On 27/2, Dr. Phan Van Thai, Head of the General Surgery Department at FV Hospital, reported that a Cambodian patient was admitted in critical condition, vomiting blood, and in shock due to anemia and fluid deficiency. The patient was severely emaciated and had a distended abdomen. CT scans revealed extreme dilation of the stomach and duodenum, occupying almost the entire abdominal cavity. After intensive resuscitation and the insertion of a tube to drain over 5 liters of accumulated fluid, the patient's hemodynamic status stabilized. A month prior, the patient had undergone surgery elsewhere for persistent nausea, but without improvement.
A multidisciplinary team convened for a consultation. According to Dr. Thai, the bleeding from diffuse gastroduodenal inflammation was controlled with medication. However, the most challenging issue was the massive dilation of the stomach and duodenum. Initially, doctors suspected bowel obstruction due to previous surgery, but endoscopy and CT scans ruled out this possibility.
According to the doctor, the duodenum (the first part of the small intestine connected to the stomach) normally measures about 25 cm in length and, when collapsed, is only about the size of a finger. However, this patient's duodenum had a diameter of up to 12 cm and a circumference of 38 cm. After three days of drainage, the stomach had significantly decompressed, but the duodenum remained maximally dilated, adhered to surrounding organs, and had lost its contractile function, indicating no bowel obstruction. The team ruled out common causes and arrived at the final diagnosis of idiopathic megaduodenum, a condition with only about 15 recorded cases in world medical literature.
The condition caused food to stagnate and not pass into the small intestine, leading to persistent vomiting and prolonged emaciation. The optimal solution was to resect the entire diseased duodenal segment and reconstruct the digestive tract's flow. This is a complex surgery because the duodenum wraps around the head of the pancreas, a region with many converging blood vessels and bile-pancreatic ducts, posing a high risk of pancreatic fluid leakage.
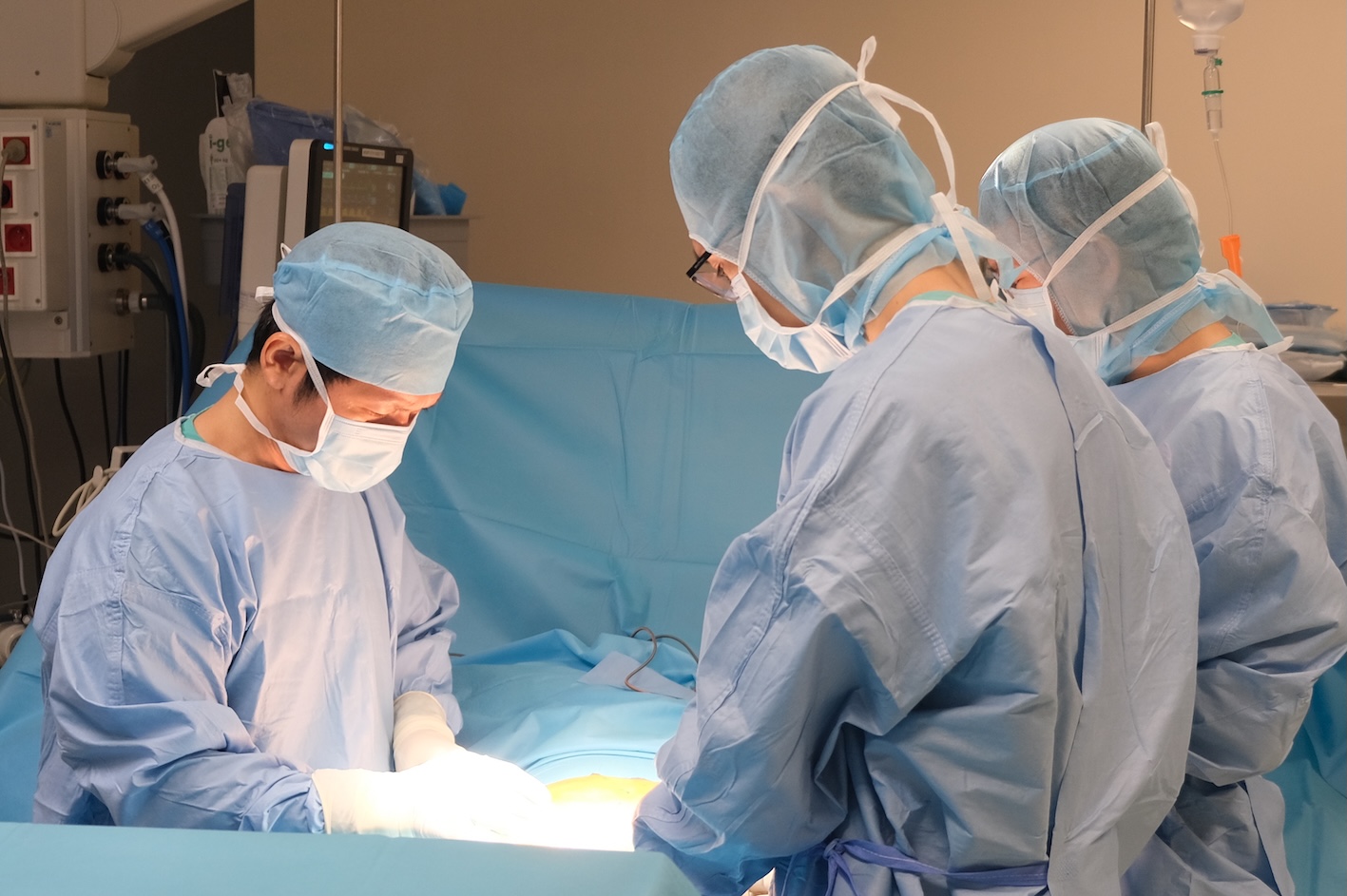 |
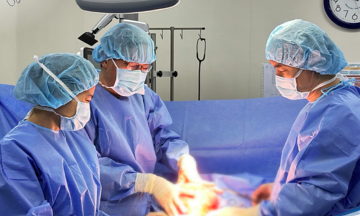
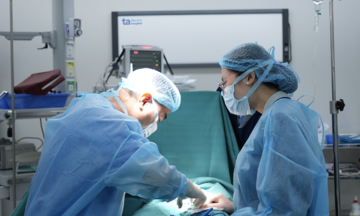
Dr. Phan Van Thai (left) and the surgical team operating on the patient with duodenal dilation. *Photo: Provided by the hospital.*
During the surgery, the team dissected and removed the malformed duodenal section, using two healthy segments of the small intestine for reconstruction. One segment was connected to the stomach to channel food, while the other naturally conveyed bile and pancreatic fluid, creating a new 'digestive junction'. After the operation, the patient stopped vomiting. Imaging confirmed good digestive flow with no fluid retention, and the patient was discharged after three weeks.
"After seven years, I can finally eat without vomiting," the patient said emotionally.
Experts state the condition is easily confused with superior mesenteric artery compression syndrome or common bowel obstruction. Many cases worldwide take years to be correctly diagnosed, requiring multidisciplinary collaboration for successful treatment.
Le Phuong