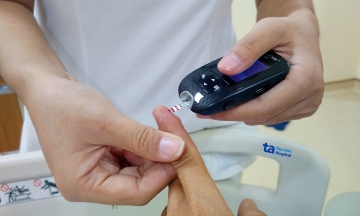
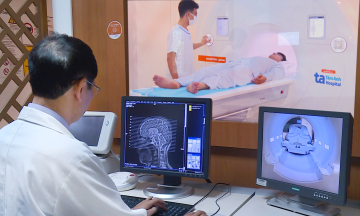
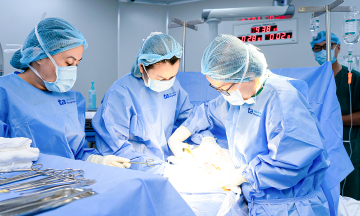
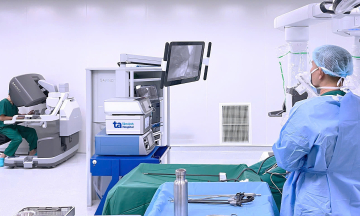
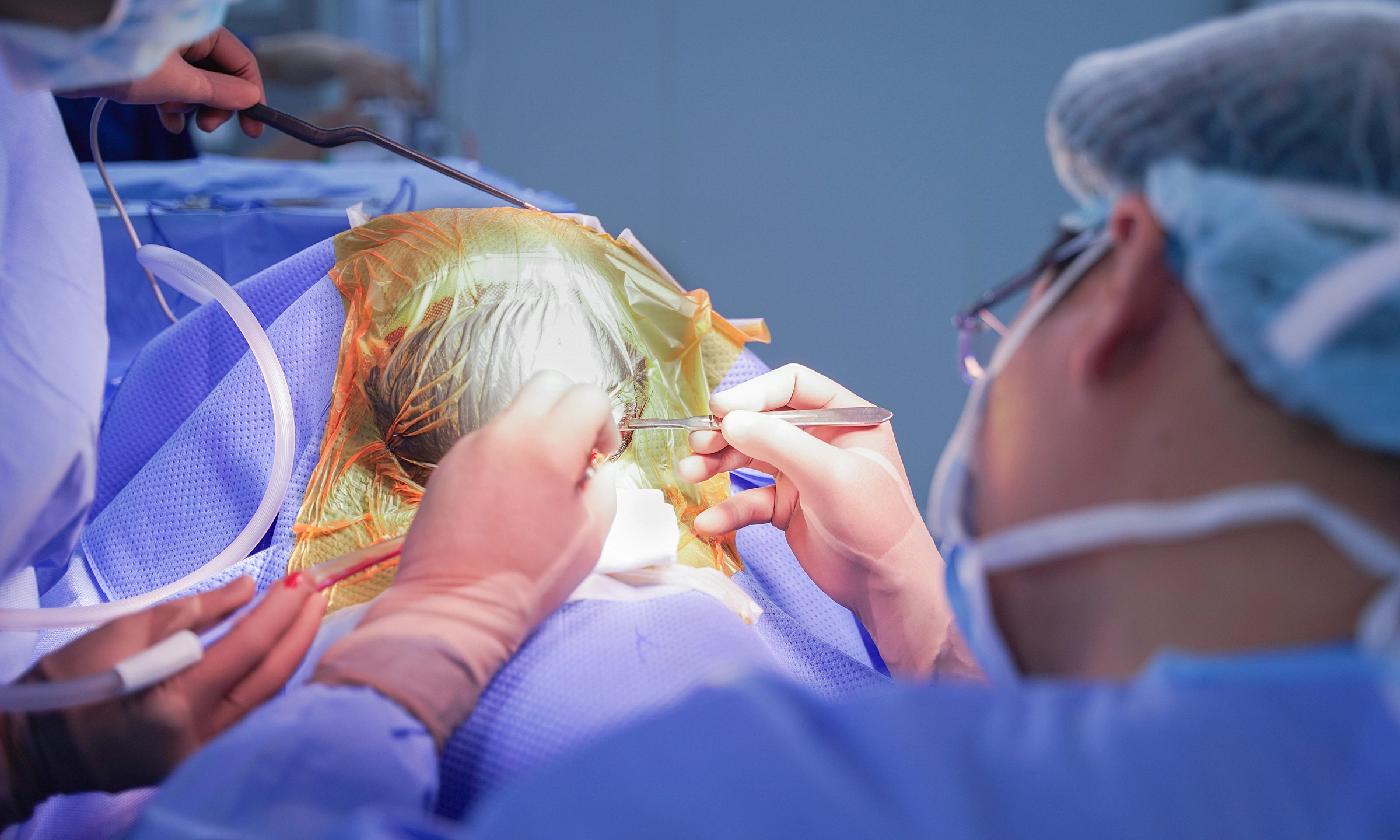
One week after stent placement, Mr. Tri experienced fatigue, fever, shortness of breath, a cough with phlegm, and chest tightness, leading to his transfer to Tam Anh General Hospital TP HCM. Doctor Do Anh Tuan, a specialist level one physician in the Department of Internal Cardiology at the Cardiovascular Center, reported that the patient had pneumonia, acute heart failure (ejection fraction (EF) dropped to 35%, normally above 50%), and pericarditis causing pericardial effusion. The doctor diagnosed him with Dressler's syndrome, also known as post-myocardial infarction syndrome, which causes secondary pericarditis after surgery or cardiac trauma.
