Initially unaware it was shingles, Mr. Hung asked his wife to squeeze the fluid-filled blisters, causing the skin damage to spread. The severe pain eventually led him to seek medical attention, but by then, the blisters had formed large clusters on his back, accompanied by fever. He required over two months of treatment.
"When I had the illness, the pain felt like boiling water burns or an electric shock, forcing me to lie on my stomach," Mr. Hung recounted. "Even after the blisters disappeared, the persistent stinging pain continued, disrupting my sleep and appetite. Pain relievers offered no relief."
Concerned by her husband's condition, Mrs. Quy, Mr. Hung's wife, proactively visited VNVC Nha Be for medical consultation and to arrange a shingles vaccine. Aware of the risk of recurrence, and given Mr. Hung's underlying conditions of high blood pressure and diabetes, she promptly scheduled his vaccination to prevent severe complications.
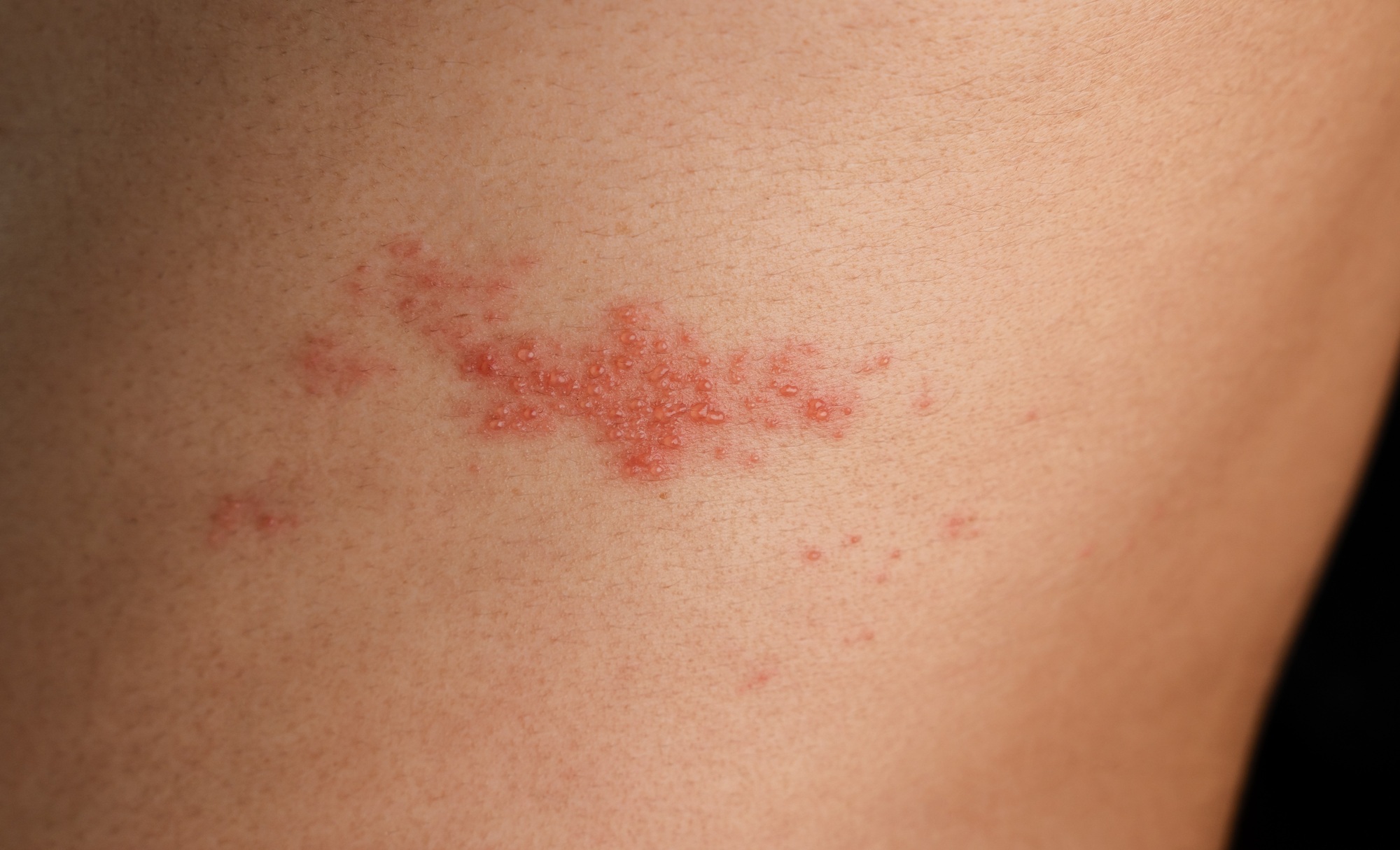 |
Burst shingles blisters can spread the infection to healthy skin. *Vecteezy*
Mrs. Thuy, 68, from Tan Ninh ward, Tay Ninh province, experienced shingles on her left bicep in late 12/2025. Initially, a red, throbbing area appeared on her arm. A doctor diagnosed shingles and prescribed oral and topical medication, but Mrs. Thuy, believing the condition was not serious, did not follow the treatment. Two days later, as blisters emerged in the painful area, causing electric shock-like sensations, she began taking and applying the medication.
