Response:
Infants often spit up or have mild choking during feeding, which can be linked to physiological gastroesophageal reflux. Severe milk choking can lead to respiratory distress or aspiration of milk into the lungs, potentially causing airway obstruction if not addressed promptly.
The primary causes of infant milk choking are immature swallowing and breathing reflexes, strong milk flow, incorrect feeding positions, or feeding while the infant is sleeping. When choking mildly, infants typically cough a few times and spit up milk. Below are the appropriate responses based on the severity.
For mild infant milk choking: If an infant is feeding or has just finished feeding, coughs a few times, possibly spits up milk, breathes normally, has pink lips, a normal complexion without bluish discoloration, cries, and responds well, they usually recover quickly within a few seconds to less than one to two minutes. This indicates a transient swallowing-breathing coordination disorder.
Parents should stop feeding the infant and place their head to one side (left or right) to help them spit up or cough out the milk. If milk spills from the infant's mouth or nose, gently wipe it with a soft cloth without reaching into their throat. Afterwards, gently pat the infant's back between their shoulder blades. Once the infant coughs and breathes steadily, they are stable, and parents can resume feeding, ensuring the infant's head is elevated higher than their body.
For severe infant milk choking: In cases of severe milk choking, parents should call emergency services or take the infant to the nearest hospital. While waiting for an ambulance, initial basic first aid can be administered as follows:
Back blows: If the infant is conscious, place them face down on your forearm or thigh with their head lower than their body. Using the heel of your hand, deliver 5 firm back blows between the infant's shoulder blades, directed downwards and forwards. If the infant does not cry, cough, or resume breathing, and their skin remains pale, chest thrusts are necessary. If the infant cries, coughs, and their skin turns pink, parents should not perform chest thrusts but should still take the infant to a medical facility for examination.
 |
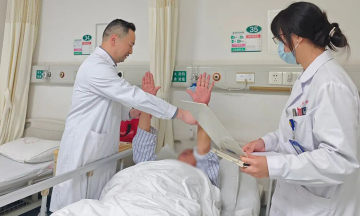
Dr. Le Thi Ngoc Dung (right) demonstrates how to handle infant milk choking during a prenatal counseling program. Photo: Tam Anh General Hospital |
Chest thrusts: Place the infant on their back (head lower than their body) on your forearm, resting on your thigh. Use two fingers (index and middle fingers) to press firmly on the center of the infant's chest (below the line connecting the nipples), performing 5 thrusts at a frequency of one second per thrust.
Parents should repeat back blows and chest thrusts if the infant has not resumed breathing or their face is not pink until they breathe normally, and then call emergency 115 or take the infant immediately to the nearest medical facility.
Infants experiencing severe milk choking often cannot cough or cry and may show bluish discoloration. If the infant loses consciousness or shows signs of respiratory arrest, parents should call for help from a relative and simultaneously call emergency 115.
To reduce the risk of milk choking, parents should feed the infant in the correct position, keeping their head higher than their body. Avoid feeding infants when they are crying or excessively hungry. If the mother has an abundant milk supply or a strong let-down, she can express a small amount of foremilk before feeding, hold the infant upright, and burp them after feeding to reduce the risk of reflux.
Dr. Le Thi Hong Hue
Pediatrics Unit
Tam Anh General Clinic District 7
| Readers can submit questions about infant care here for a doctor's response. |