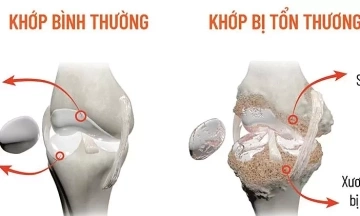
Mr. An, 85, was admitted to Tam Anh General Hospital, Ho Chi Minh City, in a critical state of near immobility and altered consciousness. A CT scan of his brain revealed acute bilateral subdural hematoma, causing severe compression of the brain tissue. Dr. Chu Tan Si, Head of the Department of Neurosurgery - Spine at the Neuroscience Center, explained that this condition typically arises when blood vessels tear, rupture, or bleed, most commonly following head trauma. While the hematoma lies outside the brain tissue, its growth can significantly increase intracranial pressure, compress the brain, and become life-threatening.
The patient, an elderly man, suffered from multiple severe underlying conditions: heart failure with an ejection fraction reduced to 30% (normal is over 50%), stage 4 chronic kidney failure, hypertension, and diabetes. A conventional open craniotomy would have posed significant risks, including hemodynamic instability, acute heart failure, respiratory failure, progressive kidney failure, and even death.
A multidisciplinary team of neurosurgeons, cardiologists, nephrologists, pulmonologists, and anesthesiologists convened to discuss Mr. An's case. They opted for bilateral subdural hematoma drainage via burr holes, a minimally invasive technique, instead of a wide craniotomy. This approach offered a shorter operating time, limited blood loss, and a reduced risk of complications, crucial given the patient's complex health profile.
The surgical team drilled small holes in the skull and inserted drainage tubes. This allowed the hematoma to drain slowly, carefully preventing sudden brain herniation. The timely intervention successfully relieved brain compression, significantly improved the patient's consciousness, and stabilized his neurological condition.
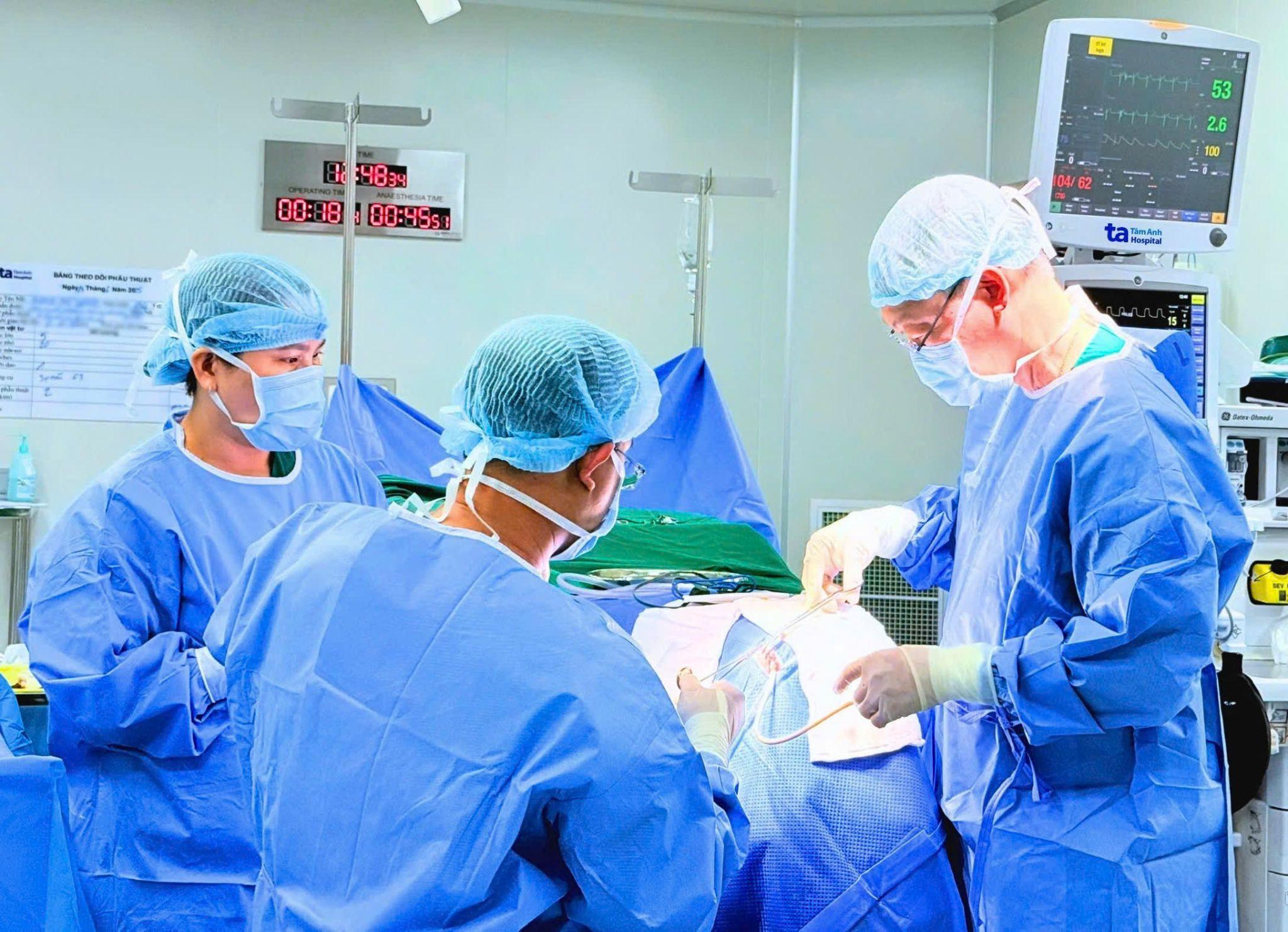 |
Doctors performing emergency surgery to drain a subdural hematoma, relieving brain compression for the patient. *Photo: Tam Anh General Hospital*
Following surgery, Mr. An was closely monitored in the intensive care unit (ICU) due to the high risk of complications, particularly acute heart failure, pneumonia, and progressive kidney failure. Dr. Huynh Thanh Kieu, Head of the Cardiology Department at the Heart Center, Tam Anh General Hospital, Ho Chi Minh City, prescribed medications to address his heart failure and pneumonia. Two days later, Mr. An developed critical acute kidney failure with elevated blood urea levels and required emergency dialysis. Once his kidney function recovered to its baseline, doctors initiated oxygen therapy, antibiotics, kidney support medications, and meticulously managed his blood pressure, blood sugar, and heart rate. After three weeks of comprehensive treatment, the patient's health stabilized, and he was discharged.
Intracranial hemorrhage can arise from various causes, most frequently head trauma resulting from traffic accidents, falls, or severe impacts. The risk is also significantly heightened in individuals taking anticoagulants or antiplatelet medications for underlying cardiovascular conditions, atrial fibrillation, or coronary stent implantation, as these drugs impair the body's natural clotting ability. Other contributing factors can include pre-existing bleeding disorders, liver disease, thrombocytopenia, or other hematological disorders.
Doctors advise individuals to take preventative measures such as wearing helmets when riding motorcycles, fastening seatbelts in cars, and avoiding excessive alcohol consumption to prevent falls. For elderly individuals, it is crucial to maintain adequate nutrition, implement strategies to prevent osteoporosis, and use assistive devices when moving to minimize the risk of injury.
Thu Ha - Trong Nghia
*Patient's name has been changed.
| Readers can submit questions about neurological diseases here for doctors to answer. |