Doctor Tuan explained that when heart muscle is damaged due to ischemia or surgery, heart cells die, releasing protein components (antigens) into the circulatory system. Normally, these components are inside the cells, so the immune system does not come into contact with them. When they spill out, the immune system mistakenly identifies them as foreign agents (similar to bacteria or viruses) invading the body. As a result, the body begins to produce antibodies to attack its own heart tissue and pericardium, causing a widespread inflammatory reaction in the pericardium and pleura, leading to symptoms such as fever, cough, and chest pain.
The patient had a moderate amount of pericardial effusion, with no signs of cardiac tamponade, so the fluid volume could be monitored. The doctor treated him with high-dose aspirin for two weeks, combined with medications for heart failure, antiplatelet drugs, and statins.
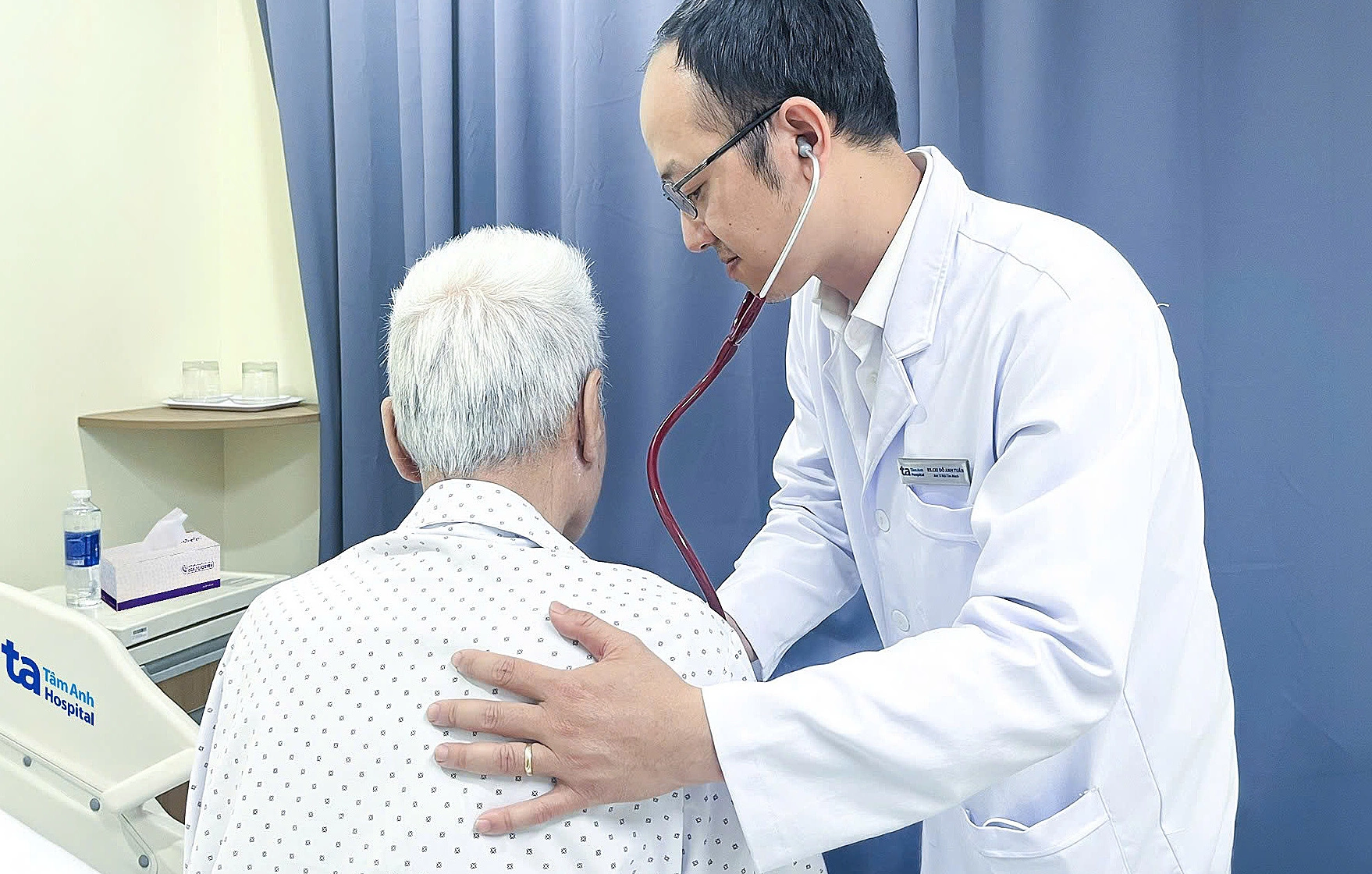 |
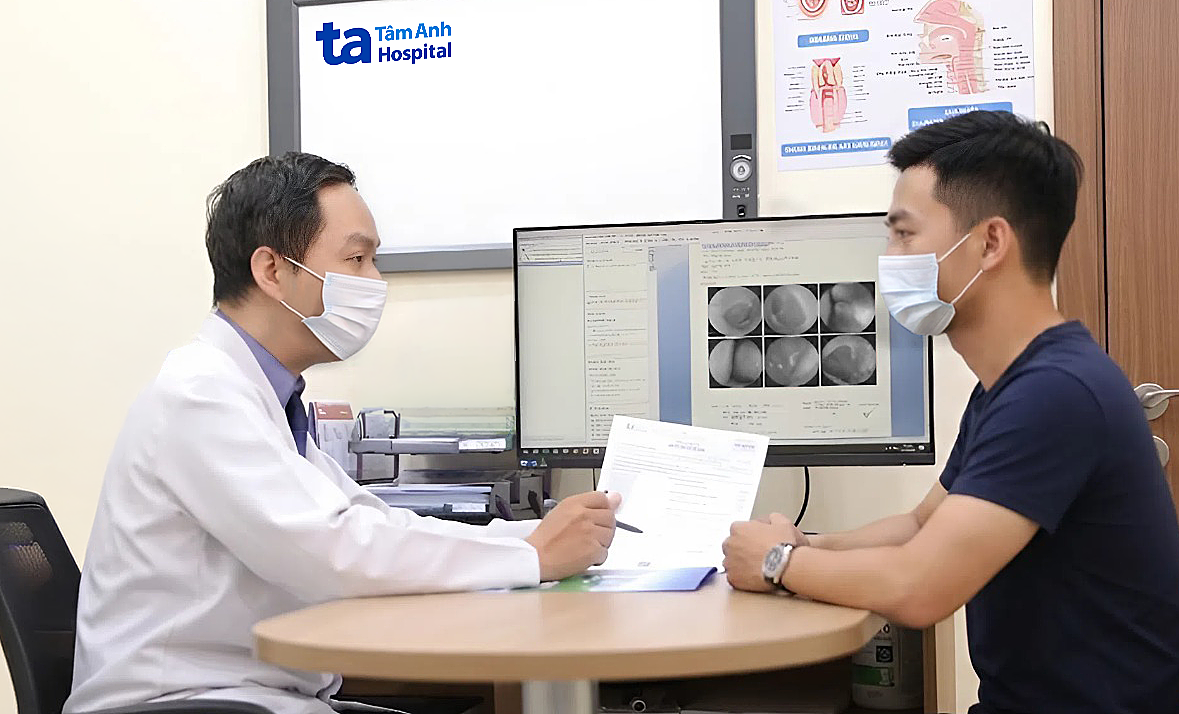
Doctor Tuan examines the patient before discharge. Photo: Ha Vu |
After 10 days, the fluid volume showed a decreasing trend; Mr. Tri's cough significantly reduced, his fever subsided, and he no longer had chest pain. He continued medication as prescribed for one more week; his heart function increased to 40%, pericardial fluid decreased, and his health stabilized, leading to his discharge.
Doctor Huynh Thanh Kieu, Head of Internal Cardiology Department 1 at the Cardiovascular Center, Tam Anh General Hospital TP HCM, stated that if detected early, Dressler's syndrome can be well-controlled with medication. However, if not treated promptly, prolonged inflammation can lead to many dangerous complications such as cardiogenic shock, and even death. This syndrome can also lead to constrictive pericarditis, though rare, which stiffens the heart, reduces its ability to pump blood, and causes heart failure, especially right-sided heart failure.
Doctor Kieu advised that patients who have undergone myocardial infarction intervention or heart surgery need close monitoring. Dressler's syndrome typically appears late, approximately two to four weeks after treatment for a cardiovascular event. Typical symptoms include pericardial chest pain, which worsens with deep breaths, coughing, swallowing, or lying down, and may lessen when sitting up or leaning forward.
In addition to chest pain, patients often experience shortness of breath (usually more pronounced when lying down), low-grade fever, general fatigue, rapid heartbeat, or decreased blood pressure. These are suggestive signs of pericarditis following cardiac injury.
Thu Ha
*Patient's name has been changed
| Readers can submit questions about cardiovascular disease here for doctors to answer. |