Meningococcal disease progresses rapidly, leaves severe sequelae, and has a high mortality rate, classifying it as a dangerous illness. Recently, health authorities reported an 11-year-old girl in Phu Quoc died from meningococcal disease. Authorities quickly cordoned off the area, isolated contacts, and disinfected the environment to prevent community transmission.
According to doctor Bach Thi Chinh, Medical Director of the VNVC Vaccination System, many people misunderstand this disease, leading to confusion and anxiety. Doctor Chinh addresses common questions to clarify understanding.
**Understanding meningococcal symptoms**
Initial symptoms are often non-specific, easily mistaken for the flu or a sore throat, including fever, headache, sore throat, and fatigue. However, meningococcal disease can be distinguished by subtle differences. For example, meningococcal fever is often sudden and unresponsive to antipyretics. Besides fever, patients may experience additional symptoms such as nausea, stiff neck, photophobia, and petechiae.
In infants, signs are difficult to recognize, such as lethargy, refusal to feed, irritability, or a bulging fontanelle. Petechiae, which are dark red or purplish-blue spots, do not fade when pressed. They can spread rapidly and merge into large patches, causing skin necrosis. These symptoms typically appear in severe stages of the disease, indicating a high risk of death.
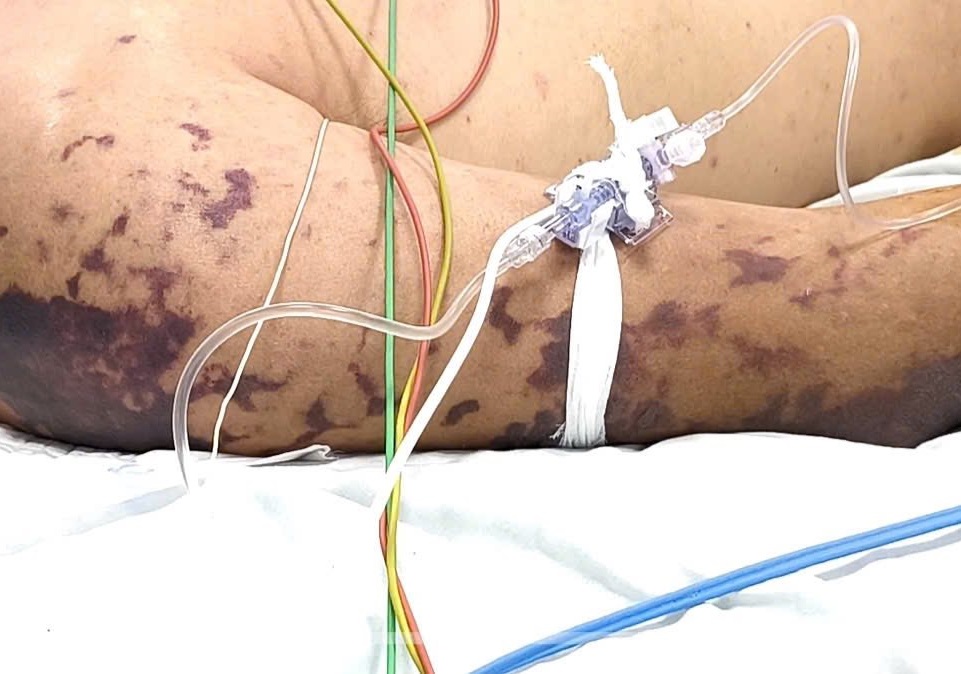 |
Petechiae appeared on the body of a meningococcal patient in january. *Photo: Central Hospital for Tropical Diseases*. |
**Transmission and disease progression**
Many people carry meningococci in their nose and throat without symptoms. This rate in the community can be 10-20% and higher in outbreak areas. The disease spreads through the respiratory tract when an infected person or an asymptomatic carrier coughs, sneezes, or talks at close range. Bacteria can also spread through contact with hands, objects, or contaminated surfaces, then enter the eyes, nose, or mouth, and subsequently invade the bloodstream. This is why the disease can spread silently, especially in schools, dormitories, and crowded places.
Meningococcal disease can cause meningitis, sepsis, or both simultaneously. The disease progresses rapidly and can become severe within just 24 hours. Without timely treatment, patients face a high risk of death or severe sequelae such as deafness, brain damage, seizures, memory impairment, necrosis, or limb amputation.
**Identifying and managing close contacts**
Individuals living in the same house, sharing a room, attending the same class, residing in the same dormitory, direct caregivers, or anyone with close contact to a patient are considered at-risk. Close contact is defined as occurring from 7 days before the patient's symptom onset until 24 hours after the patient has received appropriate antibiotics.
If you have had close contact with a patient, it is necessary to promptly report to local health authorities, comply with prophylactic medication, and monitor your health for 10 days from the last contact. If symptoms such as coughing or fever appear, seek medical attention and report them immediately; avoid contact with others to prevent disease spread.
