Hanh had no unusual symptoms when he visited Tam Anh General Hospital Hanoi for a health check-up. Endoscopic examination revealed a flat, slightly concave 3 mm lesion in the lower one-third of his esophagus. A biopsy confirmed keratinizing squamous cell carcinoma.
Associate Professor Doctor Trieu Trieu Duong, director of surgery, stated that the patient had early-stage, localized esophageal cancer (cT1bN0M0) without lymph node metastasis. Although the tumor was small, it had invaded beneath the esophageal mucosa, posing a risk of metastasis. A complete esophagectomy and radical lymphadenectomy using a total endoscopic technique were necessary. This method minimizes invasiveness, reduces blood loss, and limits complications compared to traditional open surgery. Patients do not require intensive care unit (ICU) admission, which shortens overall hospital stay and recovery time, and results in smaller post-operative scars.
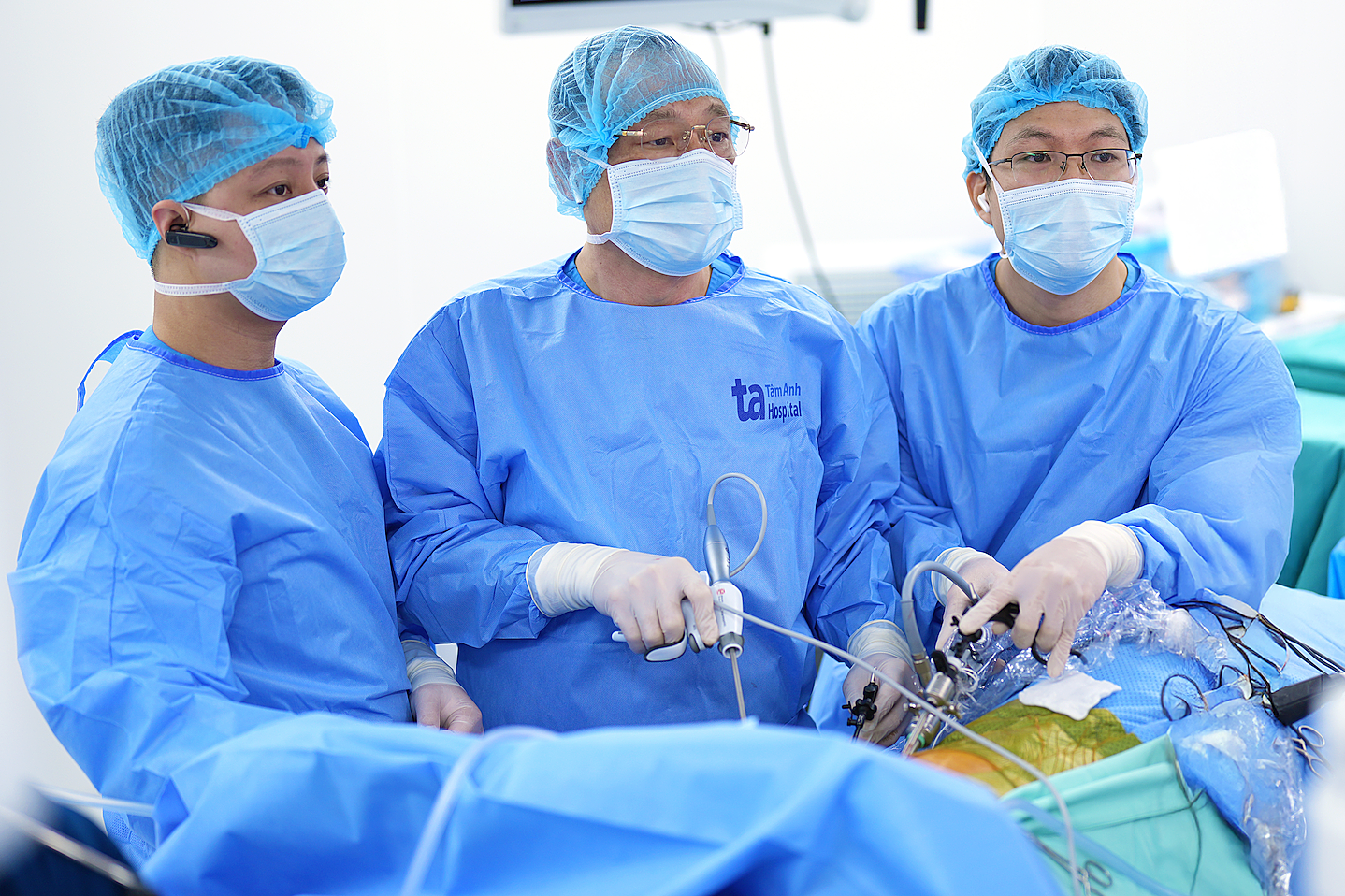 |
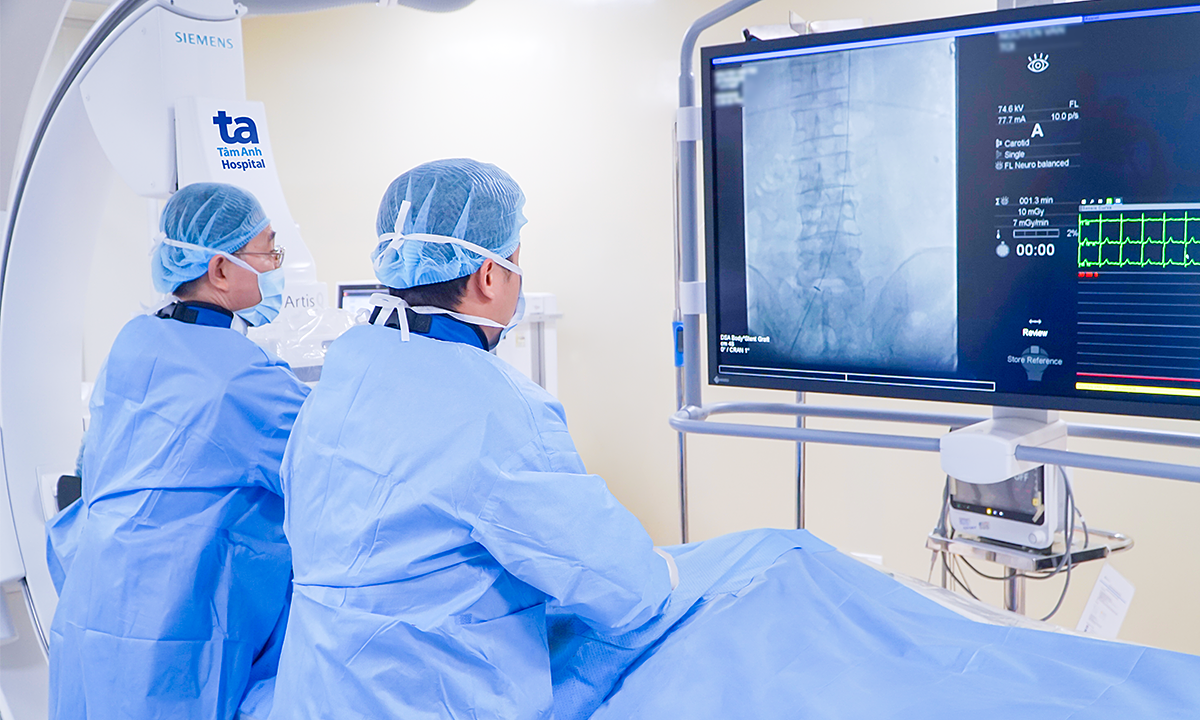
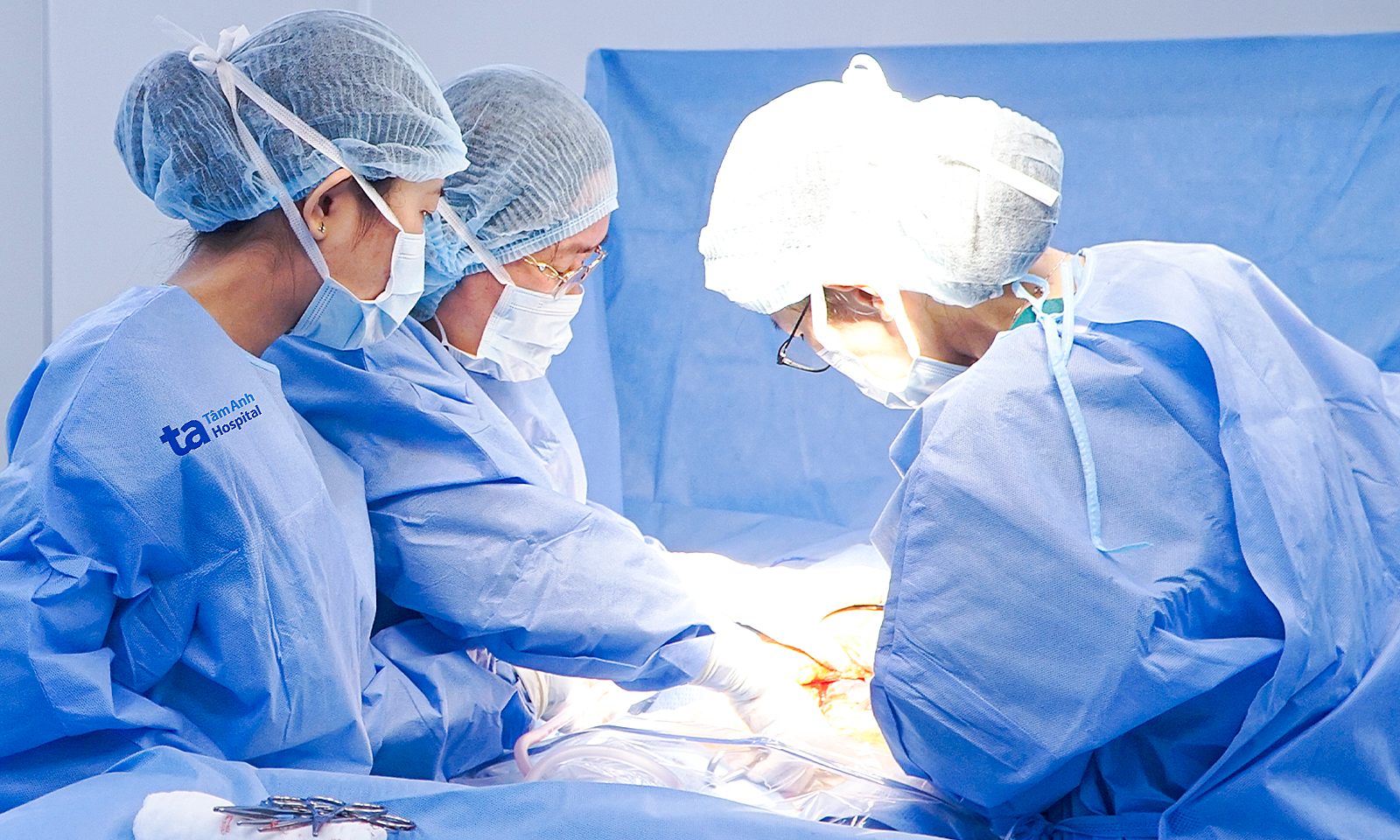
Associate Professor Duong and his team performed a total endoscopic esophagectomy for Hanh. *Photo: Tam Anh General Hospital*
The endoscopic team dissected the esophagus and stomach, then resected the esophagus. After the complete removal of the esophagus, it was necessary to replace it with another material to ensure continuous digestive tract flow. The doctors decided to reconstruct the stomach into an esophageal conduit within the abdominal cavity.
According to Associate Professor Duong, the stomach is the most commonly used material due to its rich blood supply from the gastroepiploic artery. It also provides sufficient length to be pulled from the abdomen to the neck, making it anatomically suitable. Reconstructing the stomach into an esophageal conduit is relatively straightforward, does not require microsurgery, and only needs one anastomosis in the neck, reducing the risk of leakage. Compared to the small and large intestines, the stomach's physiological characteristics are more similar to the esophagus, allowing food to pass naturally without stagnation.
One day post-surgery, Hanh experienced no pain, could walk and perform personal hygiene independently, and was fitted with a feeding tube. Once the gastroesophageal anastomosis had healed, he began oral feeding with liquid foods, consumed in small, frequent meals, gradually increasing consistency.
The patient tolerated the procedure well, had no reflux, and no digestive tract leakage, leading to discharge on the 10th day.
