Male sterilization, commonly known as a vasectomy, is a surgical procedure that involves cutting or tying the vas deferens to prevent sperm from traveling from the testicles into the semen. Doctor Nguyen Cong Minh from the Center for Reproductive Support at Tam Anh General Hospital - District 8, states that this method is safe and over 99% effective as contraception. However, the rate of men undergoing vasectomy remains low, partly due to persistent misconceptions about the procedure.
**Myth one: vasectomy impairs male sexual function.**
Male sexual function primarily depends on testosterone, produced by Leydig cells in the testicles, and the nervous system. Vasectomy only affects the vas deferens, which transport sperm, without impacting the testicles, endocrine system, or erection mechanism. Consequently, testosterone levels remain unchanged, erections and ejaculation occur normally, and sexual pleasure is unaffected.
Some studies also indicate that after a vasectomy, many men experience greater psychological comfort due to the absence of pregnancy worries, which can indirectly improve the quality of their sexual life.
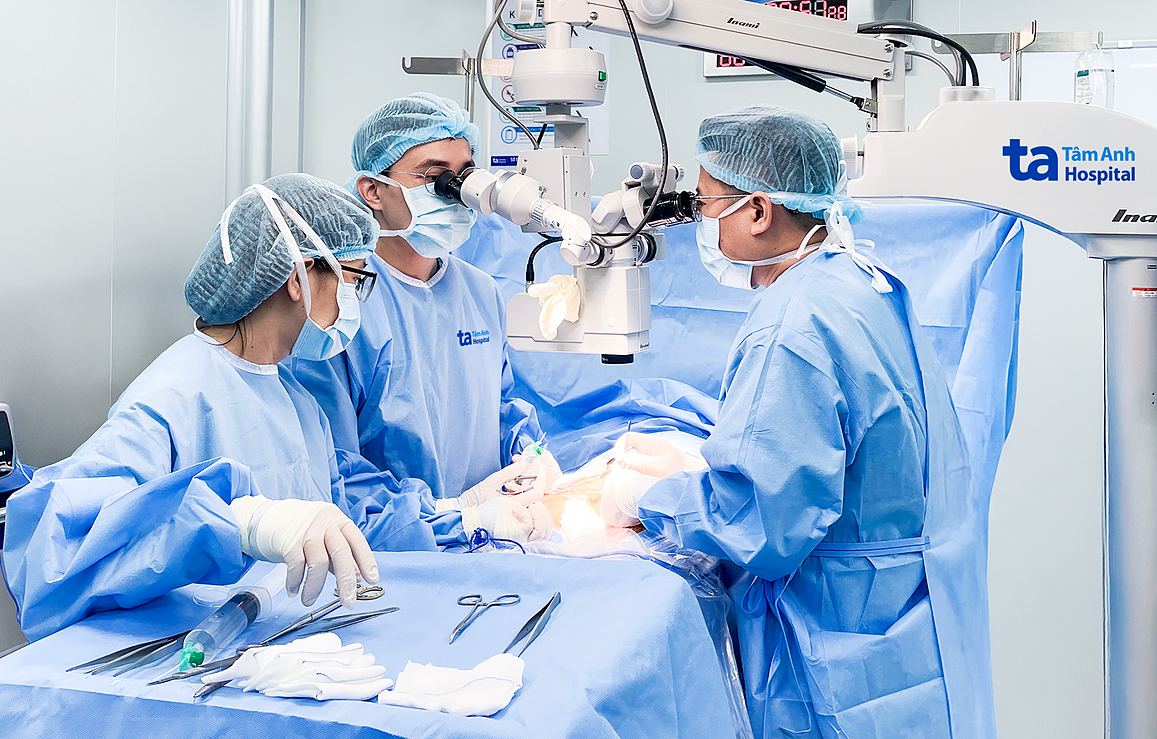 |
Doctor Minh (center) performs a vasectomy on a patient. Illustration: Tam Anh General Hospital. |
**Myth two: inability to ejaculate after vasectomy.**
Semen is primarily a mixture of fluid from the seminal vesicles (accounting for about 60-70%) and the prostate gland (20-30%), with sperm making up only 2-5%. After a vasectomy, the testicles continue to produce sperm, but it cannot pass through the ligated segment of the vas deferens. White blood cells destroy this sperm in the epididymis. The volume of ejaculate remains almost unchanged, so ejaculation occurs normally; the only difference is that the semen no longer contains sperm.
**Myth three: permanent loss of fertility.**
Many believe that after a vasectomy, men cannot regain the ability to father children. However, Doctor Minh explains that fertility can be restored through a vasovasostomy, a procedure to reconnect the vas deferens. Success depends on factors such as the time elapsed since the vasectomy (longer periods reduce success rates), scar tissue at the ligation site, sperm quality, and testicular function. The success rate for vasovasostomy can reach 90%.
 |
Doctor Minh consults with a man. Illustration: Tam Anh General Hospital. |
**Myth four: inability to undergo IVF.**
Even after a vasectomy, the testicles continue to produce sperm, though it cannot exit naturally. If a couple wishes to conceive, doctors can retrieve sperm directly from the testicles or epididymis surgically. This sperm can then be used for in vitro fertilization (IVF), often combined with intracytoplasmic sperm injection (ICSI). The advantage of this approach is that the patient does not need a vasectomy reversal, and sperm quality can be controlled.
**Myth five: vasectomy causes cancer.**
Doctor Minh cites several studies indicating that male sterilization does not alter sex hormone levels, nor does it affect cardiovascular function, metabolism, or cancer risk. While some rare complications can occur, such as scrotal hematoma, local infection, or swelling, these are manageable with various treatments.
Doctor Minh emphasizes that vasectomy is an effective and safe contraceptive method. Fertility restoration is possible, depending on individual circumstances and the specific technique used. Men considering vasectomy should consult a specialist to receive comprehensive advice on the procedure, ensuring the preservation of their physiological and reproductive functions in the future.
Dinh Lam