Earlier this year, Mr. Hung traveled from Quang Ngai to Tam Anh General Hospital, Ho Chi Minh City, for a follow-up examination. Dr. Ta Phuong Dung, Associate Director of the Urology - Nephrology - Andrology Center and Head of the Internal Medicine - Dialysis Department, noted that Mr. Hung's glomerular filtration rate (GFR) was stable at 38.9 mL/min/1.73 m². He was prescribed medication for the next two months, maintaining a proper diet, and is now able to walk, recover his health, and play sports.
Mr. Hung had no underlying health conditions and regularly played football. In 2022, he contracted Covid-19, which led to multi-organ failure, with weakened lung and heart function, requiring extracorporeal membrane oxygenation (ECMO) intervention for three months at another hospital. He narrowly escaped death, but his body was severely debilitated, weighing only 40 kg, and he suffered acute kidney failure. Transported by stretcher to Tam Anh General Hospital, Ho Chi Minh City, he was unable to sit up on his own and required assistance for all daily activities. "At times, I felt I was merely existing, not truly living," Mr. Hung recalled.
Dr. Dung explained that upon admission, the patient's GFR was approximately 30 mL/min/1.73m², equivalent to stage 3b kidney failure, a sequela of systemic inflammation and multi-organ failure caused by Covid-19. The patient's body was debilitated and dehydrated, resulting in severe malnutrition and muscle atrophy after three months of immobility. When the body is too weak, organs, including the kidneys, lack sufficient energy and resources for recovery. His lungs were also fibrotic, with chronic hypoxia causing even more rapid kidney function decline. To gain weight, he needed to consume more protein and energy, but his stage three kidney failure could not process large amounts of protein, which could easily progress to stage 4 or stage 5.
Dr. Dung could not apply standard fluid and nutritional regimens to Mr. Hung as she would for typical kidney failure patients. "Administering too little fluid means the kidneys won't receive enough perfusion to recover, while too much or inappropriate fluid carries a risk of fluid overload, electrolyte imbalance, and heart failure for the patient," the doctor explained.
The doctor prescribed a combination of fluid replacement and correction of metabolic acidosis and electrolyte imbalances, while closely monitoring the patient's blood pressure, heart rate, and urine output. During this period, the fluid and medication regimen was continuously adjusted, sometimes daily, based on the kidneys' response.
Concurrently, Dr. Dung developed a customized diet for Mr. Hung, prioritizing high-energy, easily digestible proteins that do not increase uric acid, such as: egg whites, fish, chicken, and white meat. Urea and creatinine levels were closely monitored to adjust the diet promptly, preventing further strain on the kidneys.
After more than one month of treatment, Mr. Hung gradually recovered; his GFR improved to nearly 40 mL/min/1.73m², and his weight gradually increased. He was discharged and scheduled for follow-up appointments to adjust medication. In early 2024, feeling well, he began eating irregularly, causing his GFR to drop to 29, reaching the threshold for stage 4 kidney failure. Dr. Dung readjusted the patient's diet, restricting foods that increase metabolic burden on the kidneys, while also administering controlled fluid infusions to help the kidneys excrete accumulated waste, correct electrolyte imbalances, and stabilize blood pressure.
 |
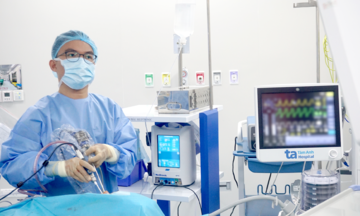
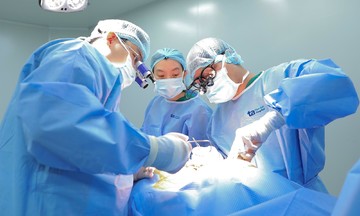
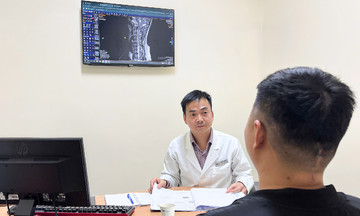
Mr. Hung has regular follow-up appointments and collects medication every two months at Tam Anh General Hospital, Ho Chi Minh City. *Photo: Dinh Lam*
Compared to the previous treatment, this regimen required fewer continuous changes, but still necessitated close monitoring of kidney function indicators to prevent prolonged progression to stage 4 disease. Thanks to timely intervention, after one week of treatment, Mr. Hung's GFR recovered to 38.9 mL/min/1.73m² and has remained stable since.
Currently, he travels to Ho Chi Minh City for regular check-ups and treatment every two months. He weighs 70 kg, can play sports, and continues his business activities. Dr. Dung noted that patients with chronic kidney disease like Mr. Hung can live healthily for decades without needing dialysis if they effectively manage blood pressure, diet, and receive regular fluid infusions.
According to Dr. Dung, kidney failure and Covid-19 have a two-way relationship. Many Covid-19 patients suffer acute kidney injury even without a prior history of kidney disease. This is because the SARS-CoV-2 virus, upon entering the body, causes systemic inflammation (cytokine storm), damaging blood vessels and kidney tissue. Covid-19 causes severe pneumonia, leading to low blood oxygen and potentially low blood pressure, which can result in kidney failure. It also increases the risk of forming small blood clots in vessels, potentially blocking the kidney's microscopic filters. Conversely, individuals with chronic kidney disease have a higher risk of contracting Covid-19 due to weakened immune systems and co-existing conditions like: high blood pressure, diabetes, or cardiovascular disease.
Dr. Dung recommends that individuals who have had Covid-19 should check their kidney function approximately three to six months after recovery. If one has kidney failure, it is essential to adhere to the treatment regimen, control blood pressure, and blood sugar to protect the kidneys from the virus's effects.
Dinh Lam
*The patient's name has been changed.
kidney