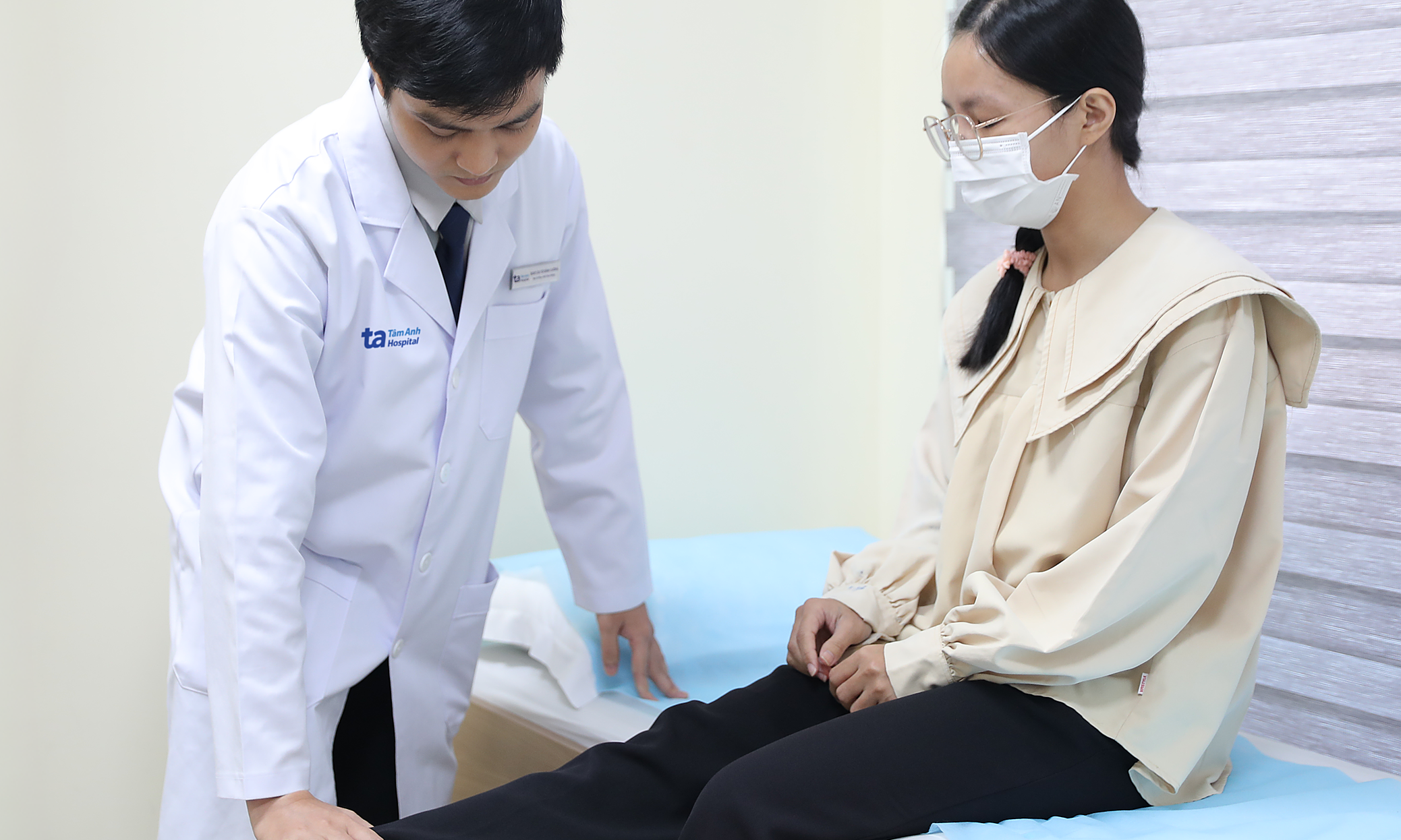
Mr. Nam had undergone endoscopic resection for prostate enlargement six months prior. Recently, he developed dull pain in his lower abdomen, along with very difficult and intermittent urination, and stinging pain.
Endoscopy at Tam Anh General Hospital Ho Chi Minh City revealed a severe stricture in his posterior urethra, located deep within the pelvic region. The diameter of his urinary tract was approximately 1,2 mm.
Master of Science, Doctor Cao Vinh Duy, from the Urology Department, Center for Urology - Nephrology - Andrology, explained that the patient's urethral stricture resulted from fibrous scarring. This scarring formed after the endoscopic prostate resection. He noted this is a common occurrence, often due to the endoscopic instruments being larger than the patient's urethra during surgery, or repeated catheterization causing mucosal damage.
Since Mr. Nam's stricture was only about one cm long, the surgical team performed posterior urethral reconstruction using an "end-to-end anastomosis" method. Surgeons removed the narrowed segment and then reconnected the two healthy ends of the urethra with eight separate stitches. This procedure avoided intervention in the pubic bone or corpus cavernosum, effectively restoring a clear urinary tract.
