Healthcare costs are rising sharply, particularly due to non-communicable chronic diseases such as hypertension, diabetes, cardiovascular conditions, and metabolic disorders. These conditions are placing an increasing strain on the health insurance fund, stated Nguyen Duc Hoa, Deputy Director of Vietnam Social Security, at the "Towards a Sustainable Health Insurance System in Vietnam" workshop. The event was organized by Vietnam Social Security in collaboration with the Danish Embassy and Novo Nordisk Vietnam on 16/4 in Hanoi.
A report by Vietnam Social Security presented at the workshop revealed that in 2025, nearly 98 million people nationwide participated in health insurance, achieving coverage for over 95% of the population. The total number of health insurance medical examinations and treatments exceeded 195 million, a 6.5% increase from the previous year, while requested payments amounted to 166.4 trillion dong, an increase of over 16%.
Notably, a significant portion of these costs stems from chronic diseases. The health insurance fund currently covers nearly 8 million people with hypertension, over 3.3 million diabetes patients, over 1.1 million individuals with chronic respiratory illnesses, and approximately 500,000 cancer patients. The non-communicable disease group alone recorded approximately 51 million visits, with total expenditures nearing 20 trillion dong, marking an increase of almost 18%.
 |
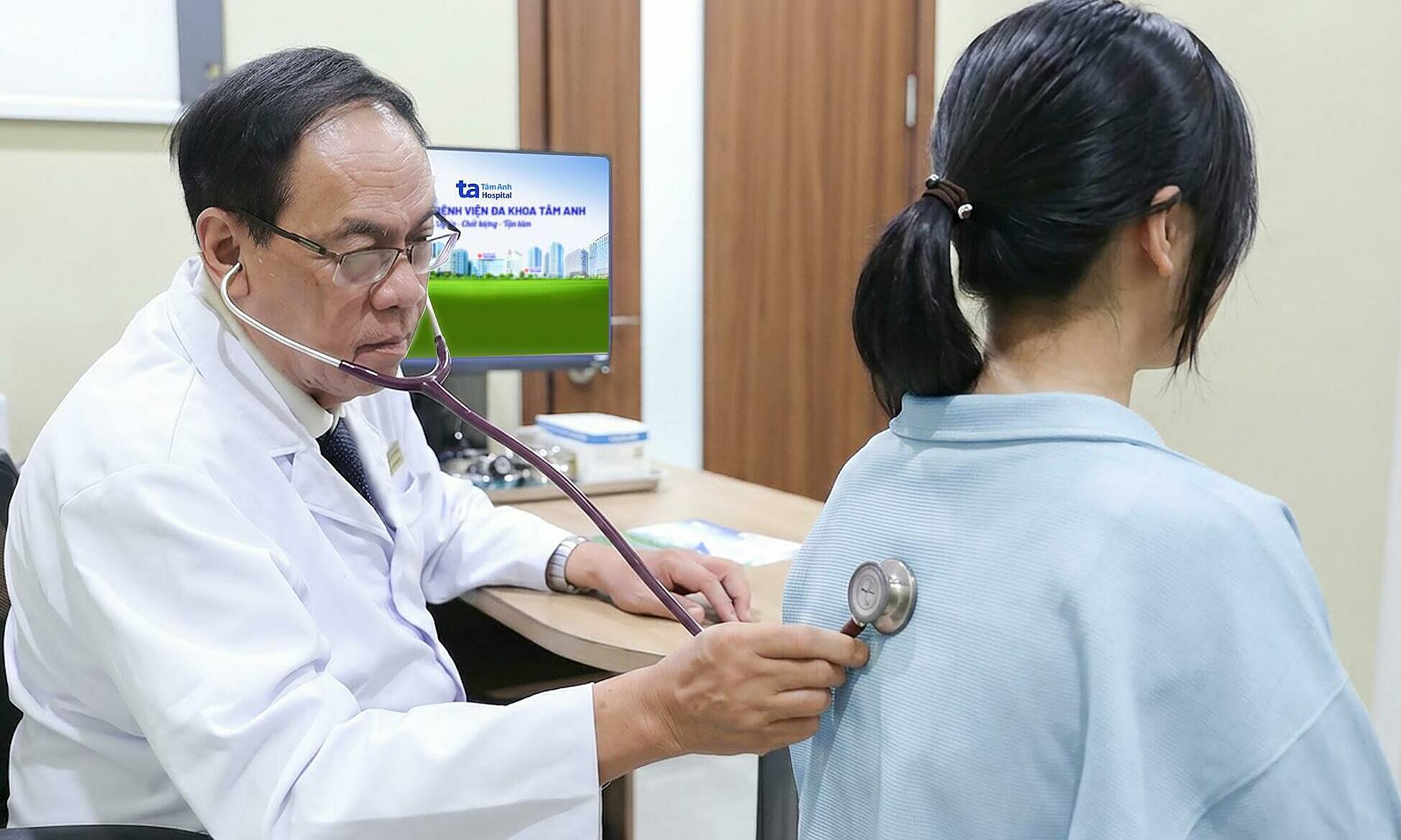
Residents have their blood pressure checked at Tang Nhon Phu ward health station, april 2026. Photo: Quynh Tran |
Associate Professor Vu Thi Thanh Huyen, Head of the Department of Endocrinology – Musculoskeletal at the National Geriatric Hospital, explained that diabetes and metabolic disorders rarely appear in isolation. They are often accompanied by multiple cardiovascular and kidney diseases, which significantly increase treatment costs and exert immense pressure on the health insurance fund. A concerning aspect in Vietnam is that most treatment costs are incurred not in the early stages, but in managing complications.
"Patients often do not suffer from a single illness but present with two to three comorbidities like cardiovascular disease, kidney disease, and metabolic disorders," said Associate Professor Huyen. She cited that approximately 55% of diabetes patients experience cardiovascular complications, and one-third progress to chronic kidney disease. Over 80% of cases are diagnosed at a late stage, causing treatment costs to multiply, sometimes requiring dialysis or intensive intervention.
