According to Doctor Doan Vinh Binh of the Medical Information Center at Tam Anh General Hospital, Ho Chi Minh City, days when outdoor temperatures exceed 35 degrees Celsius, or continuous movement between hot environments and air-conditioned rooms, can trigger an acute hypertensive crisis.
An acute hypertensive crisis occurs when systolic blood pressure (the upper reading) suddenly exceeds 180 mmHg or diastolic blood pressure (the lower reading) exceeds 120 mmHg. This increases the risk of stroke and cardiovascular complications, especially for individuals with underlying health conditions. Doctor Binh noted that this condition can appear even in people not previously diagnosed with hypertension.
 |
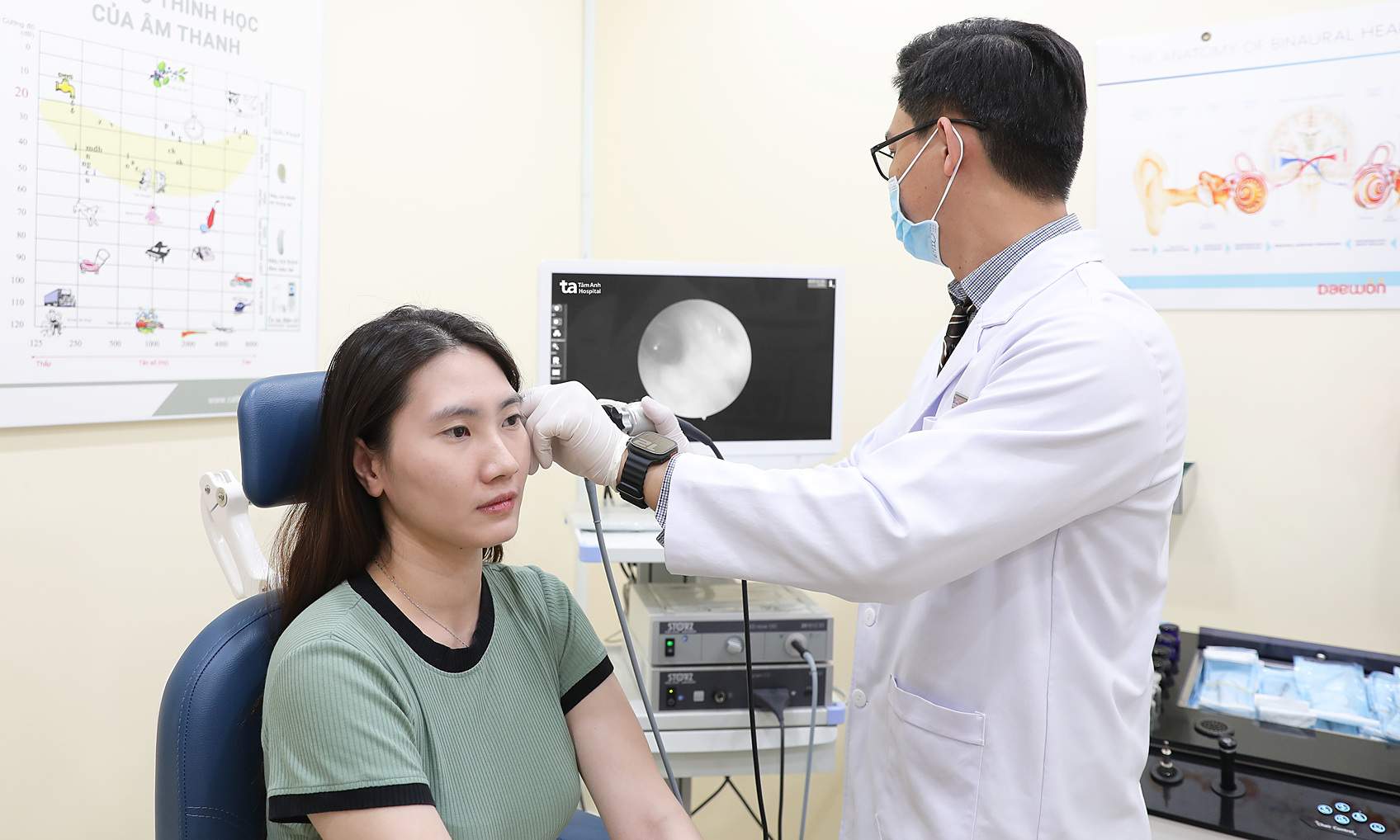
A medical staff member measures a patient's blood pressure. Illustration: Tam Anh General Hospital. |
Doctor Binh explained that when environmental temperatures rise, the body increases sweat production to cool down, leading to dehydration and electrolyte loss. This reduces circulating blood volume, causing blood to become thicker and circulate slowly. The body reacts by increasing heart rate and activating the sympathetic nervous system to maintain circulation and regulate body temperature, which can easily lead to high blood pressure. For individuals taking diuretics or who have hypertension, dehydration can be more severe, causing blood pressure to exceed safe levels and become difficult to control.
Sultry weather, causing restlessness and difficulty sleeping, can disrupt the natural nighttime blood pressure drop. This causes blood pressure to fluctuate more, easily leading to an acute hypertensive crisis.
Another factor is temperature differences, which also increase the risk of sudden blood pressure spikes. When exposed to outdoor sun, blood vessels dilate, but upon entering an air-conditioned room, they constrict rapidly, potentially causing an acute hypertensive crisis. Sudden temperature changes can trigger dangerous cardiovascular complications, especially in those with cardiovascular diseases, hypertension, or atherosclerosis.
A sudden hypertensive crisis manifests as restlessness, lightheadedness, dizziness, severe headache, nosebleeds, shortness of breath, chest pain, and palpitations. If these suspicious symptoms occur, individuals should rest in a cool, airy place, measure blood pressure, and monitor it. If they have daily hypertension medication, they should take it immediately, without waiting for the fixed daily dosage time. After about 15 minutes of taking the medication, re-measure blood pressure.
If there are signs of confusion, drowsiness, facial drooping, difficulty speaking, convulsions, limb weakness, or vision changes (eye pain, vision loss, blurred vision), the patient requires immediate emergency care, as these could be signs of a stroke.
If a patient shows signs of weak breathing, a weak pulse, or no pulse, cardiopulmonary resuscitation (CPR) should be performed. Simultaneously, call emergency services or transport the patient to the nearest medical facility.
Doctor Binh recommended preventing hypertensive crises during hot weather by following these measures: avoiding going outside during peak sun hours, between 10h and 16h; maintaining room temperature around 26-28 degrees Celsius and limiting sudden temperature changes, allowing the body time to adapt to avoid heat shock; drinking 2-2,5 liters of water daily, supplementing with oresol or electrolyte drinks if sweating heavily; and eating a bland diet, limiting spicy and hot foods, and increasing fresh fruits, vegetables, and tubers.
Individuals with blood pressure and cardiovascular conditions should monitor blood pressure at home, have regular check-ups, and adhere to treatment. Patients can supplement with natural nutrients beneficial for cardiovascular health, such as GDL-5 (extracted from South American sugarcane pollen), to help regulate blood lipids, protect blood vessels, and contribute to blood pressure stabilization.
Thai Thanh
| Readers can submit questions about cardiovascular health here for doctors to answer. |