Vaginitis is a common condition during pregnancy, potentially occurring at any stage. Elevated estrogen and progesterone levels lead to changes in the lower genital tract, including mucosal congestion, vaginal mucosal hypertrophy, increased cervical secretions, altered pH, and shifts in the vaginal microbiome. Local immune system adjustments also occur to adapt to pregnancy. These changes create a favorable environment for pathogenic microorganisms, such as anaerobic bacteria, yeast, or parasites, to thrive, increasing the risk of vaginitis.
 |
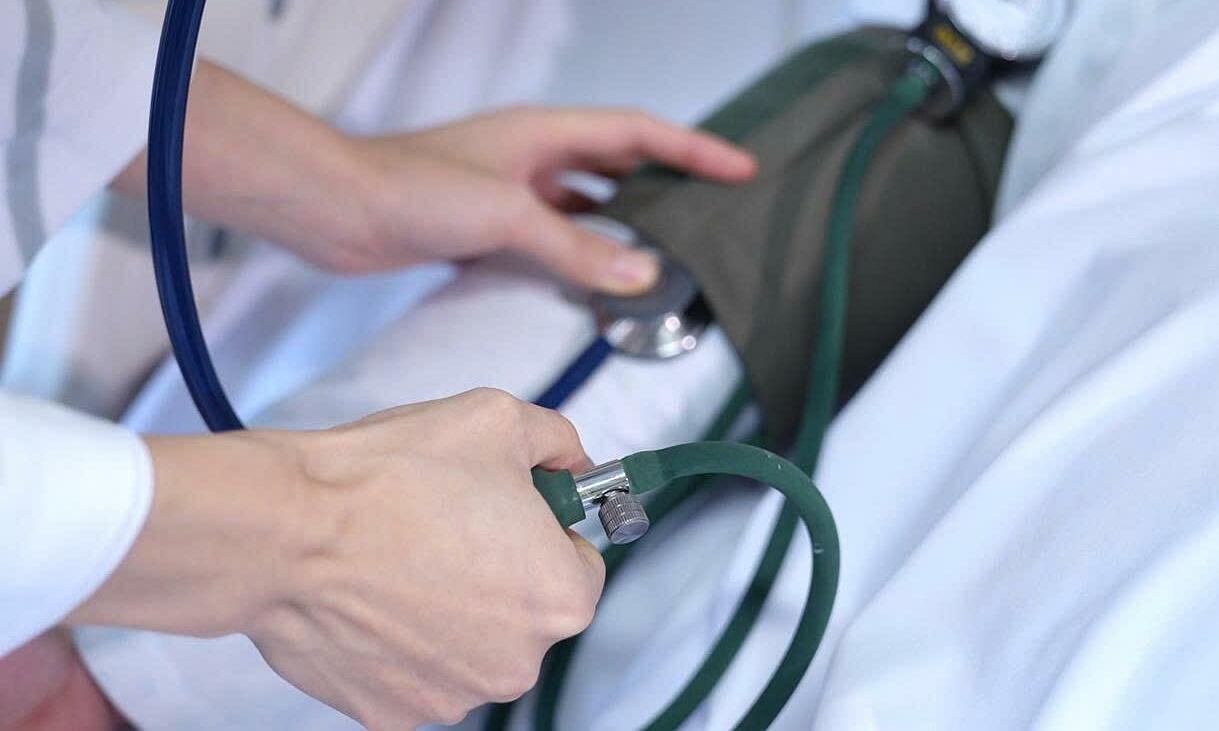
Dr. Nguyen Thi Minh Phuong advises on preventing vaginitis during pregnancy. Photo: Tam Anh General Hospital
Various factors can cause vaginitis in pregnant women. The most common is bacterial vaginosis (BV), an imbalance in the vaginal microbiome where anaerobic bacteria overgrow. Symptoms often include thin, gray-white discharge with a fishy odor, particularly noticeable after intercourse.
Candida infection is another frequent cause during pregnancy due to increased glycogen in the vaginal environment. This typically results in thick, white, lumpy discharge, resembling cottage cheese, accompanied by itching and burning in the vaginal and vulvar areas.
Trichomonas can also cause vaginitis, presenting with yellow-green, frothy, foul-smelling discharge. Group B Streptococcus (GBS) may colonize the vagina or rectum of pregnant women without clear symptoms, but poses a risk of transmission to the baby during childbirth, potentially causing severe infections in newborns.
For pregnant women, vaginitis causes itching, burning, discomfort, and can disrupt daily life. If left untreated, it may spread to upper reproductive organs like the uterus or pelvic region. Some cases increase the risk of premature rupture of membranes, miscarriage, or preterm birth before 37 weeks.
For the fetus, certain vaginitis pathogens, such as bacteria, Trichomonas, or sexually transmitted infections, can contribute to early labor, preterm birth, low birth weight, or postpartum respiratory issues. In rare cases, Group B Streptococcus can lead to sepsis, pneumonia, or meningitis in newborns.
During pregnancy, vaginal discharge typically increases due to hormonal changes. Normal physiological discharge is usually clear or slightly cloudy white, odorless or with a very mild odor, and does not cause itching. However, pregnant women should seek early medical attention if they notice unusual signs: abnormally excessive discharge; lumpy or discolored discharge (yellow, green, gray); a fishy or foul odor; or accompanying itching, burning, or redness in the vaginal and vulvar areas.
For a pregnant woman at 25 weeks experiencing white, lumpy discharge, itching, and a foul odor, vaginitis is highly likely, most commonly a candida infection. However, clinical symptoms alone cannot precisely identify the cause. Therefore, it is advisable to visit a hospital for an examination, including a wet mount test of vaginal discharge or other necessary tests to determine the causative agent. Based on the results, the doctor will prescribe appropriate and pregnancy-safe vaginal suppositories or oral medication.
Pregnant women should avoid self-medicating with vaginal suppositories or oral drugs, as some medications are unsuitable or require specific dosages during pregnancy. To prevent vaginitis, maintain clean, dry intimate hygiene, gently cleanse without douching, wear cotton underwear and change it when damp, and limit harsh or strongly scented feminine washes. Regular prenatal check-ups are essential, or seek immediate consultation if discharge becomes excessive, foul-smelling, discolored, lumpy, or accompanied by itching or burning in the genital area.
Dr. Nguyen Thi Minh Phuong
Obstetrics and Gynecology Center
Tam Anh General Hospital System, TP HCM
| Readers can submit questions about obstetrics and gynecology here for a doctor's response. |