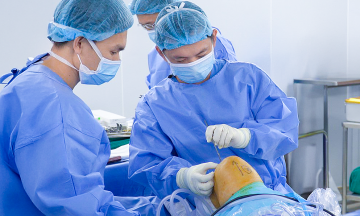
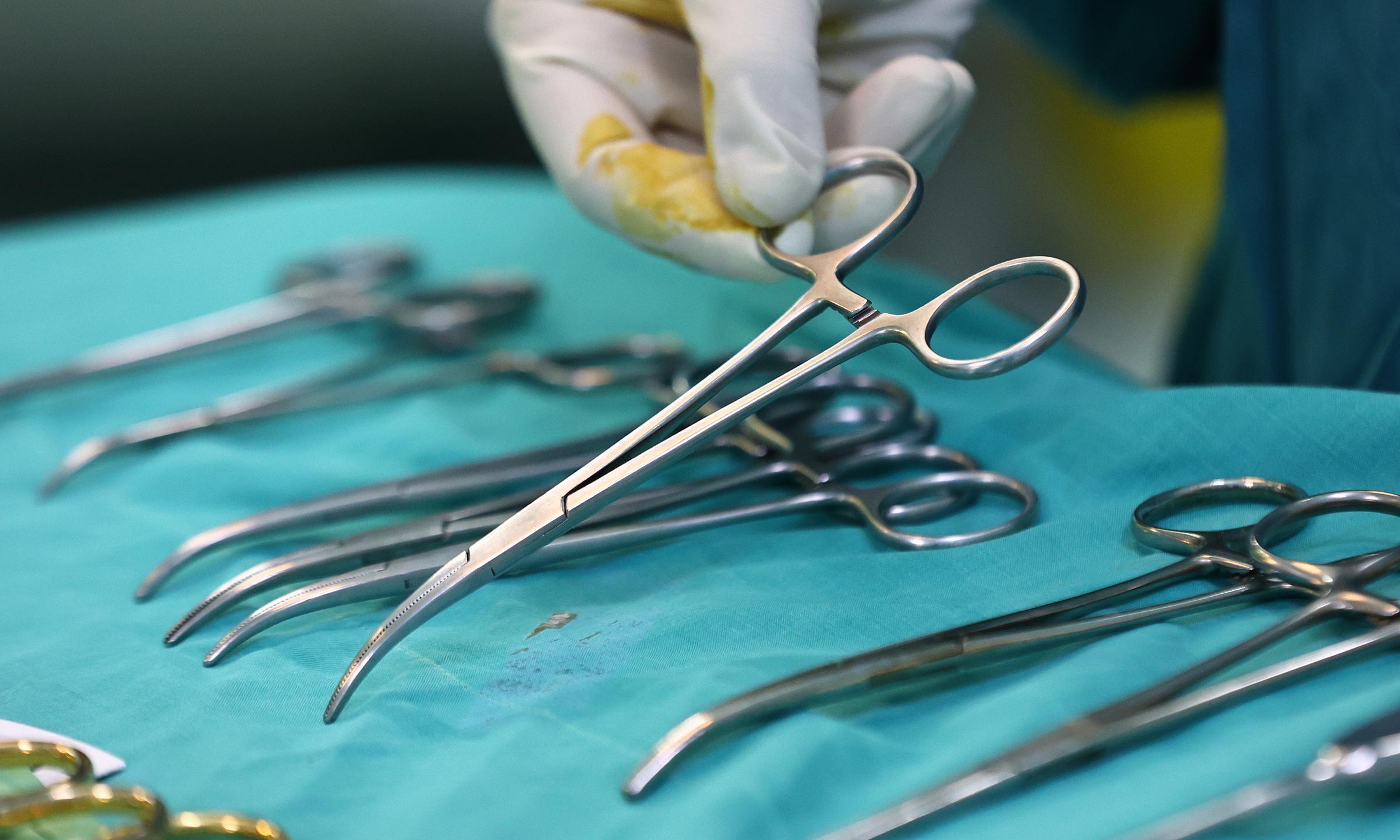
On the morning of 31/3, the patient was discharged with stable health after a life-threatening surgery. Previously, she had two normal births and a history of ectopic pregnancy, with her left fallopian tube removed 11 years ago. Recently, after forgetting to take birth control pills, she experienced a missed period and a positive pregnancy test. As her abdominal pain intensified, she sought examination at Long Khanh Hospital, where an abdominal pregnancy of approximately 10 weeks was suspected. She was urgently transferred to Tu Du Hospital on the afternoon of 26/3.
