Doctor Nguyen Duc Thong, Head of the Endoscopy Department at Nguyen Trai Hospital, stated on the sidelines of an international conference on 15/4 that most patients at the hospital typically wait for symptoms such as abdominal pain, bloody stools, anemia, or weight loss before seeking medical examination.
According to the doctor, by the time the body "speaks out" with symptoms, the disease is often in an advanced stage. At this point, even with surgery, cancer cells may have already metastasized to other organs, significantly reducing the prognosis for survival.
To mitigate the risk of digestive cancer progression, individuals should shift from a "wait until sick to treat" mindset to proactive screening while healthy. The recommended age to begin stomach and colon endoscopy is 40. After the initial endoscopy, doctors will establish an appropriate follow-up schedule based on the results. High-risk individuals, such as those with Helicobacter pylori (HP) infection, atrophy, or intestinal metaplasia, require more frequent endoscopic examinations, approximately every one to two years. Crucially, those with a family history of digestive tract cancer should begin screening even earlier.
Early endoscopy offers significant benefits by enabling timely detection and management of precancerous lesions. Doctor Thong cited HP infection as a primary cause of stomach cancer, which can progress through stages of atrophy, intestinal metaplasia, and early cancer. For the colon, adenomatous polyps carry a high risk of developing into malignant tumors if not detected and removed promptly.
When polyps are detected during an endoscopy, doctors can remove them immediately. Patients typically experience a full recovery, are discharged the same day, thereby avoiding major surgery and reducing their future risk of colon cancer.
 |
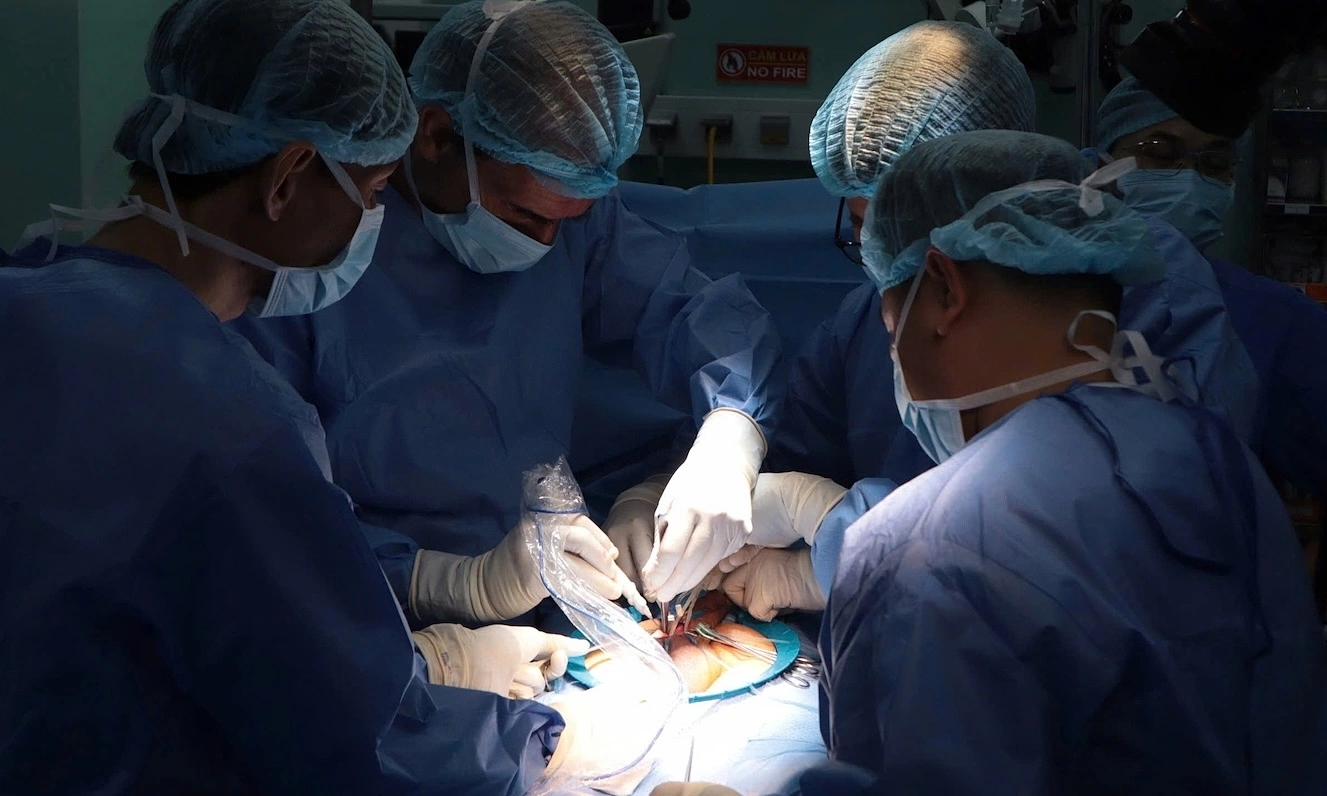
Digestive endoscopy doctors at Nguyen Trai Hospital. *Photo: Hospital provided*
Beyond individual initiative, the early diagnostic capabilities of healthcare facilities are also crucial. The hospital is actively implementing modern techniques such as chromoendoscopy and magnifying endoscopy to enhance lesion detection. Endoscopic ultrasound is also being further developed, aiding in the precise assessment of tumors within the digestive tract wall, identifying the depth of lesions for biopsy, and informing treatment plans.
Doctor Le Thanh Phong, Deputy Director of Nguyen Trai Hospital, emphasized that digestive endoscopy plays an increasingly pivotal role in early diagnosis, lesion assessment, and minimally invasive treatment. Updating medical advancements and expanding international cooperation are central strategies to enhance professional expertise and improve the quality of treatment.
At the conference, doctor Kinoshita Koshi, Head of the Department of Gastroenterology and Endoscopy at Kyoto Miniren Central Hospital (Japan), provided direct academic exchange, assisting domestic doctors in refining and upgrading endoscopic submucosal dissection (ESD) techniques to more difficult and specialized levels.
This endoscopic method treats early-stage cancer, removing lesions while preserving the stomach, limiting complications, shortening hospital stays, and reducing costs. In Japan, ESD is widely adopted due to effective screening programs. Previously, individuals aged 40 and above underwent annual barium X-rays followed by endoscopic screening. More recently, as HP infection rates have decreased, Japan has observed a gradual reduction in stomach cancer cases and has shifted to periodic screening every two to three years for individuals over 50.
According to doctors, anesthetized endoscopy has become common, making the procedure gentle and painless. This helps alleviate apprehension and encourages people to proactively undergo screening to protect their health.
Le Phuong