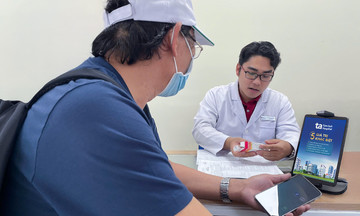
Master of Science, Doctor, Level II Specialist Huynh Thanh Kieu, head of Cardiology 1, Heart Center, Tam Anh General Hospital Ho Chi Minh City, reported that Mr. Tu was admitted conscious, without headache, dizziness, or chest pain. Elevated blood pressure increases arterial pressure, risking cerebral hemorrhage. This damages arterial walls, forming blood clots that can lead to ischemic stroke.
Hypertension is diagnosed when blood pressure readings are 140/90 mmHg or higher. Systolic blood pressure near 200 mmHg can manifest as headaches, blurred vision, dizziness, sudden weakness, facial paralysis or distortion, chest pain causing shortness of breath or coughing up blood, and decreased vision. Mr. Tu showed no symptoms, his condition was discovered during a dental check-up.
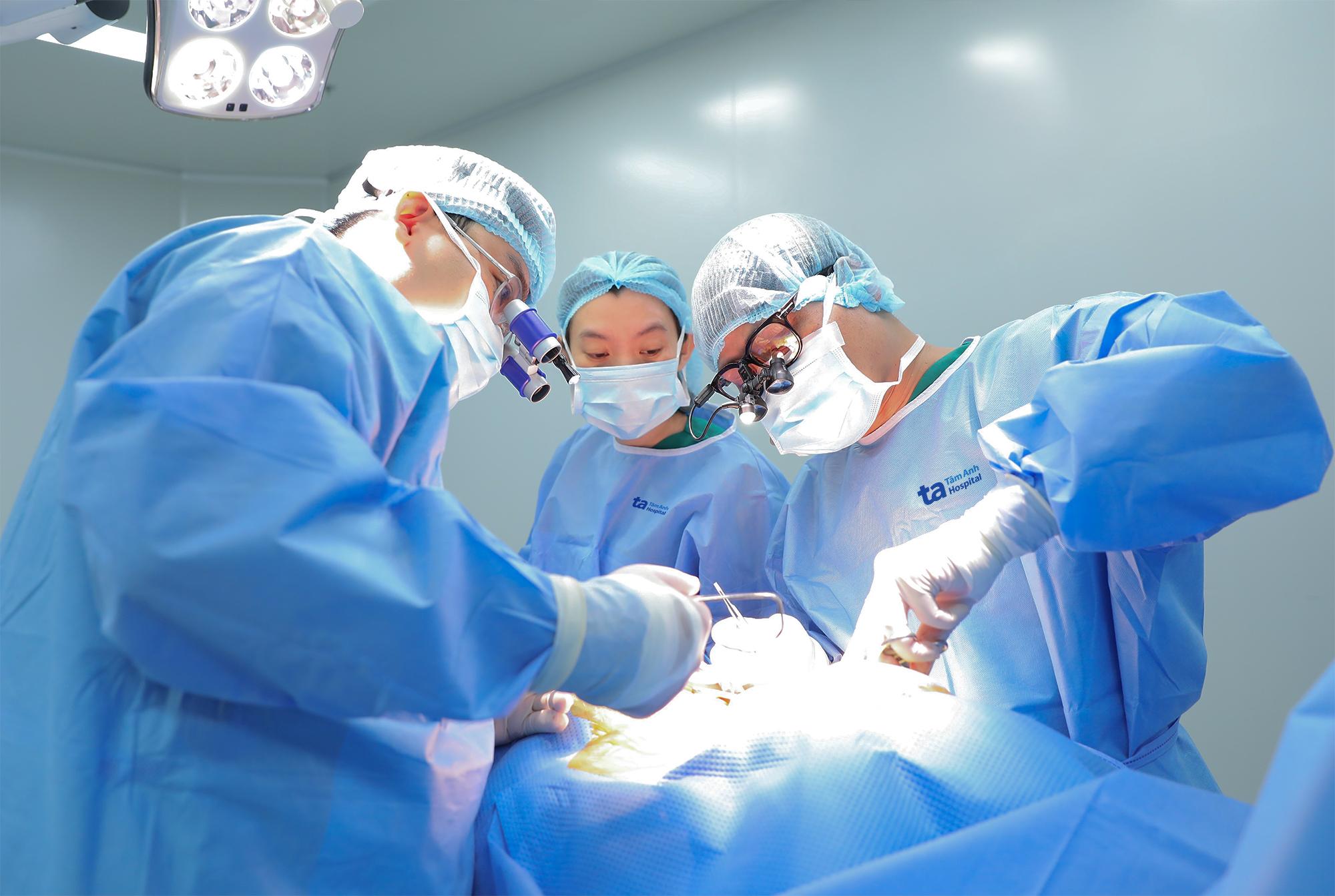 |
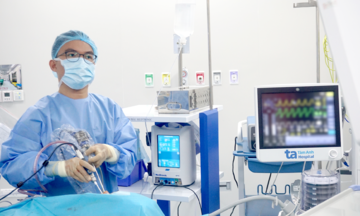
Doctor Khang (far right) and the surgical team operate on a patient. *Trung Vu* |
Doctors prescribed medication to stabilize the patient's blood pressure. A CT scan confirmed 80% stenosis of the right internal carotid artery and mild to moderate (20-60%) coronary artery stenosis with severe calcification.
Master of Science, Doctor Tran Thuc Khang, Deputy Head of Cardiovascular Surgery, Heart Center, Tam Anh General Hospital Ho Chi Minh City, identified this as a case of multi-system vascular damage due to atherosclerosis. While the coronary arteries, which supply the heart, showed moderate narrowing in multiple areas manageable with medical treatment, the right carotid artery, supplying the brain, was severely narrowed. Without surgical intervention to address the atherosclerotic lesion causing the stenosis, the risk of cerebral vascular accident was high. The patient also had extensive pulmonary cavitary lesions from incompletely treated pulmonary tuberculosis, posing a surgical risk.
Following a consultation, the surgical team performed an endarterectomy to remove the atherosclerotic plaque narrowing the lumen of the internal carotid artery. According to Doctor Khang, various carotid endarterectomy techniques exist: longitudinal arteriotomy to remove plaque and patch the artery, or the "eversion" technique for the internal carotid artery. Throughout the surgery, continuous brain perfusion must be ensured with monitoring equipment for cerebral oxygen saturation.
The team detached the internal carotid artery, inverted it, removed the inner atherosclerotic plaque, and then reattached the internal carotid artery to its original position. This technique avoids artificial patch materials, reducing the risk of postoperative thrombosis, bleeding complications, re-stenosis rates, and surgical duration.
Post-surgery, the patient's blood pressure remained stable, with no intraoperative neurological complications, and he was discharged after three days.