Nearly three months later, the affected skin was no longer red, yet the throbbing sensation in her bicep persisted for months. The entire arm felt a "twitching" pain, particularly with weather changes. Despite trying various oral medications, her post-shingles pain showed no improvement. Mrs. Thuy expressed regret, believing that if she had followed her doctor's advice sooner, her condition might not have become so severe.
Doctor Nguyen Van Mac Toan, Medical Manager at VNVC Vaccination System, stated that post-herpetic neuralgia is the most common complication of shingles, potentially lasting months to years. This significantly impacts patients' health and quality of life. Approximately 22-46% of patients experience post-herpetic neuralgia for 2-10 years, with some enduring the pain indefinitely. Individuals who contract shingles on their head or face face a higher risk of developing this prolonged nerve pain.
Research indicates that the risk of post-shingles pain increases with age. About 30% of individuals over 60 experience nerve pain lasting over three months, and in some cases, for many years after the shingles rash has healed.
Chronic conditions such as diabetes, high blood pressure, and pulmonary, renal, or cardiovascular diseases can elevate the risk of developing shingles and, consequently, post-herpetic neuralgia. For instance, diabetic patients face a 24-38% increased risk of shingles and a 19% increased risk of post-herpetic neuralgia. The risk further escalates for individuals with multiple underlying health issues.
