Doctor Cam Ngoc Phuong, Director of the Neonatal Center at Tam Anh General Hospital TP HCM, reported that the premature baby, born at 31 weeks gestational age, weighed only one-third of a typical infant at the same stage. The baby experienced respiratory failure, pneumonia, and struggled with weight gain due to three gene mutations.
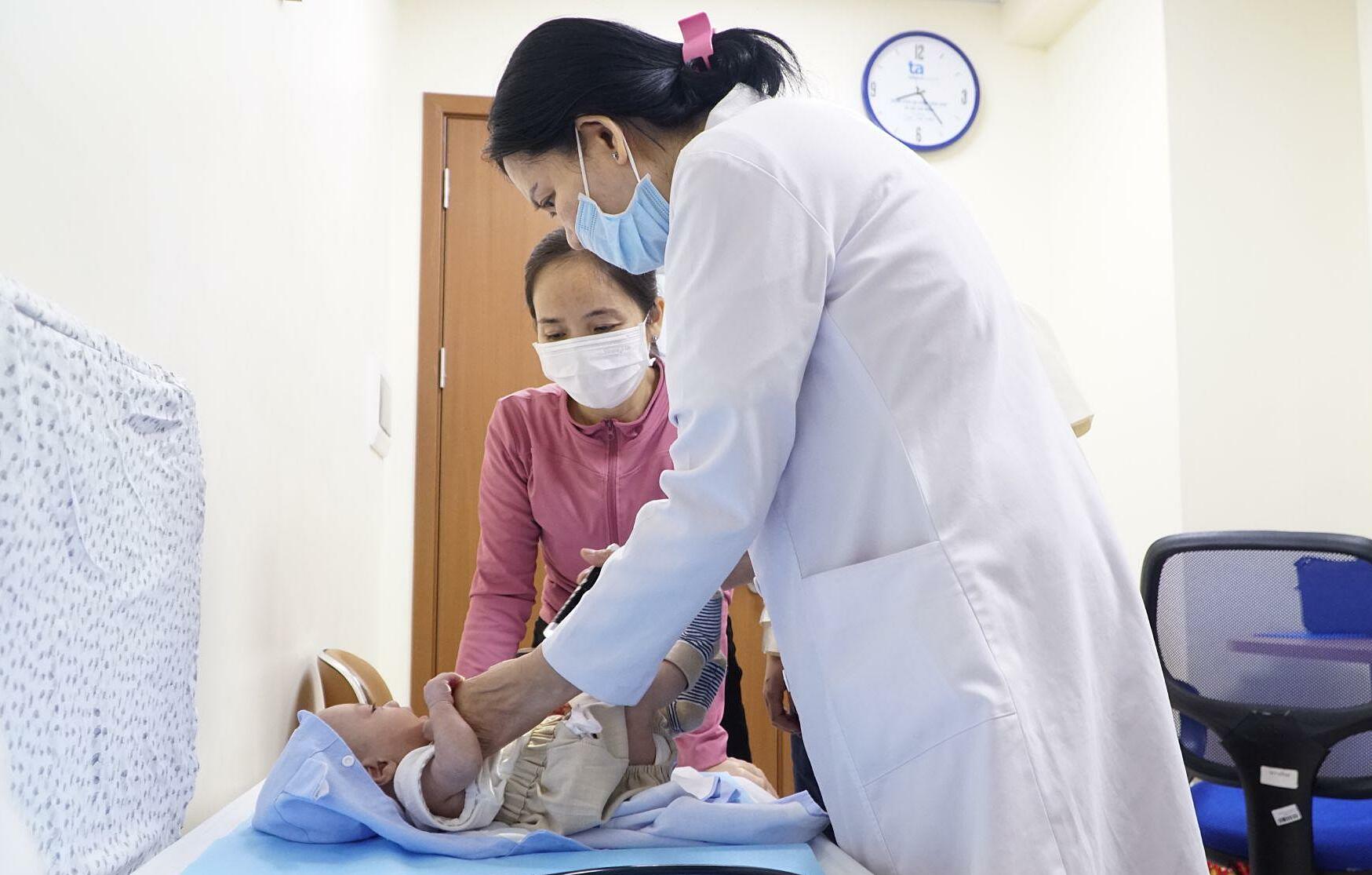 |
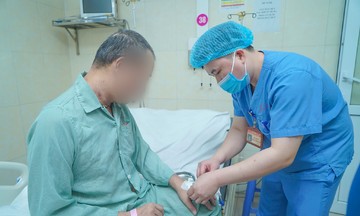
Doctor Phuong performs a comprehensive health check on the baby during a follow-up visit before Tet. Photo: Tam Anh General Hospital |
The baby's mother, 32 years old and pregnant for the first time, had been monitored for signs of fetal growth restriction since 16 weeks gestational age at another medical facility. At 25 weeks, she visited Tam Anh General Hospital TP HCM. Doctor Le Quang Hung, from the Fetal Medicine Center, diagnosed severe early-onset intrauterine growth restriction and an increased uterine artery pulsatility index.
