A wireless pacemaker is a device implanted inside the patient's body to treat conditions such as bradycardia-tachycardia syndrome, high-degree atrioventricular block, and atrial fibrillation with slow ventricular response.
Professor, Doctor Vo Thanh Nhan, Director of the Interventional Cardiology Center at Tam Anh General Hospital in Ho Chi Minh City, stated that traditional wired pacemakers, though widely used previously, were prone to complications like infection (due to the need for a skin incision to place the device under the skin), localized hematoma at the implantation site, and unsightly scars. Wireless pacemakers overcome these disadvantages. The device weighs approximately 2 g, which is 93% lighter than a conventional wired pacemaker (28 g). It is inserted directly into the right heart chamber via the femoral vein, making the procedure minimally invasive, painless, and scar-free. Patients remain conscious throughout the intervention and can walk around after one day.
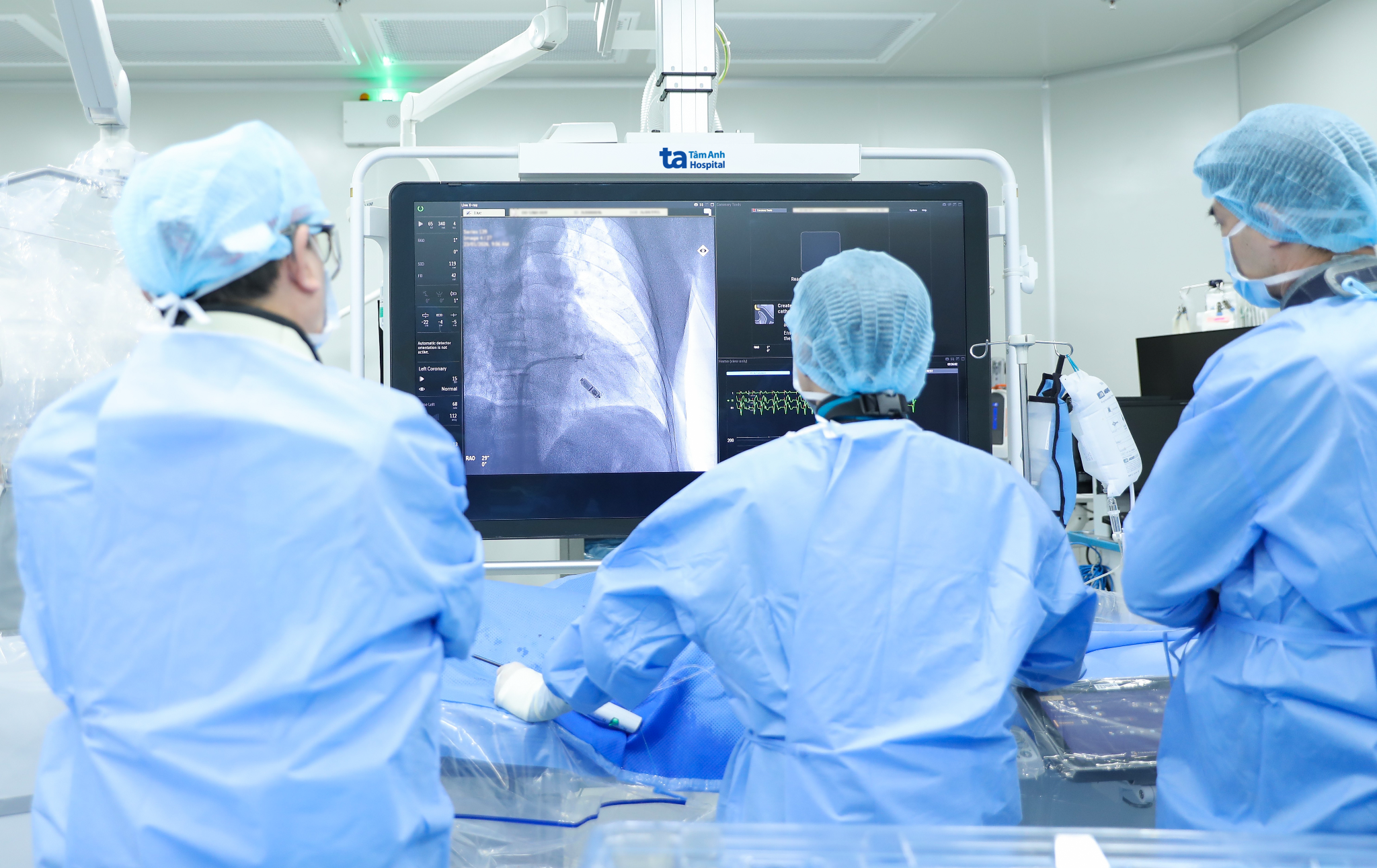 |
Professor Nhan and his team implanting a wireless pacemaker for a patient. Photo: Tam Anh General Hospital
While wireless pacemakers are suitable for many patients requiring a cardiac pacemaker, they are particularly beneficial for the following groups:
Individuals with a frail physique or multiple underlying health conditions: This group is not suitable for surgical procedures that require a skin incision to create a pocket under the skin or muscle for device placement. With a wireless pacemaker, doctors guide a catheter through the femoral vein to the right ventricle and position the device correctly. The implantation process takes about 30-45 minutes, compared to 90-120 minutes for wired pacemakers.
Those prone to keloid scarring: If a skin incision is necessary, patients would have a long, aesthetically unpleasing scar on their chest, which is prone to keloid formation if they have such a predisposition. Wireless pacemaker implantation avoids skin incision, thus preventing this risk.
Patients with a history of metal allergies: This device implantation technique does not require open-chest surgery, which helps patients avoid the risk of infection.
Thin individuals: For patients with a thin layer of subcutaneous tissue, dissecting muscle to place a device underneath can easily cause hematoma at the implantation site. Therefore, a wireless pacemaker is an optimal solution for thin individuals.
Patients with memory impairment: Elderly patients with memory impairment often forget they have a pacemaker and tend to touch or scratch the incision site, which can lead to infection. When a small, capsule-like pacemaker is placed inside the heart chamber, patients feel almost no foreign object in their body, allowing them to carry out daily activities comfortably.
Professor Nhan noted that after a wired pacemaker implantation, patients must avoid strenuous arm movements on the side of the device for at least several weeks. With a wireless pacemaker, patients can resume normal activities and perform personal tasks immediately after the intervention. It is important to attend follow-up appointments and take medication as prescribed by the doctor. If unusual symptoms occur, such as palpitations, shortness of breath, difficulty breathing, chest pain, weakness, or dizziness, patients should seek immediate medical attention.
Thu Ha
| Readers can submit cardiovascular questions here for doctors to answer. |