A primary reason for these escalating costs is the low rate of disease control. Currently, under 30% of patients achieve their blood sugar targets, which heightens the risk of complications and leads to substantial cumulative costs. Overweight and obesity are prominent risk factors, with approximately 90% of type 2 diabetes patients exhibiting these conditions. This is linked to sedentary lifestyles, high-energy diets, and work-related stress.
Erik Wiebols, General Director of Novo Nordisk Vietnam, stated that chronic diseases currently account for over 70% of the disease burden and over 80% of deaths in Vietnam. This highlights the urgent need to shift focus from treatment to early, comprehensive, and sustainable prevention and disease management. Effective control of metabolic disorders such as obesity, diabetes, cardiovascular disease, and chronic kidney disease not only helps reduce long-term complications but also optimizes health insurance resources, lowers societal costs, and improves patients' quality of life.
International experience also demonstrates the effectiveness of this approach. Several countries have implemented risk stratification models and early interventions for medium-risk groups to prevent severe progression, thereby reducing long-term treatment costs. In Thailand, for example, non-communicable diseases like obesity and diabetes are creating a massive economic burden, necessitating a shift in healthcare policy towards early prevention and comprehensive population management.
Associate Professor Petch Rawdaree, President of the Federation of Non-Communicable Disease Prevention Associations (Thailand), elaborated on Thailand's approach, which stratifies the population into three risk groups: low risk (approximately 50%), medium risk (35-40%), and high risk. The medium-risk group is considered a critical "interception point," currently accounting for approximately 30-35% of healthcare costs. In contrast, the high-risk group, despite comprising only about 5% of the population, bears 40-55% of total healthcare expenditures.
Thailand's policy, therefore, simultaneously focuses on multiple pillars: enhancing public health, strengthening grassroots healthcare, early screening, continuous management, and mobilizing participation from across society, from government to the private sector. "The most effective strategy is to prevent them from progressing to severe stages, rather than solely focusing on treating those who already have complications," he said.
Le Nga