For many years, vaccines were primarily seen as tools for preventing infectious diseases. However, a growing number of observational studies show that middle-aged and older adults who receive certain vaccines have a lower risk of dementia compared to those who do not. This connection gained more attention after studies on shingles vaccines. Shingles is caused by the Varicella-Zoster virus, which also causes chickenpox. The virus can lie dormant in the nervous system for many years after chickenpox, reactivating to cause shingles when immunity declines. Experts suggest vaccines protect the brain in two main ways: by preventing infections that increase nervous system inflammation and by activating the immune system to clear harmful substances from the brain.
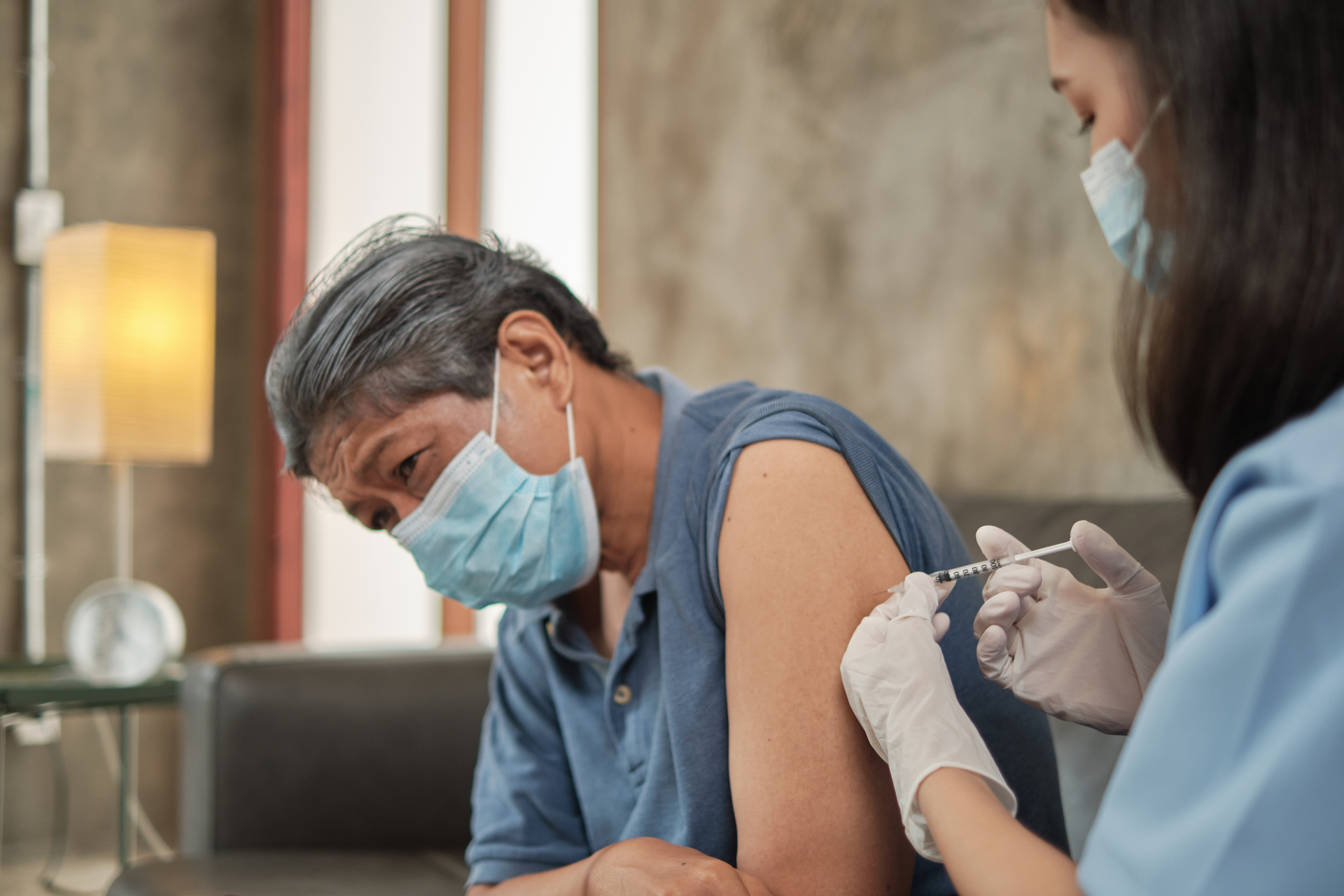 |
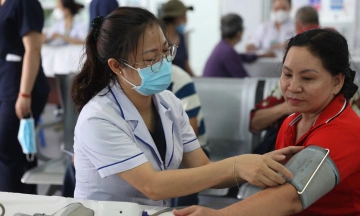
Regular vaccination supports brain health. Photo: Vecteezy |
How vaccines protect the brain
Pascal Geldsetzer, an epidemiologist at Stanford University, who studied shingles vaccines, stated that increasing evidence shows viruses can "hide" in the nervous system for years, linking them to neurodegenerative diseases. The simplest explanation is that vaccines help the body avoid infections that can harm the brain. When a person gets an infection, the body activates an inflammatory response to fight the pathogen. If this occurs repeatedly, persists, or involves viruses capable of residing in the nervous system, the brain can be affected. For example, the Varicella-Zoster virus constantly interacts with the immune system, causing neuroinflammation; a shingles vaccine can help reduce dementia risk. Beyond shingles, other infections have also been linked to dementia risk, including pneumonia, syphilis, Lyme disease, and periodontal disease. Some studies also suggest certain influenza virus strains might affect brain cells and relate to neurodegenerative conditions like Parkinson's disease or dementia. This prompts scientists to ask: if chronic infection and inflammation can contribute to brain decline, could vaccines preventing these diseases help mitigate the long-term risk of brain damage?
