Master, Doctor Do Khac Khanh from the Obstetrics and Gynecology Unit at Tam Anh Cau Giay General Clinic, states that menstrual pain (dysmenorrhea) is common, often appearing before or during menstruation. The primary mechanism causing this pain is an increase in prostaglandins, inflammatory mediators produced in the uterine lining. When menstruation begins, the lining sheds, releasing prostaglandins that cause the uterus to contract to expel blood. Higher concentrations of this substance lead to stronger contractions, causing intense cramping, which can be accompanied by nausea, diarrhea, or fatigue.
However, not all instances of severe menstrual pain are physiological. Pain that appears later in life, worsens over time, or does not respond to common painkillers may indicate underlying medical conditions.
Endometriosis is a condition where uterine lining tissue grows outside the uterus, such as on the ovaries, fallopian tubes, or pelvic peritoneum. These tissues still respond to hormonal changes, thickening and bleeding cyclically. Since there is no exit for this blood, it accumulates, causing inflammation and forming cysts and adhesions within the pelvis.
Patients often experience cramping in the lower abdomen, radiating to the back or down the thighs, lasting before, during, and after menstruation. Many cases also involve painful intercourse, increasing the risk of infertility.
Adenomyosis, also known as endometriosis within the uterine muscle, occurs when endometrial tissue grows into the muscular wall of the uterus. This condition causes the uterus to enlarge and harden. During menstruation, blood flows directly into the muscle layer, creating significant pressure and stimulating strong uterine contractions, leading to severe pain.
Uterine fibroids are benign growths in the uterus that can alter its structure and ability to contract. Submucosal fibroids, in particular, can obstruct the shedding process and the outflow of menstrual blood, causing severe pain, heavy periods, or prolonged bleeding, which increases the risk of anemia and general weakness.
 |
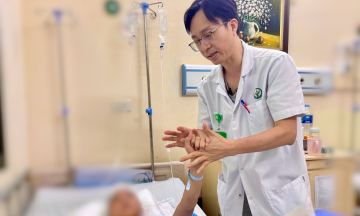
An obstetrician-gynecologist consults with a woman. Photo: Tam Anh Cau Giay General Clinic |
Pelvic inflammatory disease (PID) is often the result of untreated genital tract infections, where bacteria like gonococcus or Chlamydia spread from the vagina to the uterus, fallopian tubes, and ovaries. According to doctor Khanh, chronic inflammation causes the pelvic area to swell and form scar tissue. During menstruation, this area becomes sensitive and easily irritated, leading to increased pain.
Uterine abnormalities can also cause severe menstrual pain. Some women have a congenitally narrow cervix or a cervix that has narrowed due to medical interventions such as abortion or cervical cauterization for ectropion. During menstruation, blood struggles to exit, increasing pressure within the uterus. To push blood through the narrowed segment, the uterus must contract forcefully, causing intense pain.
Malformations such as uterus didelphys or a septate uterus can also obstruct menstrual flow, causing early onset pain.
Copper intrauterine devices (IUDs) can contribute to menstrual pain. Copper IUDs work by creating a mild inflammatory reaction in the uterus to prevent fertilization. However, doctor Khanh notes that this reaction increases prostaglandin production, causing the uterus to contract more strongly during menstruation. This type of pain is common during the first 3-6 months after IUD insertion.
Lifestyle factors also influence pain levels. Prolonged stress, lack of sleep, physical inactivity, an unhealthy diet, or the use of stimulants like caffeine, alcohol, and tobacco can reduce blood circulation in the pelvic area, making the body more sensitive to pain.
To alleviate symptoms, women can apply a warm compress to the abdomen, engage in light exercise, get enough sleep, and maintain a balanced diet. In some cases, a doctor may prescribe painkillers, hormonal medication, or more specialized treatments depending on the cause.
Doctor Khanh advises that conditions like appendicitis, kidney stones, digestive disorders, or urinary tract infections can also cause similar pain, often accompanied by symptoms such as one-sided pain, fever, diarrhea, or constipation.
Women should seek gynecological examination if they experience severe menstrual pain that does not respond to painkillers, or if it is accompanied by prolonged bleeding, fever, difficulty conceiving, or painful intercourse.
Trinh Mai
| Readers can submit questions about obstetrics and gynecology here for doctors to answer. |