Associate Professor, Doctor Pham Thi Ngoc Thao, from the Department of Intensive Care at Cho Ray Hospital and Vice President of the Vietnam Association of Emergency and Poison Control, announced at a scientific conference last week that the "green ICU" model (green intensive care) is a necessary step in the healthcare sector's green transition. Currently, Vietnam lacks a truly "green" intensive care unit (ICU), which is the area for treating the most severe and critical patients in a hospital.
ICUs and anesthesia-resuscitation areas are among the highest consumers of energy and medical supplies within hospitals. To sustain life, resuscitation rooms must continuously operate extensive machinery systems, using significant amounts of electricity, oxygen, medical gases, and water. These areas also generate large quantities of waste, primarily from single-use supplies and difficult-to-dispose-of equipment like ventilators at the end of their lifespan.
Compared to countries like Japan or Singapore, where medical waste is tightly controlled through strict segregation, the volume of waste in central hospitals in Vietnam remains substantial. The Covid-19 pandemic clearly showed the pressure from single-use plastic supplies and high electricity and water consumption required for severe patient care. These efforts occur as the healthcare sector contributes approximately 4-5% of total global greenhouse gas emissions.
The environmental impact of healthcare activities creates a paradoxical loop: environmental pollution (climate change, heavy metals, El Nino) increases illness, which in turn adds a burden to the healthcare system. Recognizing this challenge, Cho Ray Hospital began its transition years ago, replacing lighting systems with LED lights and applying solar energy.
However, achieving a comprehensive green model still faces many obstacles for the healthcare sector. Specifically, procurement policies lack criteria prioritizing safe reusable medical supplies, making it difficult to choose environmentally friendly products. Upgrading infrastructure and equipment also requires significant costs, while healthcare workers' habit of using single-use items cannot change quickly.
"Initial investment costs may be high, but the long-term benefits are substantial," Doctor Thao said, emphasizing that this journey requires time and perseverance. The hospital has developed a three-phase roadmap for implementing the green ICU.
 |
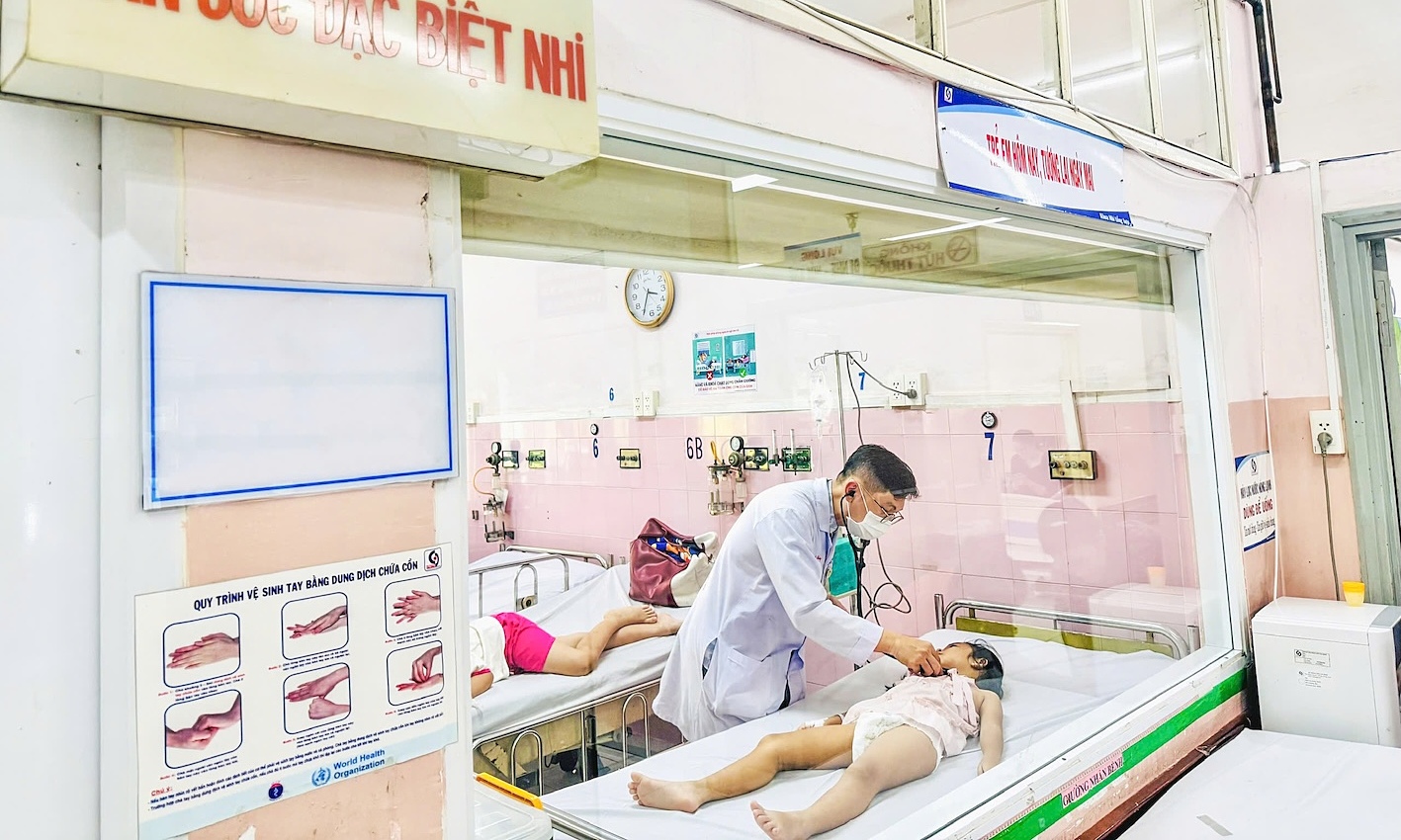
Emergency and Intensive Care Department, Cho Ray Hospital. *Photo: Hospital provided* |
Initially, the model will be piloted in two intensive care units, Zone B and Zone D. Solutions include: bedside waste segregation, supply chain review, designing spaces that utilize natural light, and training for energy-saving habits. The pilot's effectiveness will be measured not only by emission reduction levels or carbon offset costs but also by improvements in the working environment. With actual data, the model will be considered for expansion to other specialties such as respiratory, cardiology, and neurology.
"Medicine develops high-level techniques to save lives but also creates a significant environmental impact," the doctor emphasized. "A green ICU not only reduces this impact and optimizes resources but must also maintain the quality of patient care." According to experiences from developed countries such as Japan, South Korea, Singapore, and Canada, a "green ICU" operates on a 4P model:
* Product: focuses on sustainable medical equipment and supplies that can be safely recycled or reused.
* Process: aims for environmentally friendly procedures, reducing single-use items, source segregation of waste, and controlling anesthetic gases.
* People: emphasizes training healthcare staff, developing energy-saving habits, and multidisciplinary coordination.
* Patient: focuses on designing ICU spaces with natural light and good ventilation to aid comprehensive patient recovery.
Le Phuong