Another hypothesis is that vaccines can trigger a broader immune response in the body. Professor Rudolph Tanzi, a neurologist at Harvard Medical School, believes Alzheimer's disease often develops silently for many decades. From the appearance of the first amyloid plaques and protein tangles in the brain until clear dementia symptoms emerge can take about 20 years. Therefore, if some vaccines, only in use for a few years, have already shown a link to lower dementia risk, the protective mechanism might extend beyond preventing a specific infection. When vaccinated, the immune system not only learns to recognize a specific pathogen but is also awakened to a certain extent. According to Professor Tanzi, this peripheral immune response can help white blood cells enter the brain and clear amyloid plaques. These protein plaques are believed to play a significant role in Alzheimer's disease. In a study on mice genetically modified to mimic Alzheimer's, scientists observed that activating a peripheral immune response allowed white blood cells to migrate into the brain and begin processing plaques. Thus, Professor Tanzi suggests that vaccination might partially reduce the amyloid burden in the brain. Simply put, vaccines do not directly cure Alzheimer's but may prompt the immune system to work more actively in clearing substances related to neurodegeneration.
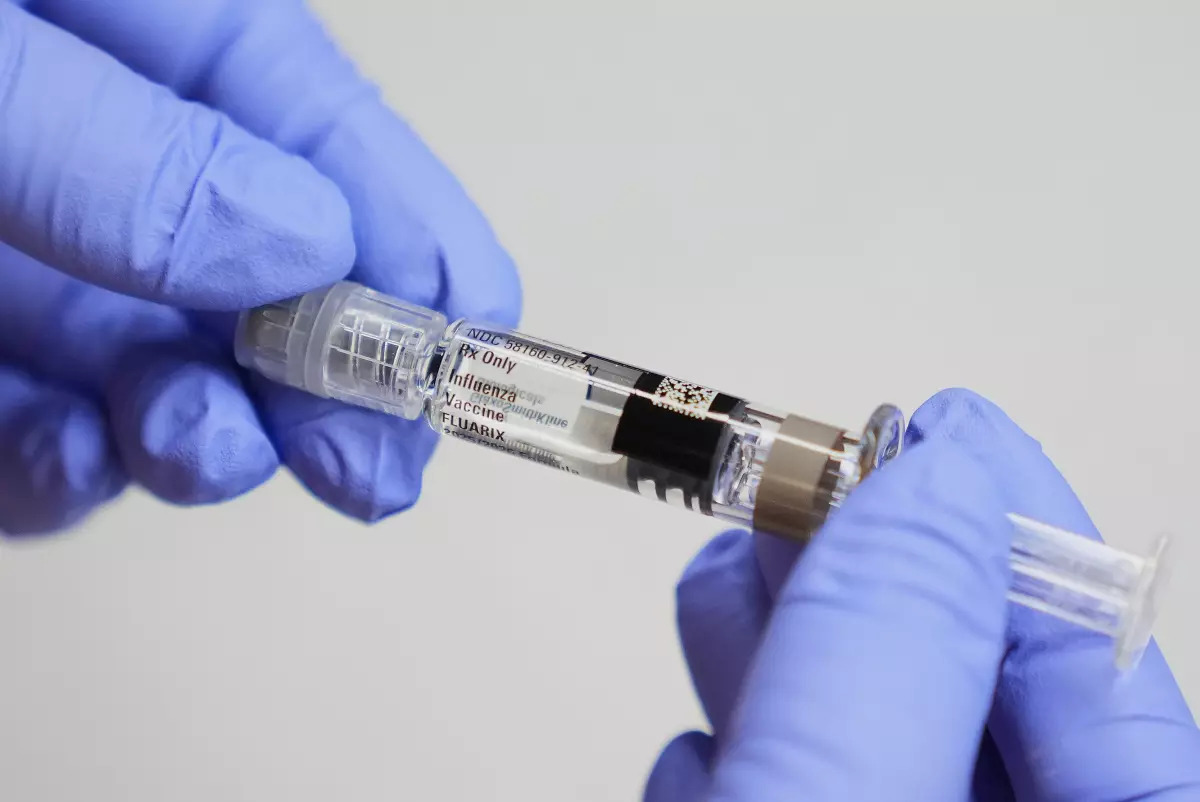 |
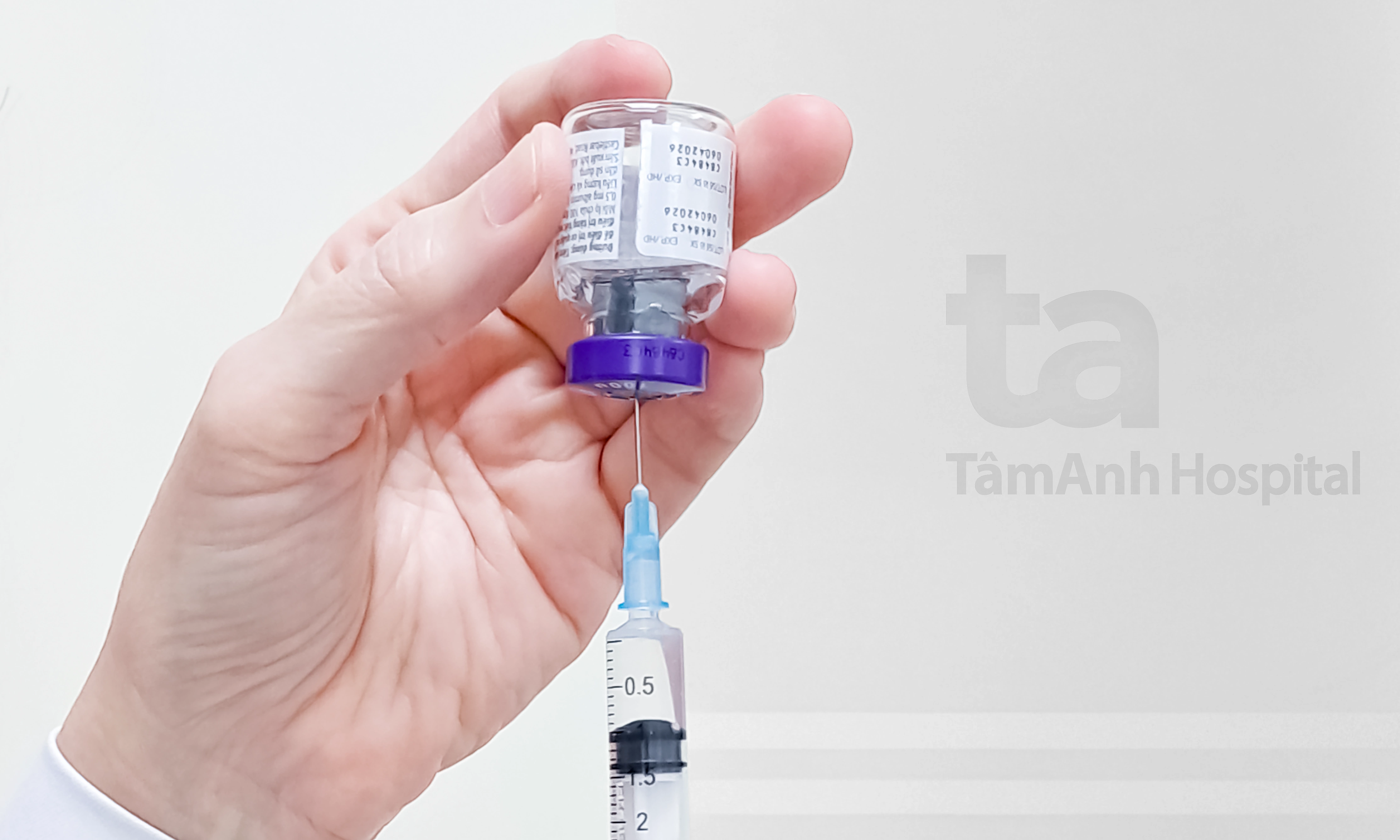
An influenza vaccine. Photo: AP |
Recommended vaccines
While the brain's protective mechanisms still require more research, experts agree that following recommended vaccination schedules offers clear benefits. Vaccines help reduce the risk of infections, minimize complications, decrease hospitalizations, and may provide additional benefits for brain health. For middle-aged and older adults, commonly mentioned vaccines include influenza, shingles, pneumococcal for pneumonia prevention, and RSV vaccine, depending on age, individual risk, and national recommendations. Professor Paresh Malhotra, a neurologist at Imperial College London, suggests that as evidence of vaccines' impact on brain health grows, it may be necessary to consider administering some vaccines earlier, from ages 40-50, rather than waiting until old age.
Van Ha (According to The Telegraph)