Early-onset intrauterine growth restriction occurs when the fetal weight measured by ultrasound is below the 3rd percentile for gestational age, developing before 32 weeks. An increased uterine artery pulsatility index indicates that blood flow from the mother to the placenta is restricted, limiting oxygen and nutrient supply to the fetus. The mother also had a high risk of preeclampsia, for which she was taking Aspirin, and type 2 diabetes managed with insulin. The medical team assessed the pregnancy as complex, with a high risk of fetal distress and premature birth. The mother also faced potential severe preeclampsia or eclampsia, and diabetes complications.
To identify the cause of the fetal malnutrition in utero, doctors at the Fetal Medicine Center performed an amniocentesis on the mother. Specialized genetic testing revealed that the fetus carried a BRAF gene mutation (dominant - heterozygous), a KMT2B gene mutation (dominant - heterozygous), and a 0,5 mB deletion on chromosome number 7 (q21.2). The BRAF mutation can cause facial anomalies or physical developmental delays. The KMT2B mutation can lead to dystonia (muscle spasms, difficulty moving), short stature, and intellectual developmental delay. The microdeletion on chromosome number 7 was classified as having an unclear function, requiring further assessment of the baby's morphology.
"Global medical literature currently has no statistics on cases simultaneously carrying these three genetic mutations," Doctor Hung stated, adding that these genetic abnormalities complicate the prognosis. Genetic counselors supported the couple in investigating the origin of the mutations. Subsequent gene tests for both parents showed that two of the gene mutations were inherited from the mother, offering hope for the fetus's survival.
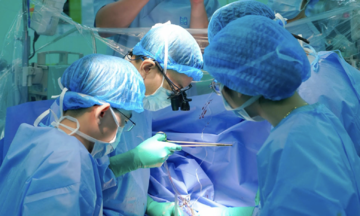
The mother was monitored weekly with Doppler ultrasound to assess the fetus's vital signs, continued optimal diabetes control with insulin, and prevention of preeclampsia risk. Doctors administered a full course of lung support injections and magnesium sulfate infusions to enhance fetal brain protection. At 31 weeks, the fetus began showing signs of distress. The Obstetrics and Gynecology, Fetal Medicine, and Neonatal teams held an interdisciplinary consultation, coordinating a cesarean section and intensive postnatal resuscitation.
The baby was born in mid-september last year, weighing 600 g, and had weak breathing, requiring immediate resuscitation in the delivery room. The team warmed the baby with a specialized thermal bag, provided CPAP respiratory support, and then transferred him to an incubator in the Neonatal Intensive Care Unit (NICU).
 |
The team transferred the baby to the NICU after resuscitation in the operating room. Photo: Tam Anh General Hospital |
"The baby was barely longer than a hand span; every breath revealed his ribs," the mother recalled the moment she met her son one day after birth.
Doctor Le Thi Ngoc Dung, from the Neonatal Center, explained that the baby suffered from respiratory failure and required non-invasive mechanical ventilation. The team provided intravenous feeding combined with early breast milk administration via a gastric tube. The baby responded to the treatment protocol, transitioning to oxygen therapy, discontinuing intravenous fluids, and fully feeding through the digestive tract from the 10th day after birth. The baby gained weight slowly and received enhanced high-energy nutrition in stages.
Seven weeks after birth (38 weeks gestational age), the baby began to develop the suck-swallow reflex, though it was slow and difficult, while other premature infants typically master this skill by 34 weeks. Doctor Phuong noted that the gene mutations likely affected the muscles in the mouth and esophagus, weakening the suck-swallow reflex. The baby followed a personalized feeding plan, including smaller, more frequent feeds and physical therapy to support oral motor skills.
The baby reached 2 kg more than two months after birth. "Every gram of weight gained was a miracle," Doctor Dung said. However, one night in early december, the baby suddenly developed labored breathing and chest indrawing. The SpO2 monitor screen turned red, and the reading dropped sharply. The medical team used a bag-mask device to provide oxygen, and chest X-rays and tests confirmed pneumonia. The baby received CPAP therapy combined with a two-week course of antibiotics, blood transfusions, continued aggressive nutritional support, and maintained suck reflex training.
Throughout the baby's care, the team of doctors and nurses provided psychological support to the family and instructed them on how to care for the baby, including holding him to look around and listen to people talk. Every day, the mother provided skin-to-skin contact, which helped the baby relax, reduce pain, and promote growth.
 |
Doctor Dung checks the baby's motor function. Photo: Tam Anh General Hospital |
Four months after birth, the baby weighed 3,1 kg, breathed well independently, and showed improved suck reflex. He received all necessary vaccinations and was discharged. During a follow-up visit before Tet, doctors noted no visual abnormalities, improved motor function, and stable progress in all other indicators. "This Tet is truly joyful because we have our son," the mother shared.
Ngoc Chau
| Readers can submit questions about neonatology here for doctors to answer |