A baby boy, born at just 28 weeks gestation, faced a critical start to life. His mother, with a history of placental abruption, arrived at Tam Anh General Hospital TP HCM experiencing abdominal pain. Diagnosed with ruptured membranes, she received medication to mature the baby’s lungs before an emergency C-section. Born weighing 1,3 kg, the infant was not breathing, did not cry, was cyanotic, and had a heart rate below 100 beats/minute. Specialist Doctor Level II Pham Le My Hanh, Head of the Neonatology Department, Neonatal Center, explained that the baby's extreme prematurity meant underdeveloped organs, posing high risks of apnea, cardiac arrest, and potential brain damage.
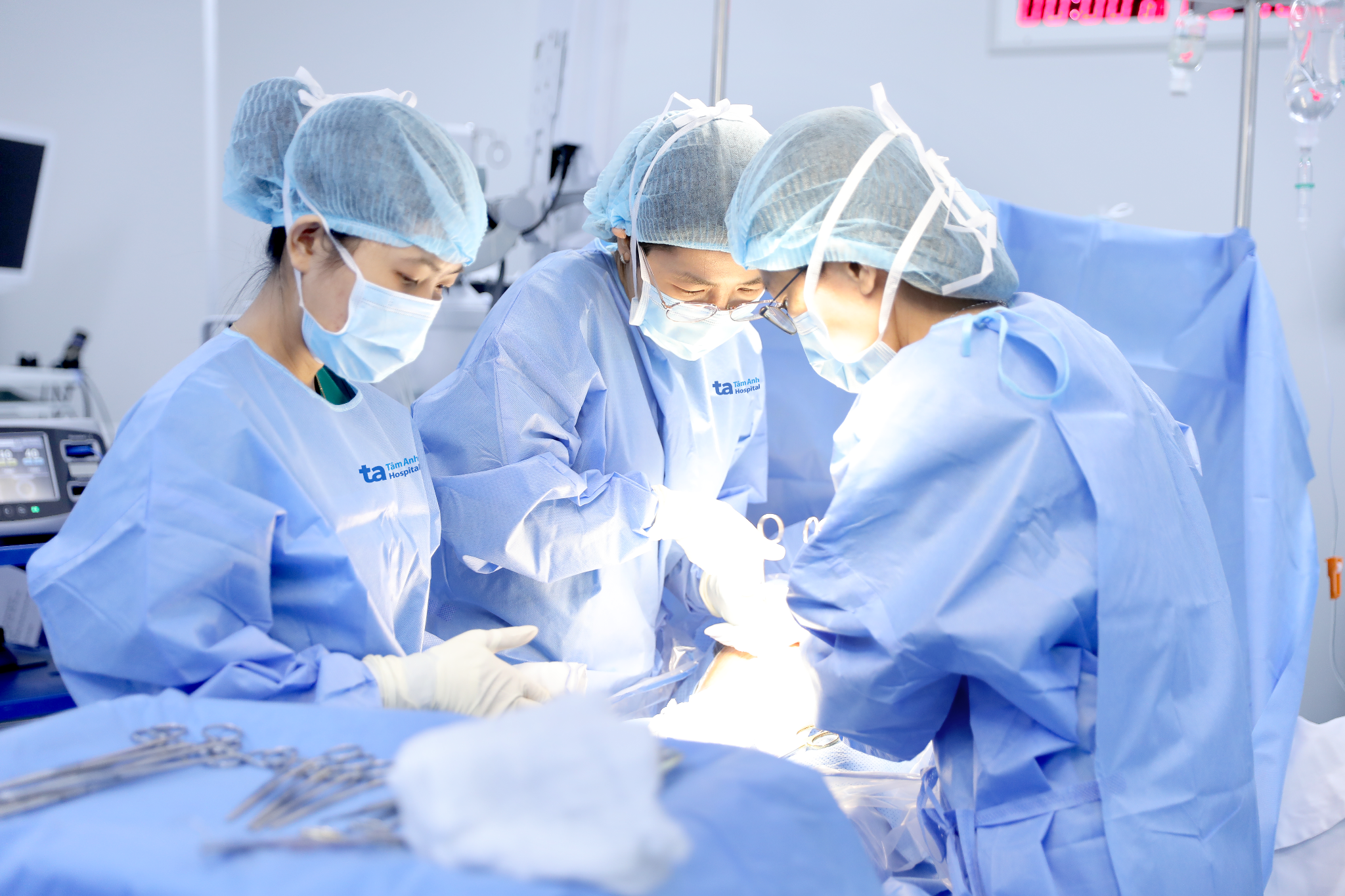 |
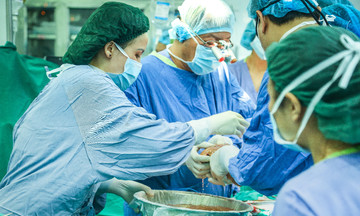
Obstetricians performing a C-section for the mother. *Photo: Tam Anh General Hospital*
Immediately, the obstetrics and neonatal teams initiated resuscitation in the delivery room. Due to unstable vital signs, the baby required intubation for respiratory support. Gradually, his heart rate improved, rising above 100 beats/minute, his skin regained color, and his limbs showed slight movement. Continuous monitoring of blood oxygen saturation (SpO2) and other vital signs was maintained. The baby was kept warm in a specialized thermal bag and then transferred to the Neonatal Intensive Care Unit (NICU) for ongoing care in an incubator.
Specialist Doctor Level I Nguyen Minh Thanh Giang, from the Neonatal Center, reported that the infant suffered from severe respiratory failure. Treatment included antibiotics, surfactant to enhance lung ventilation and oxygen exchange, and specialized mechanical ventilation. An effective "golden hour" intervention led to improved respiratory function within 24 hours of birth, allowing the baby to be extubated and moved to non-invasive mechanical ventilation. A day later, a blood transfusion was necessary due to severe pallor, providing essential energy for his brain, heart, and lungs to recover and stabilize blood pressure, thereby protecting the delicate cerebral blood vessels typical in extremely premature babies.