**The importance of early vaccination**
Early meningococcal vaccination is recommended to prevent the disease, rather than waiting for an outbreak. Vaccines require time to stimulate the body to produce protective antibodies. During the incubation period or meningococcal infection immediately after vaccination, the body has not yet developed protective antibodies, leaving individuals still at risk of contracting the disease. Furthermore, large gatherings for vaccination during an outbreak can cause local overload, leading to long waiting times and inadequate service.
 |
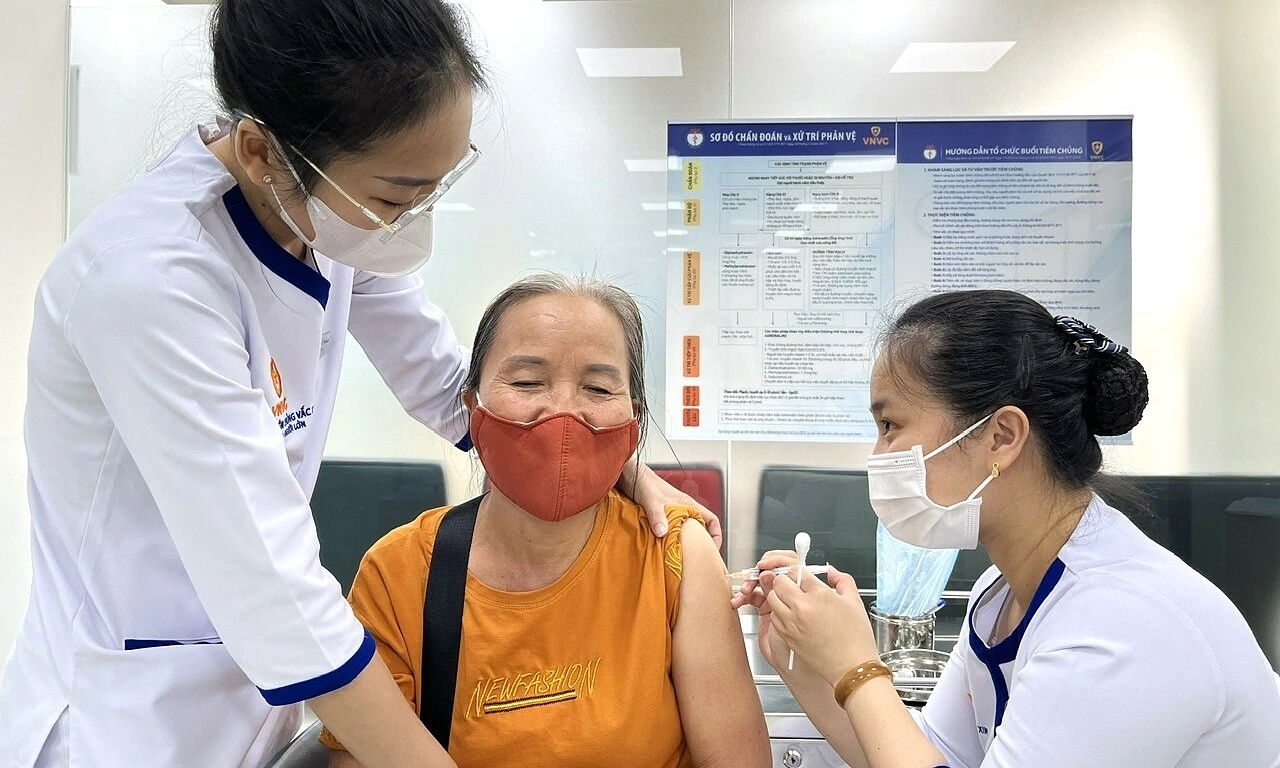
Residents from Phu Quoc Special Economic Zone brought children to VNVC Chau Thanh, An Giang, for meningococcal vaccination on the morning of 20/3. *Photo: Moc Thao*. |
Vietnam has licensed vaccines that fully protect against 5 serogroups of meningococcal disease for children and adults. These include three new-generation quadrivalent vaccines that protect against serogroups A, C, Y, and W: Menquadfi (USA) and Nimenrix (Belgium), administered from 6 weeks of age with no upper age limit for adults; and Menactra (USA), administered from 9 months to 55 years of age. Additionally, the new-generation Bexsero vaccine (Italy) protects against serogroup B, administered from 2 months to 50 years of age. The VA-Mengoc-BC vaccine (Cuba) protects against serogroups B and C, administered from 6 months to 45 years of age.
Individuals who have received the Cuba-produced B and C serogroup vaccine can supplement it with the new-generation serogroup B vaccine for broader protection against bacterial strains within serogroup B that cause the disease. Vaccines do not create cross-immunity, so people need to combine two types of vaccines: one for serogroup B and one for serogroups A, C, Y, and W. If only one type of vaccine is administered, the body remains susceptible to the disease caused by the other meningococcal serogroups.
**Additional preventive measures**
Besides vaccination, people also need to combine other preventive measures: maintaining personal hygiene, frequently washing hands, covering the mouth when coughing or sneezing. Living and working spaces should be well-ventilated and regularly disinfected. Everyone should wear masks in public and crowded places; avoid smoking, prolonged stress; and not share personal items.
Khanh Hoa