The rectum, the final 11-15 cm segment of the large intestine located just above the anus, stores stool before excretion. Rectal cancer develops when mucosal cells in the rectum mutate and proliferate abnormally, forming a tumor. Without timely detection and treatment, these tumors can deeply invade the intestinal wall, spread to adjacent organs, or metastasize to the liver, lungs, and other distant sites.
Doctor Luu Van Dat, a Master of Science from the Department of General Surgery at Tam Anh General Hospital Hanoi, states that surgery is a common treatment for rectal cancer, particularly in early stages. The primary goal is to completely remove the tumor, adjacent lymph nodes, and any metastatic tissues. Surgery also addresses complications like intestinal obstruction, bleeding, and pain caused by large, invasive tumors.
Doctors select the most suitable treatment based on the disease stage, tumor size, location, and the patient's overall health. This approach aims to preserve natural bowel function as much as possible.
Endoscopic mucosal resection and submucosal dissection
For tumors confined to the mucosal layer or superficially invading the submucosal layer of the rectum, doctors may employ minimally invasive techniques such as endoscopic mucosal resection (EMR) or endoscopic submucosal dissection (ESD). These procedures use specialized endoscopic instruments inserted through the anus to dissect and remove the lesion. This approach avoids open abdominal surgery or rectal resection, thereby preserving anatomical structure and gastrointestinal function. Patients often avoid a colostomy and maintain normal bowel function post-treatment.
Transanal endoscopic surgery
When early-stage rectal cancer tumors have invaded deeper through the mucosal layer, doctors may recommend transanal endoscopic surgery, such as transanal excision (TAE) or transanal minimally invasive surgery (TAMIS). These procedures remove the lesion along with a margin of healthy surrounding tissue to ensure clear margins. The rectal wall is then sutured during the same operation. Doctor Dat notes that patients usually avoid a colostomy and can maintain natural bowel function, as these procedures do not require removing a large rectal segment.
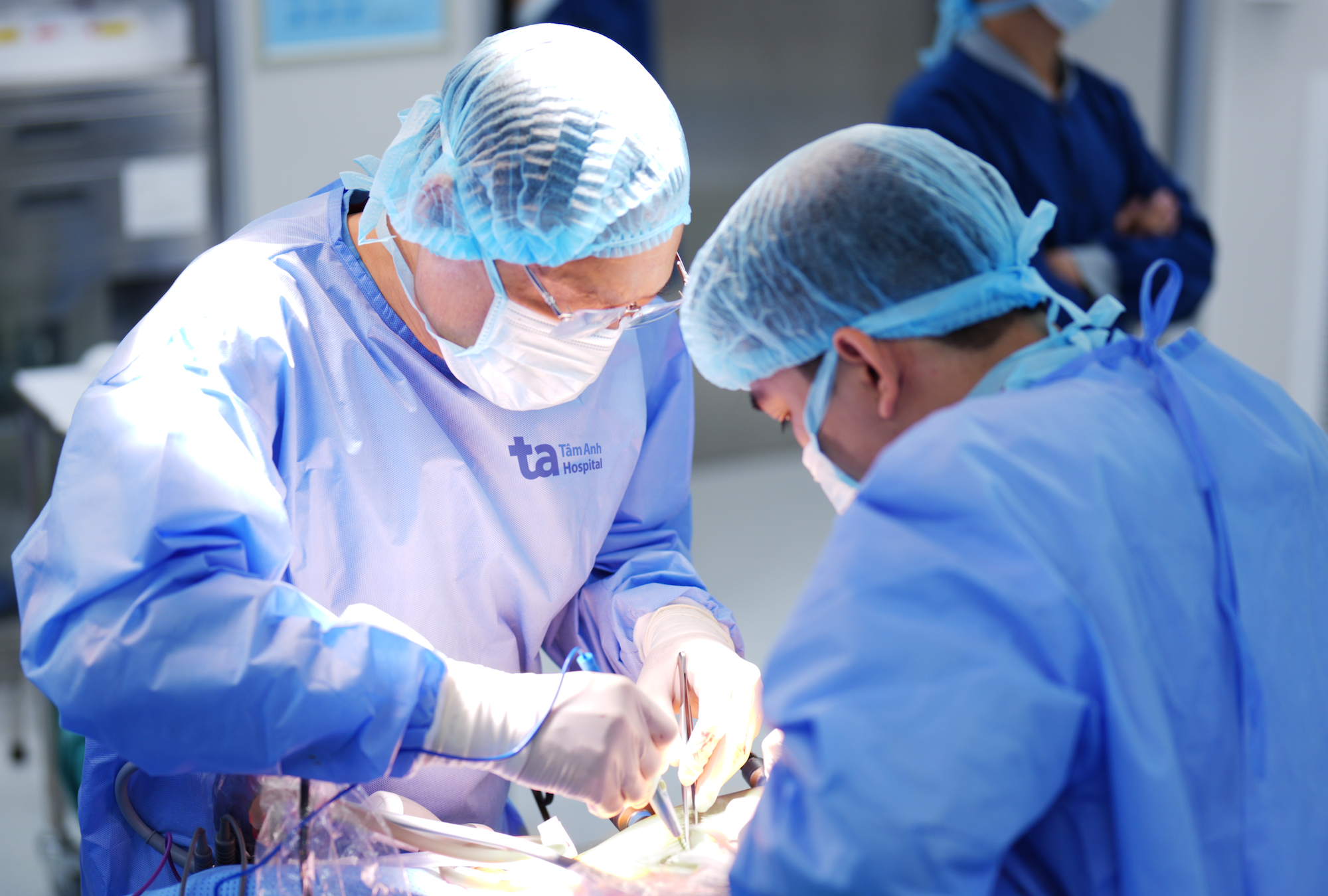 |
Doctors perform surgery on a rectal cancer patient. Photo: Tam Anh General Hospital |
Sphincter-preserving rectal resection
For advanced rectal cancer with deep invasion into the rectal wall and a tumor located far from the anus, sphincter-preserving rectal resection methods like total mesorectal excision (TME) or low anterior resection (LAR) are performed. This involves removing the tumor-bearing rectal segment, along with surrounding fatty tissue and lymph nodes. The remaining colon is then directly connected to the residual rectum or anal canal, preserving digestive tract continuity and natural bowel function.