The medical team focused on nutrition, providing intravenous feeding alongside early breast milk delivered via a gastric tube. The baby responded well, gradually transitioning to continuous positive airway pressure (CPAP), a non-invasive respiratory support. However, 16 days after birth, the infant suddenly turned cyanotic, experiencing multiple episodes of apnea and a heart rate below 100 beats/minute. The NICU emergency team promptly intervened, stimulating his skin until his color returned. An X-ray confirmed pneumonia, necessitating a second 10-day course of antibiotics.
Although the pneumonia resolved, recurrent apnea persisted. An echocardiogram revealed a large patent ductus arteriosus (PDA), a fetal blood vessel that typically closes shortly after birth. When it remains open, it causes abnormal blood flow and can lead to pulmonary circulatory overload, increasing risks of heart failure and further complications. The medical team successfully closed the PDA with medication. A follow-up echocardiogram three days later confirmed the vessel had shrunk to 0,7 mm, with no adverse hemodynamic effects.
Throughout his recovery, the baby also received blue light therapy for jaundice and a second blood transfusion to support his development. Embracing a "family-centered care" approach, his mother visited daily to hold him. This close connection helped stabilize his heart and breathing rates, reduced stress, strengthened his immune system, and fostered overall development. After 67 days of intensive care, the baby was able to breathe and feed independently, his weight had increased to 3 kg, and he had received all necessary vaccinations. He was discharged home with a schedule for regular follow-up appointments.
 |
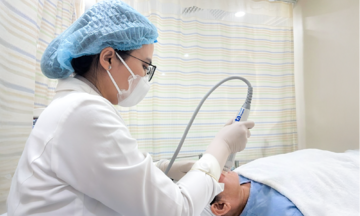
Doctor Giang checking the baby's health before discharge. *Photo: Tam Anh General Hospital*
Doctor Hanh emphasized the importance of close monitoring for premature infants during their first two years, focusing on both physical and mental development. She noted that their weight, height, and head circumference might initially be below standard averages. Developmental milestones, such as rolling, crawling, sitting, walking, and speaking, often occur later than in full-term infants. Parents are advised to consult with their doctor to track the baby's progress using an adjusted age, calculated from the original due date rather than the actual birth date.
Ngoc Chau
| Readers can submit questions about neonatology here for doctors to answer |