This innovative model marks the first comprehensive treatment for Pierre Robin sequence in the South. Doctor Ngo Ngoc Quang Minh, Director of Children's Hospital 1, announced the model's launch on 20/3. He stressed the complex nature of the disease and its high risk of death from suffocation if not addressed promptly, underscoring the necessity of a multidisciplinary team for early, comprehensive care. Following over one year of collaboration with a team of US experts, doctors from the Maxillofacial Department have mastered two key techniques: bilateral mandibular distraction osteogenesis to widen the airway, and the use of an orthopedic appliance to advance the tongue and floor of the mouth, which reduces obstruction and supports jaw development.
Pierre Robin sequence is a rare congenital anomaly characterized by an underdeveloped mandible. This condition causes the tongue and floor of the mouth to be displaced posteriorly, leading to airway obstruction. Many affected children also present with a cleft palate. These abnormalities create difficulties in breathing, feeding, and swallowing, making infants susceptible to respiratory infections from birth. In severe instances, airway obstruction can become life-threatening.
Previously, treatment for this syndrome at Children's Hospital 1 was primarily temporary. Methods included changing sleeping positions, inserting breathing tubes, or performing a tracheostomy. However, a tracheostomy carries many risks, including infection and difficulties with long-term care.
 |
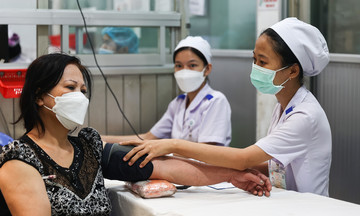
Experts from the US team and Children's Hospital 1 doctors examine a child with Pierre Robin sequence on 20/3. *Photo: Le Phuong* |
According to Professor Phuong D. Nguyen, Medical Director of Nuoy Reconstructive International and Head of Pediatric Plastic Surgery at the University of Colorado School of Medicine, the mandibular distraction osteogenesis method, adopted globally since the 1990s, offers superior efficacy. In Vietnam, since 2022, local doctors have successfully performed dozens of mandibular distraction cases independently. The success rate for patients avoiding tracheostomy is 100%, and their sleep apnea index has decreased from dangerous levels to completely normal.
In its first year of implementation at Children's Hospital 1, nearly 20 children with this syndrome have been successfully treated and can now breathe and feed normally. This comprehensive treatment requires coordination among multiple specialties, including: Neonatology, Resuscitation, Otorhinolaryngology, Maxillofacial Surgery, Anesthesia and Resuscitation, Nutrition, and Rehabilitation, to monitor patients from the emergency phase through long-term recovery.
Le Phuong