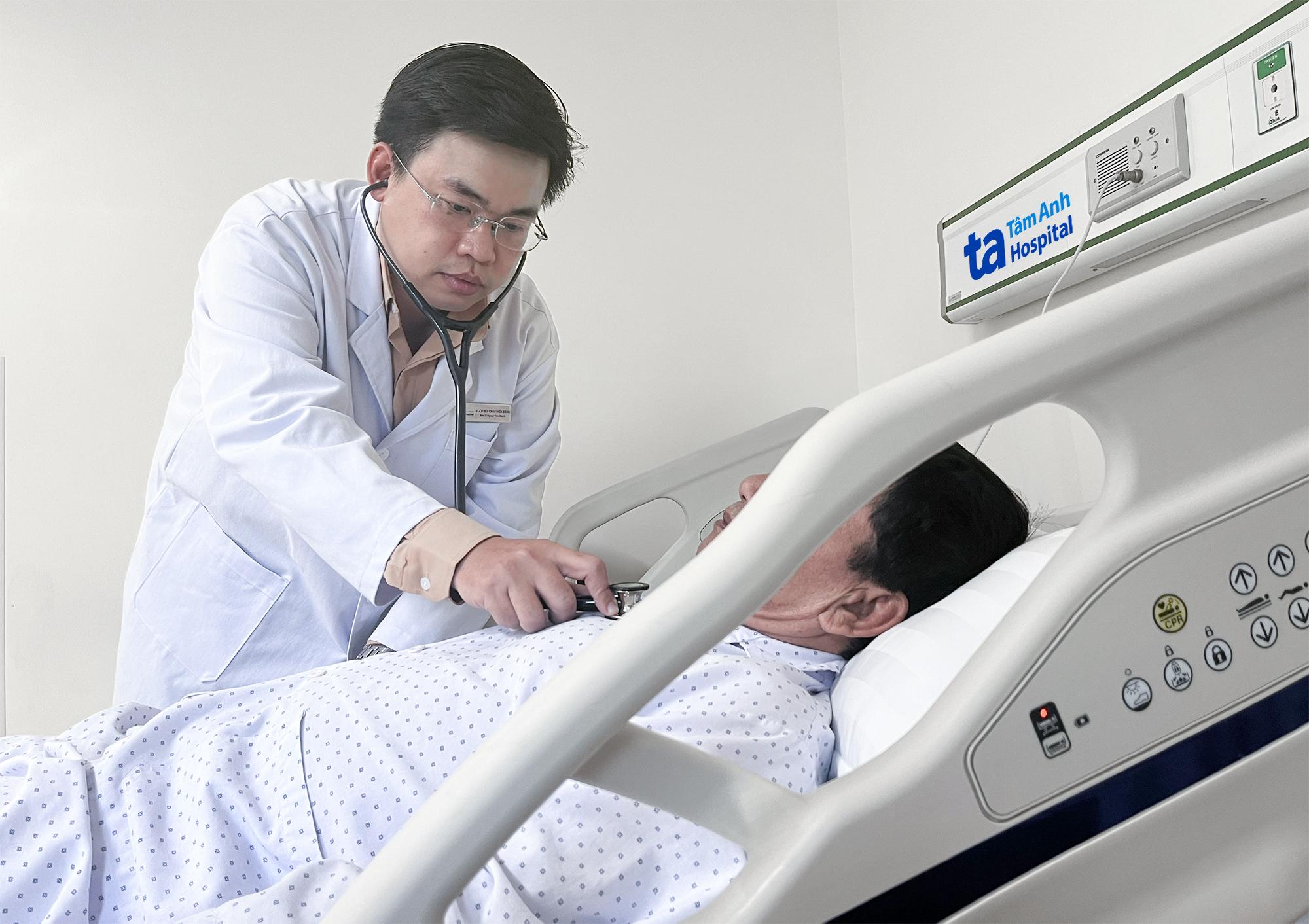 |
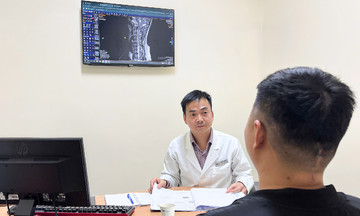
Doctors check the patient's health before discharge. *Ha Vu* |
According to Doctor Khang, approximately 70-75% of internal carotid artery stenosis cases are asymptomatic, discovered incidentally during examinations for other conditions or after a stroke. Patients with risk factors, such as a family history of atherosclerosis or coronary artery disease, smoking, obesity, heavy alcohol consumption, or underlying conditions like hypertension, dyslipidemia, and diabetes, require regular health check-ups.
Thu Ha
*Patient's name has been changed*
| Readers can submit cardiovascular questions here for doctors to answer. |