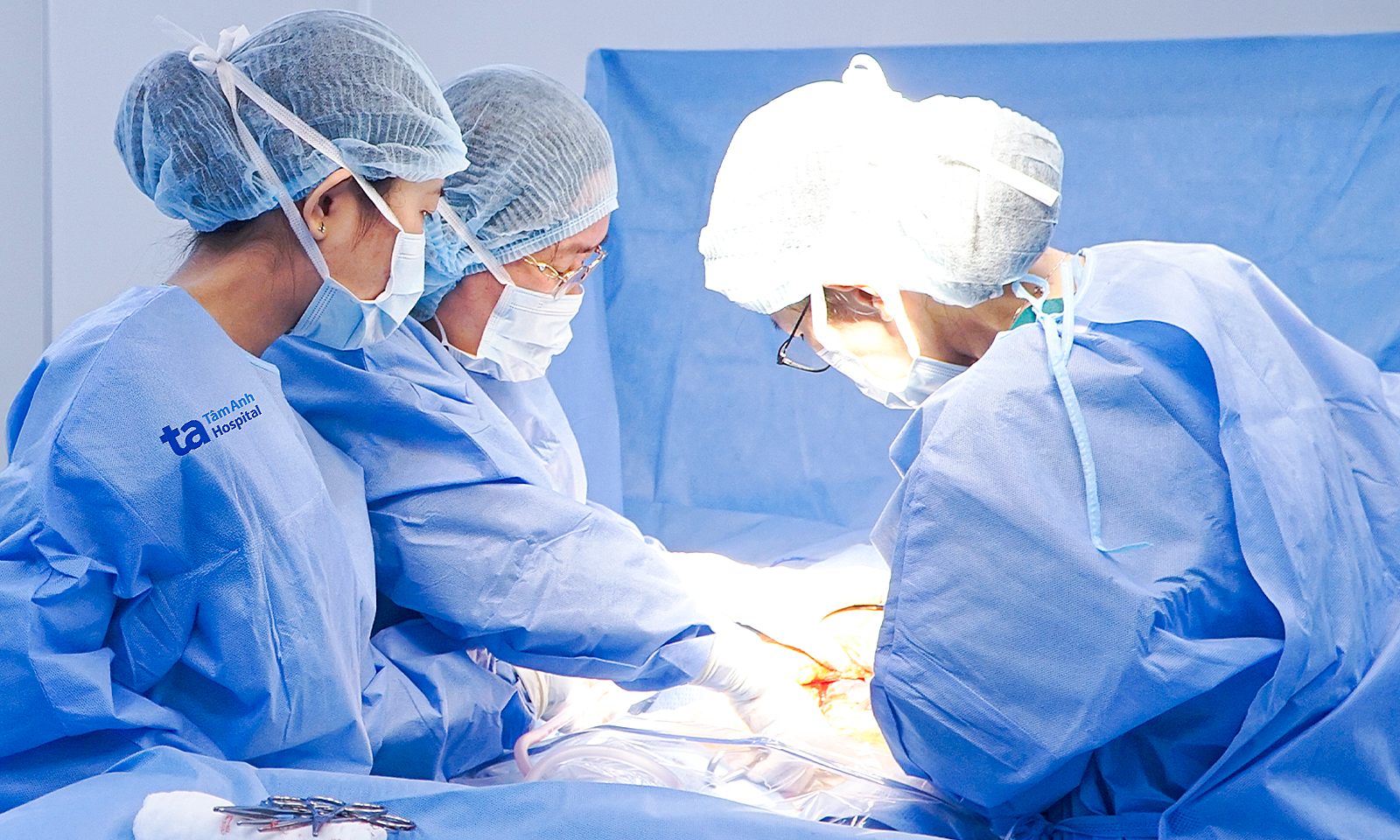
Born weighing 2.6 kg, the baby initially received intensive care for three days at another hospital before transfer to Tam Anh General Hospital Ho Chi Minh City. Dr. Cam Ngoc Phuong, Director of the Neonatal Center, highlighted the high-risk nature of the case, stressing the need for maximum safety during transfer. A dedicated team monitored the baby's respiration, circulation, body temperature, and vital signs throughout the journey until admission to the Neonatal Intensive Care Unit (NICU).
Dr. Phuong diagnosed the baby with chylothorax, grade three brain hemorrhage, and cholestatic jaundice. Chylothorax, a rare condition in newborns, happens when chyle—a milky white lymphatic fluid rich in triglycerides, fat-soluble vitamins, lymphocytes, and immunoglobulins—accumulates in the pleural space around the lungs. This condition has a high mortality rate due to nutrient loss, immune deficiency, and reduced perfusion to tissues and organs.
