Osteoporosis, a condition marked by reduced bone density and quality, makes bones fragile and susceptible to fractures. It often progresses silently with few noticeable symptoms.
According to Doctor Nguyen Van Cong, a first-degree specialist from the Obstetrics and Gynecology Center, Tam Anh General Hospital Hanoi, women over 50 face a higher risk of osteoporosis compared to men due to their naturally smaller, thinner bone structures. Menopause significantly elevates this risk in women. Beyond age and hormonal changes, several other factors contribute to the increased likelihood of developing or worsening osteoporosis in women.
**1. Estrogen decline**
During menopause, estrogen levels drop rapidly, leading to increased bone resorption that outpaces bone formation. Estrogen typically balances osteoblast bone formation and osteoclast bone resorption. A sharp decrease in estrogen after menopause accelerates bone breakdown, and new bone growth cannot keep up. This reduces bone mineral density, making bones porous, brittle, and prone to fractures even from minor impacts or daily activities.
 |
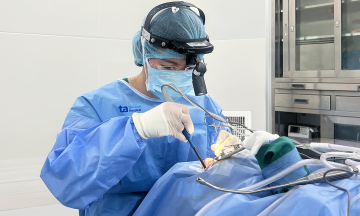
A doctor at Tam Anh Hospital Hanoi examines a woman. *Photo: Tam Anh General Hospital* |
**2. Chronic diseases**
Chronic conditions such as inflammatory bowel disease, rheumatoid arthritis, and systemic lupus erythematosus cause prolonged inflammation. This inflammation elevates pro-inflammatory cytokines, stimulating osteoclast activity and accelerating bone resorption. Patients with these conditions often require long-term glucocorticoid or immunosuppressant use, which diminishes osteoblast activity and impairs calcium absorption. This combination of chronic inflammation, medication effects, and post-menopausal estrogen decline hastens bone mineral density loss.
**3. Family history of osteoporosis**
Genetics play a role in peak bone mineral density, bone microstructure, and overall bone metabolism. Women whose parents, especially their mother, experienced osteoporosis or related fractures face an earlier risk of reduced bone mineral density.
**4. Smoking and alcohol consumption**
Nicotine and toxins in cigarette smoke hinder osteoblast activity, promote bone resorption, and lower estrogen levels. Prolonged alcohol consumption disrupts vitamin D metabolism, reducing intestinal calcium absorption and impeding bone formation. When combined with declining post-menopausal estrogen, these habits rapidly decrease bone mineral density and increase fracture risk.
**5. Calcium-deficient diet**
Calcium is a vital mineral for bone structure and strength. A long-term diet lacking sufficient calcium forces the body to draw calcium from bones into the bloodstream to maintain essential physiological functions, leading to reduced bone mineral density. In menopausal women, estrogen decline further reduces intestinal calcium absorption and increases bone resorption.
**6. Low body mass index (BMI)**
Individuals with a low BMI typically have less bone and muscle mass, which results in lower bone mineral density. In women with low body fat, estrogen levels show an even more pronounced decrease after menopause.
**7. Sedentary lifestyle**
Weight-bearing exercises stimulate bone formation and help maintain bone mineral density. When physical activity is low, mechanical stimulation to the skeletal system decreases, reducing osteoblast activity. For menopausal women, this inactivity, coupled with estrogen decline, accelerates bone loss.
Women should adopt a healthy lifestyle and proactively care for their bone and joint health. This includes a balanced diet rich in calcium, vitamin D, and other essential trace elements for bone formation, alongside regular physical activity. Limiting smoking and alcohol, maintaining a healthy weight, and taking prescribed medications are also important. Regular hospital check-ups for bone density screening are recommended.
Hang Tran
| Readers can send questions about obstetrics and gynecology here for doctors to answer. |