence, which is vital for patients with disc herniation.
Medical treatment, in some cases, involves pain relievers or muscle relaxants at appropriate dosages. Doctors carefully consider medication use, especially for breastfeeding mothers, to ensure the safety of both mother and baby.
Surgical intervention is considered when conservative measures are ineffective or when severe nerve compression symptoms appear. A doctor will assess the condition to determine the most suitable intervention, aiming for minimal invasiveness.
Master, Doctor Nguyen Thi Phuong
Department of Musculoskeletal
Tam Anh Cau Giay Polyclinic