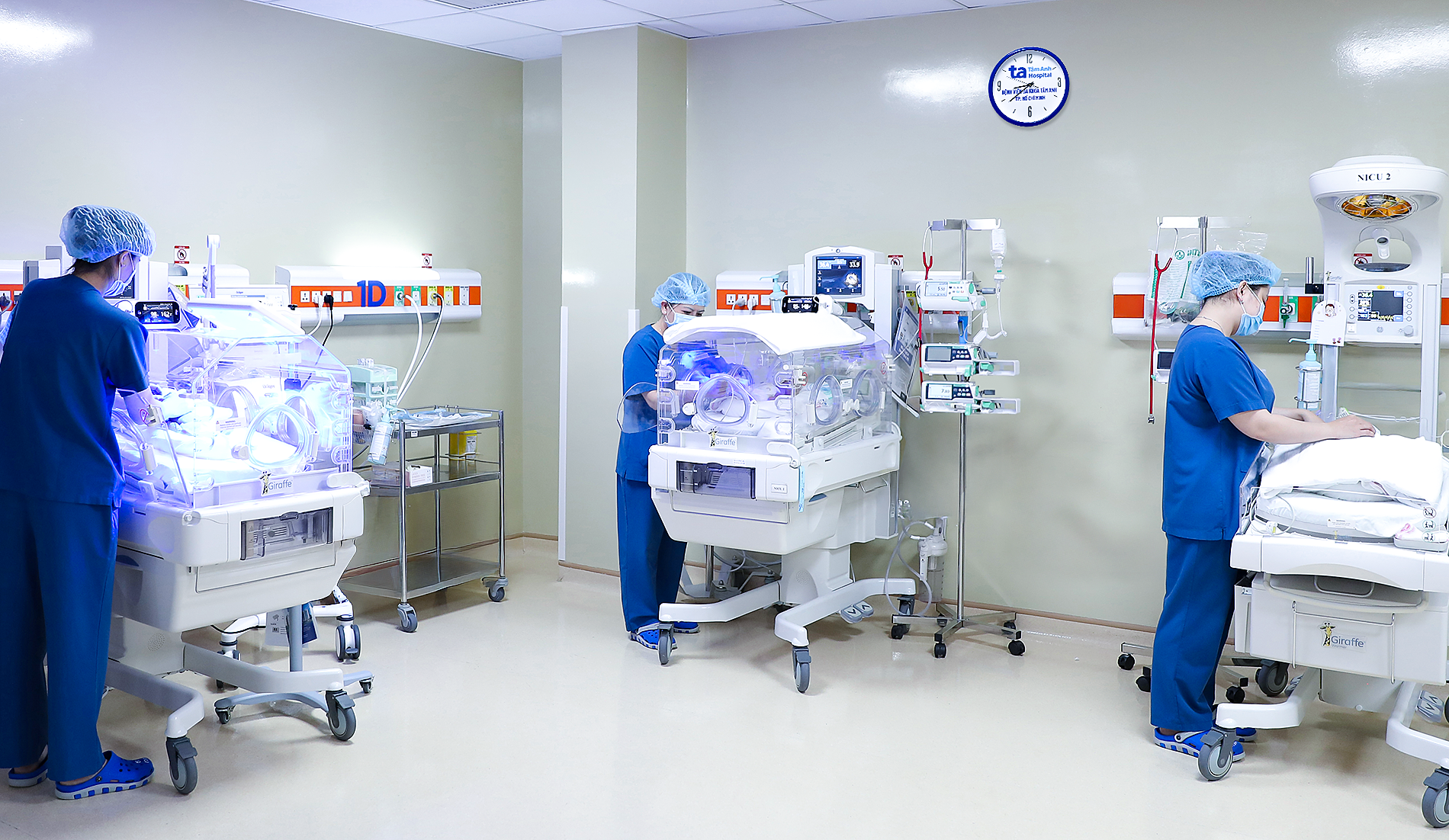 |
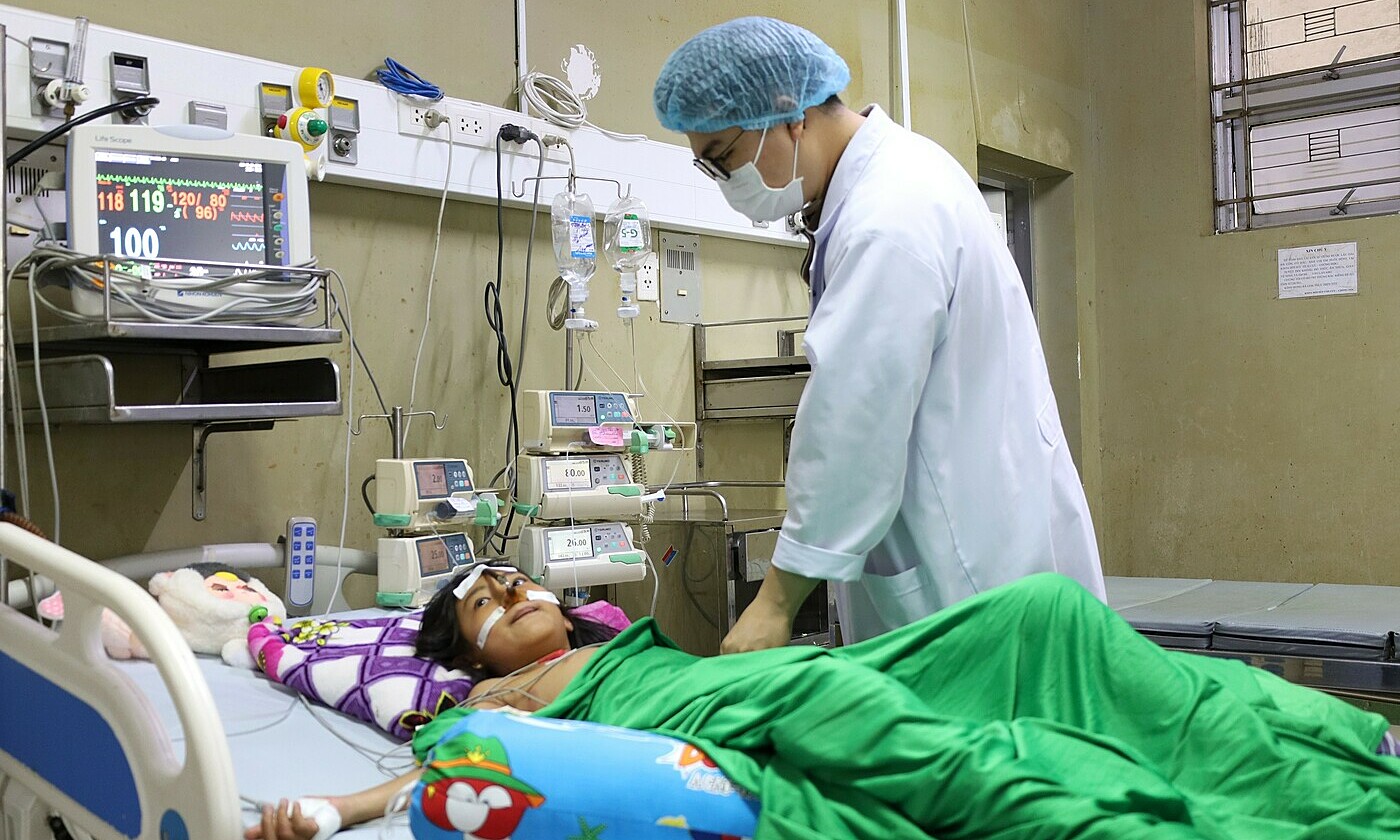
Nursing team caring for the premature baby at the Neonatal Intensive Care Unit. *Photo: Tam Anh General Hospital* |
The medical team supported the baby's respiration using a specialized ventilator for premature infants. They treated the pleural effusion with specific medications and provided intravenous nutrition along with antibiotics.
One day later, the baby's condition became unstable. Doctors performed pleural fluid aspiration and drainage. The infant responded to medication, and the drained pleural fluid decreased daily, allowing a switch to non-invasive ventilation. Concurrently, the baby received special milk via a gastric tube to reduce chyle production and provide energy through the digestive tract. After 8 days of treatment, the pleural drainage tube was removed, and the baby transitioned to oxygen therapy.
However, one week later, the infant developed bloody stools due to enteritis. Doctors stopped milk feeding to allow the digestive tract to rest, switching to intravenous fluids and administering combined antibiotics. 10 days later, the enteritis stabilized, and the baby resumed milk feeding.
Dr. Nguyen Thi Kim Hoc, from the Neonatal Center, noted the infant's grade three brain hemorrhage had an unclear cause. It was possibly due to vulnerable cerebral blood vessels in the germinal matrix, susceptible to various factors, leading to blood flow into the ventricles and subsequent ventricular dilation. This severe condition can cause mental and motor sequelae. The medical team strictly controlled blood pressure, oxygen and carbon dioxide levels, and clotting factors to prevent further bleeding.
The baby developed cholestatic jaundice due to Cytomegalovirus infection, which caused dark urine and pale stools. This condition can damage liver cells, potentially leading to liver failure, cirrhosis, and impaired fat absorption, resulting in malnutrition. Doctors prescribed antiviral drugs and bile thinners to dilute bile, protect liver cells, and stimulate bile secretion.