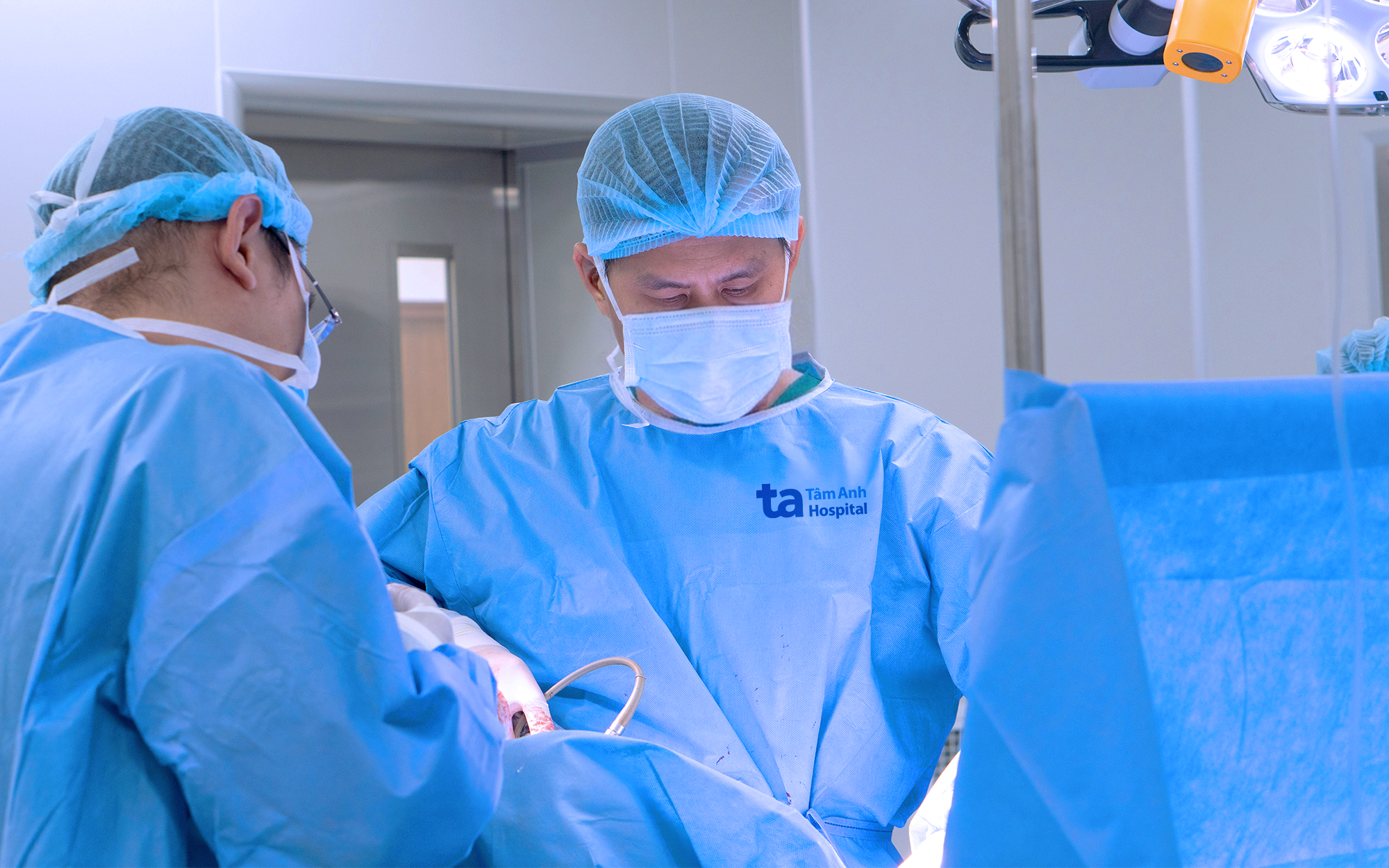 |
Doctor Duy (center) performing urethral reconstruction surgery for a patient. Photo: Tam Anh General Hospital. |
Following the three-hour intervention, the new urethral anastomosis was clear and unstrained, reducing the recurrence rate to below 5%. After surgery, the patient had the drainage tube removed after 48 hours and a urinary catheter placed for two to three weeks. He experienced minimal incision pain, resumed normal eating, and was discharged.
Mr. Nam received instructions on wound care and antibiotic use to prevent infection. According to Doctor Duy, infection is the leading cause of surgical failure. It can delay wound healing and stimulate the formation of new fibrous tissue, leading to faster re-stricture.
Urethral stricture can affect patients with a history of urinary tract intervention or pelvic trauma. Many patients, however, often confuse the symptoms with recurrent prostate enlargement and self-medicate. This can lead to severe fibrosis, complicating future reconstructive interventions.
To mitigate this risk, Doctor Duy advises patients who have undergone urinary tract surgery to adhere to scheduled follow-up appointments, drink adequate water, and maintain proper genital hygiene. Symptoms such as weak or dribbling urination, prolonged urination time, stinging urination, dull pain in the perineum or lower abdomen, unusual urine color or smell, or swelling of the penis or scrotum require immediate medical attention for timely intervention, to preserve physiological function, and shorten recovery time.
Bao Anh
*Patient's name has been changed