Post-surgery, the resected esophageal margins and all lymph nodes showed no cancer cells. Hanh did not require adjuvant chemotherapy or radiation therapy but will maintain regular follow-up appointments.
 |
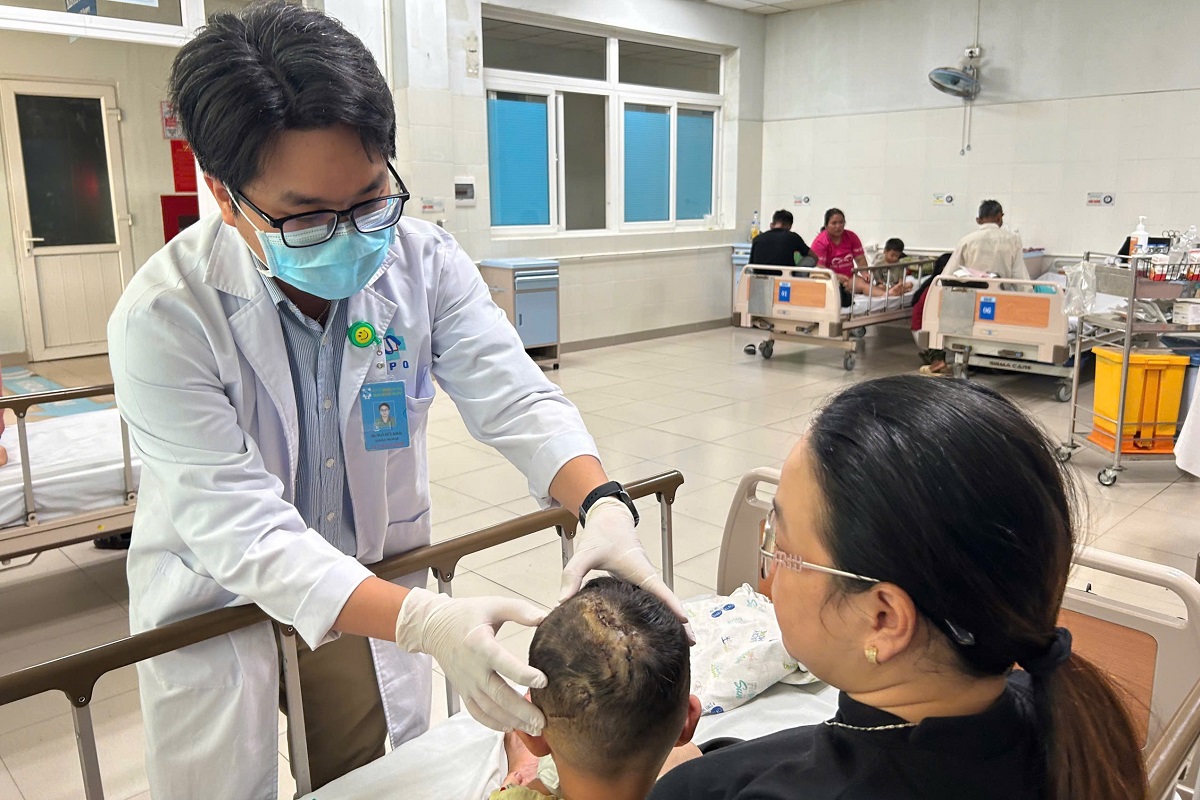
Associate Professor Duong visits Hanh after surgery. *Photo: Tam Anh General Hospital*
"Thanks to early cancer detection, Hanh's prognosis is very good, with a high survival rate exceeding 10 years", the associate professor stated.
Esophageal cancer is often detected at a late stage, when the tumor has invaded and metastasized. Patients then require costly multi-modal treatment involving chemotherapy, radiation therapy, surgery, immunotherapy, and targeted therapy, enduring severe side effects with a reserved prognosis.
Associate Professor Duong recommends that individuals over 45 undergo regular health check-ups at a hospital and esophageal cancer screening as advised by a doctor, especially if they have risk factors such as a family history, gastroesophageal reflux disease, ulcers, Barrett's esophagus, heavy alcohol consumption, or smoking.
Thanh Long
| Readers can submit questions about cancer here for doctors to answer. |