The baby's mother visited the hospital daily for skin-to-skin contact, supporting the baby's body temperature, heart rate, and breathing stability. After 8 weeks of treatment, the baby gained 3.7 kg, the pleural effusion resolved, and he breathed and fed well. The brain hemorrhage gradually diminished, and the jaundice improved.
Doctors recommended parents monitor the baby's motor and communication functions. They advised scheduled follow-up appointments for physical therapy intervention if indicated.
 |
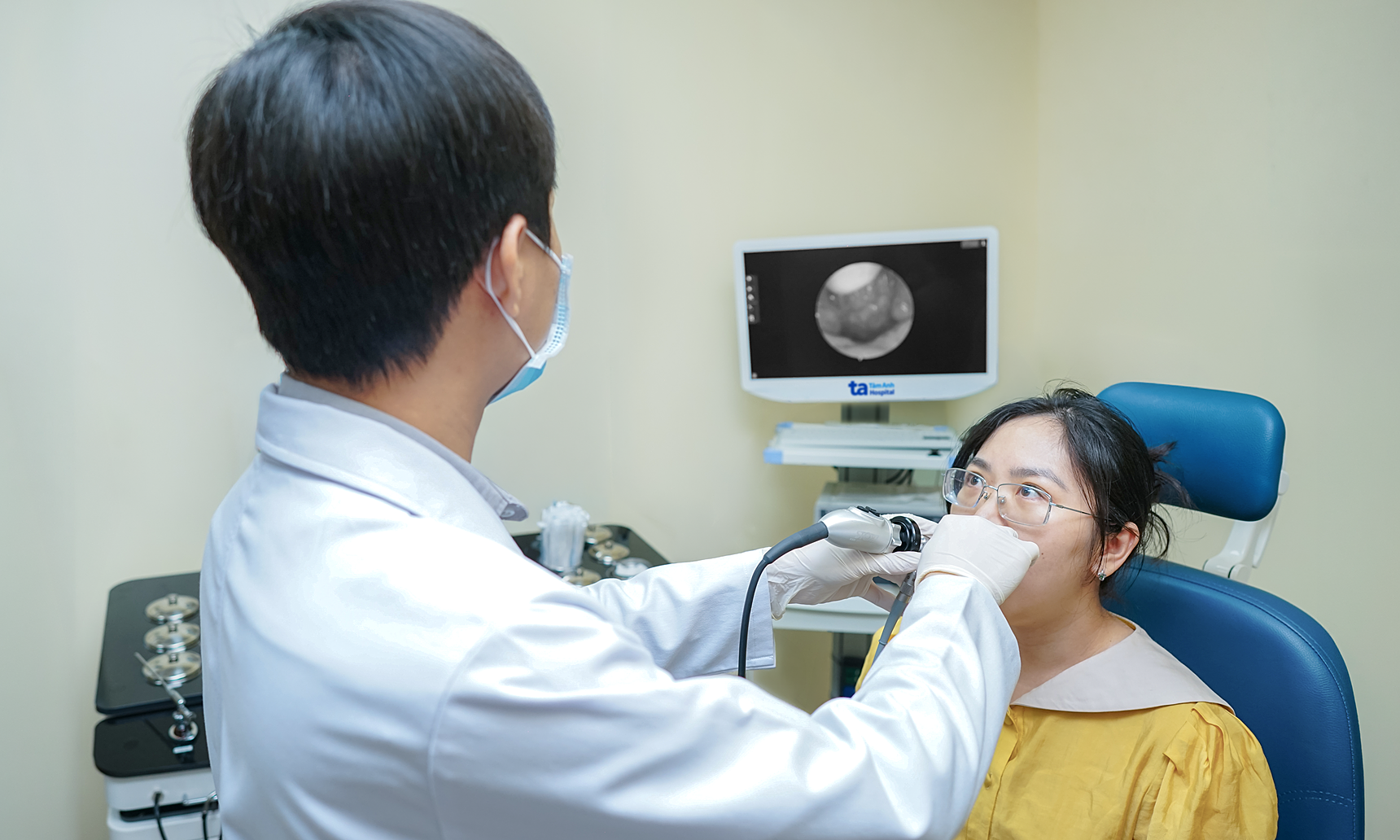
Doctors screened the baby for retinopathy of prematurity (ROP), noting no abnormalities. *Photo: Tam Anh General Hospital* |
Dr. Phuong explained that Tam Anh General Hospital employs a comprehensive resuscitation strategy for premature infants with complex multiple conditions. This approach helps them overcome critical stages and achieve stable development. Family involvement, through a family-centered care model, also supports effective treatment for these children.
Ngoc Chau
| Readers can send questions about neonatology here for doctors to answer. |