Doctor Dat explains that for rectal tumors located near the anus or those potentially affecting anal sphincter function, doctors might recommend pre-operative chemotherapy or radiation therapy to reduce tumor size. A good response to this neoadjuvant treatment increases the likelihood of preserving the anus and maintaining natural bowel function.
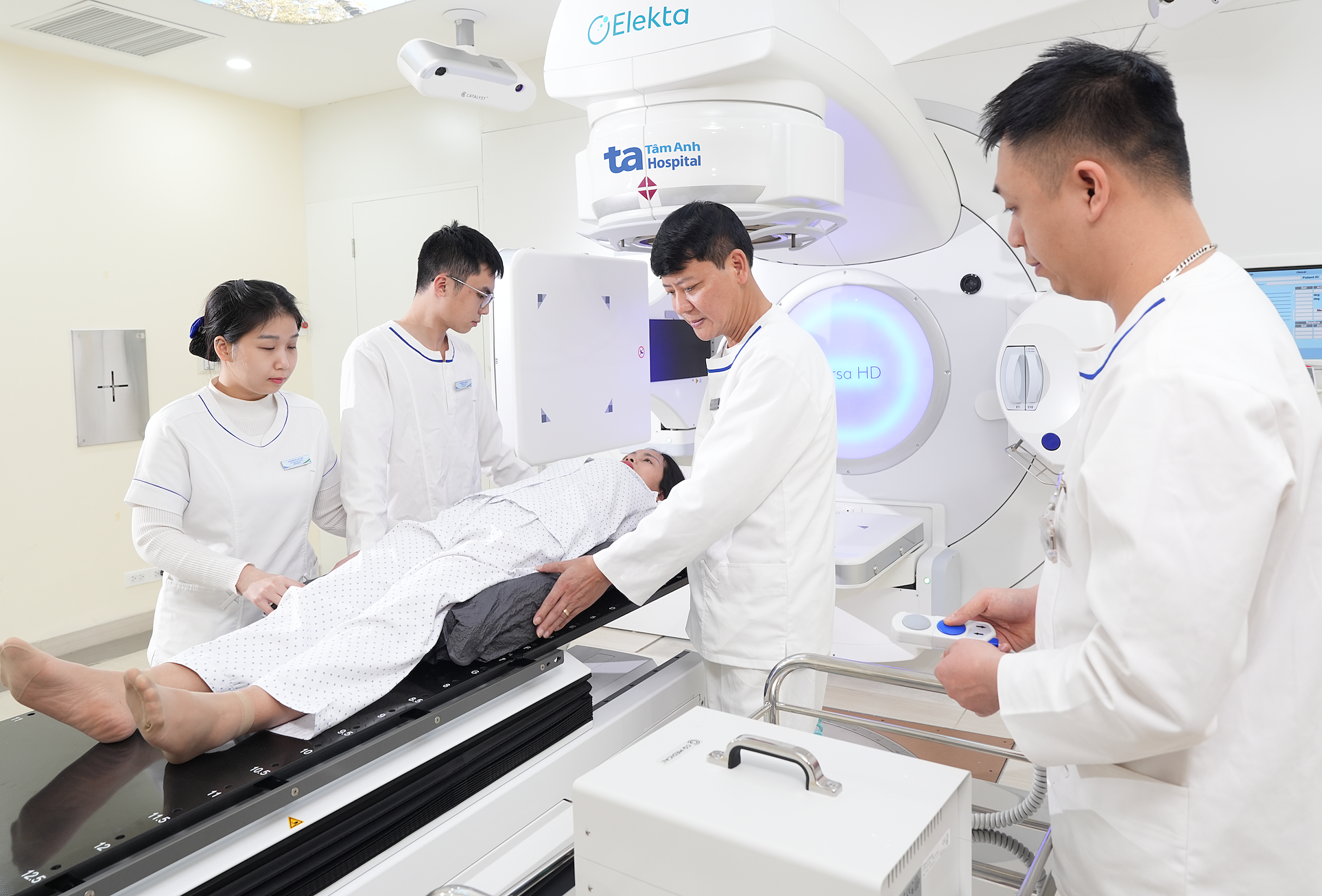 |
A rectal cancer patient undergoes neoadjuvant radiation therapy before surgery. Photo: Tam Anh General Hospital |
Doctor Dat highlights that advancements in surgical techniques and multimodal treatment have significantly improved the prognosis for rectal cancer patients. Early detection, appropriate treatment selection, and diligent post-treatment follow-up are crucial for enhancing treatment effectiveness, improving quality of life, and extending patient survival.
Thanh Long
| Readers can submit questions about digestive diseases here for doctors to answer. |