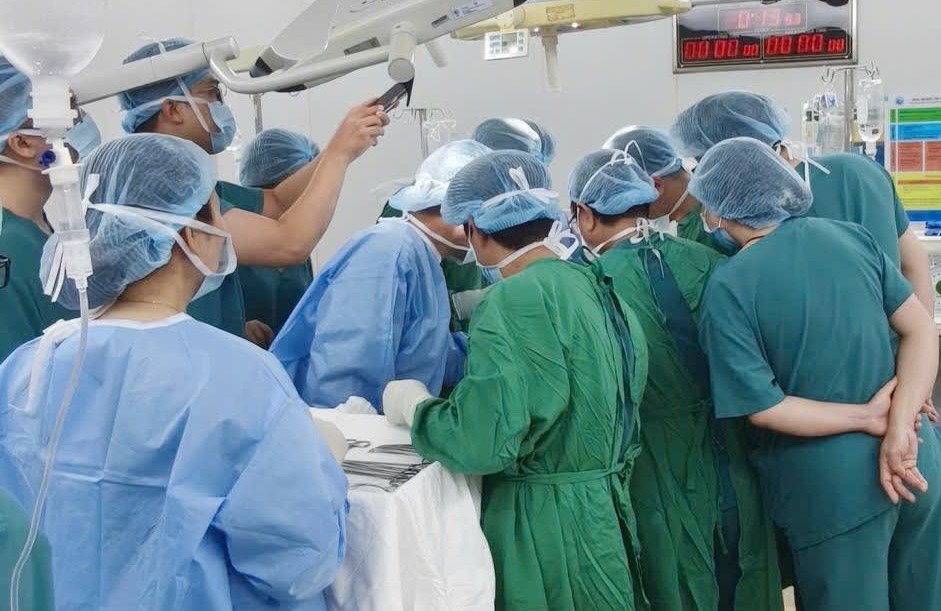 |
Doctors performing emergency surgery on the patient at midnight at Tu Du Hospital. *Photo: Hospital provided*
Doppler ultrasound and MRI scans revealed a 10-11 week live fetus in a very rare retroperitoneal position, close to the abdominal aorta. The pregnancy mass was adhered to the aortic wall by approximately 10 mm, located below the left renal artery bifurcation, and showed signs of progressive hemorrhage. This is a rare form of ectopic pregnancy, carrying a high risk of major blood vessel rupture and rapid death if not intervened promptly. Recognizing the complexity of the case, doctors activated an inter-hospital red alert, inviting a vascular team from Cho Ray Hospital for a joint consultation to devise an optimal plan.
Near midnight on 26/3, the surgery began. The team observed diffuse retroperitoneal hemorrhage, with the pregnancy mass situated close to several vital structures, including the abdominal aorta, renal blood vessels, and the left ureter. Doctors performed meticulous dissection, millimeter by millimeter, to avoid damaging major blood vessels.
During the dissection, doctors skillfully separated the pregnancy mass from the aorta while preserving the renal blood vessels and the left ureter. Although there was minor bleeding, the situation was controlled promptly. Ultimately, the entire pregnancy mass and placenta were completely removed.
The surgery lasted three hours, with blood loss estimated at approximately 500 ml, so the patient did not require an additional transfusion. Two days post-surgery, the patient was conscious, had stable vital signs, a dry incision, and was able to eat, drink, and walk normally. The success of the surgery highlights the effectiveness of inter-hospital red alert coordination model at Ho Chi Minh City's tertiary hospitals.
Le Phuong