"Many individuals experience insomnia, anxiety, chronic fatigue, loss of appetite, weight loss, and even depression due to post-herpetic neuralgia," Doctor Toan explained. "Furthermore, shingles carries a risk of recurrence. Therefore, early vaccination is crucial for prevention."
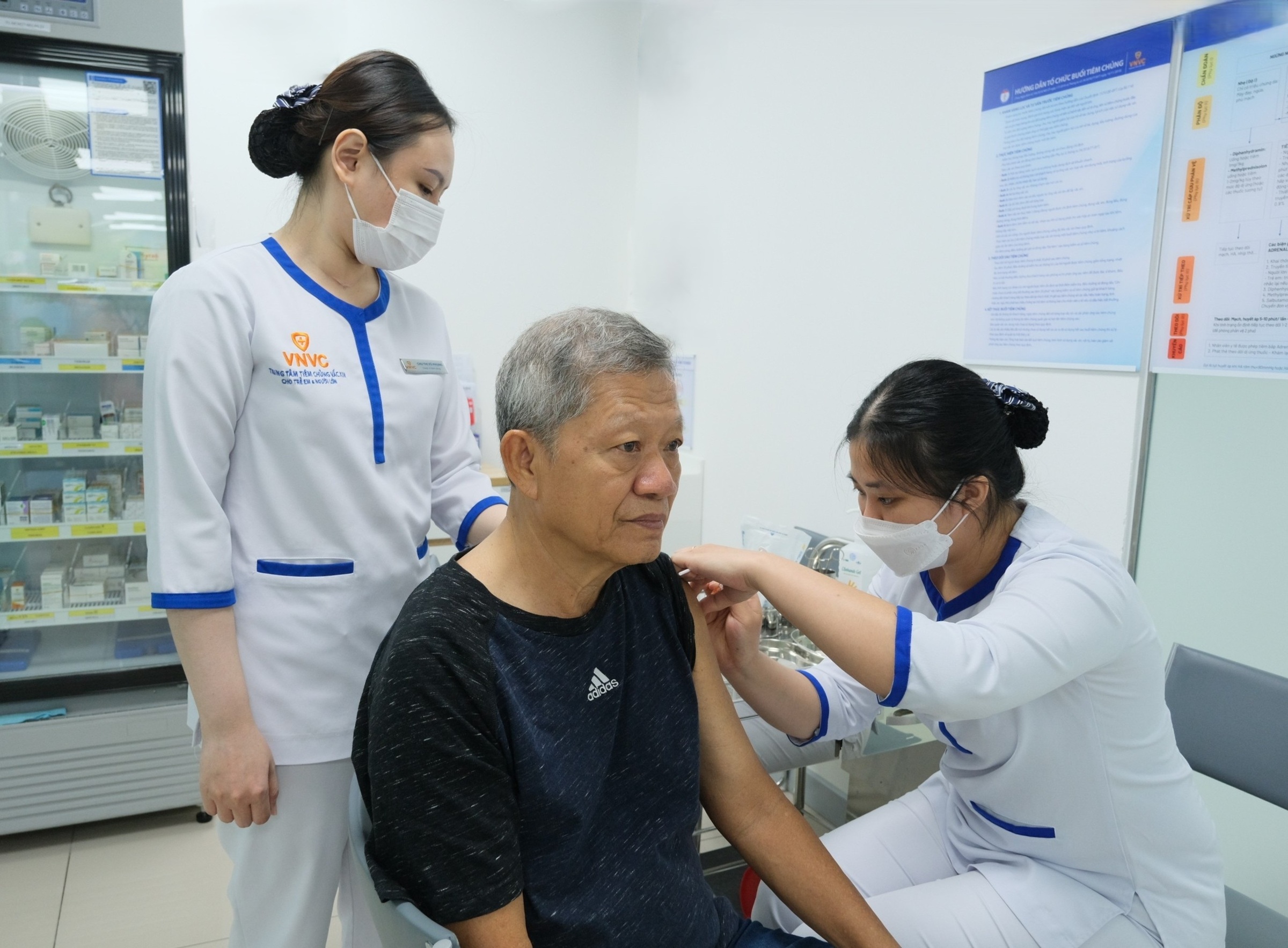 |
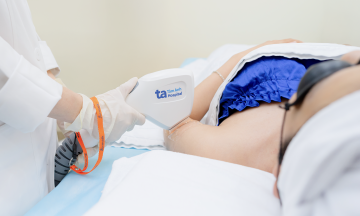
Elderly individuals receiving the shingles vaccine at VNVC. *Hoang Duong*
Currently, Vietnam offers a single shingles vaccine manufactured by GSK. This vaccine demonstrates over 97% efficacy in reducing shingles risk for individuals over 50, and up to 87% efficacy for immunocompromised individuals aged 18 and older. It also reduces the risk of post-herpetic neuralgia and other associated complications by more than 90%. The vaccination regimen involves two doses, administered 1-2 months apart, depending on the recipient's age and health status.
Shingles is caused by the same virus responsible for chickenpox. This virus remains dormant in the nerve ganglia of individuals who previously had chickenpox, reactivating when the body's immune system is compromised, leading to shingles.
Risk factors for shingles include advanced age, chronic conditions such as diabetes, high blood pressure, and pulmonary, renal, or cardiovascular diseases. Additionally, individuals with immunosuppressive conditions like HIV or lupus erythematosus, those taking immunosuppressants (e.g., post-organ transplant patients), and those experiencing prolonged stress are at increased risk.
Hoang An