Master, Doctor Nguyen Kim Tan, from the Center for Endoscopy and Endoscopic Gastrointestinal Surgery at Tam Anh General Hospital, Ho Chi Minh City, stated that patients can begin eating when they feel hungry again, their abdomen is not distended, and pain has decreased. These are signs that bowel movements have recovered, and the intestines are ready to receive food. Eating too early, before the digestive system is stable, can increase the risk of digestive disorders.
After an appendectomy, patients can resume eating within 24 hours if their digestive system has recovered. The diet needs to be adjusted in stages: from liquid to soft, then back to normal. Following nutritional guidelines helps reduce digestive complications, shortens recovery time, and allows patients to return to normal activities sooner.
First 24 Hours Post-Surgery: Prioritize Liquid, Easily Digestible Foods
On the first day after surgery, the digestive system is still sensitive and less efficient. The nutritional goal at this stage is to gently stimulate bowel movements to resume, avoiding pressure on the stomach and intestines.
Patients should start with small amounts of liquid, easily digestible foods such as thin porridge, rice water, clear broth (strained), or diluted apple juice. These foods provide gentle energy without overloading the digestive system. Avoid fatty, spicy foods, whole milk, or difficult-to-digest foods during this period.
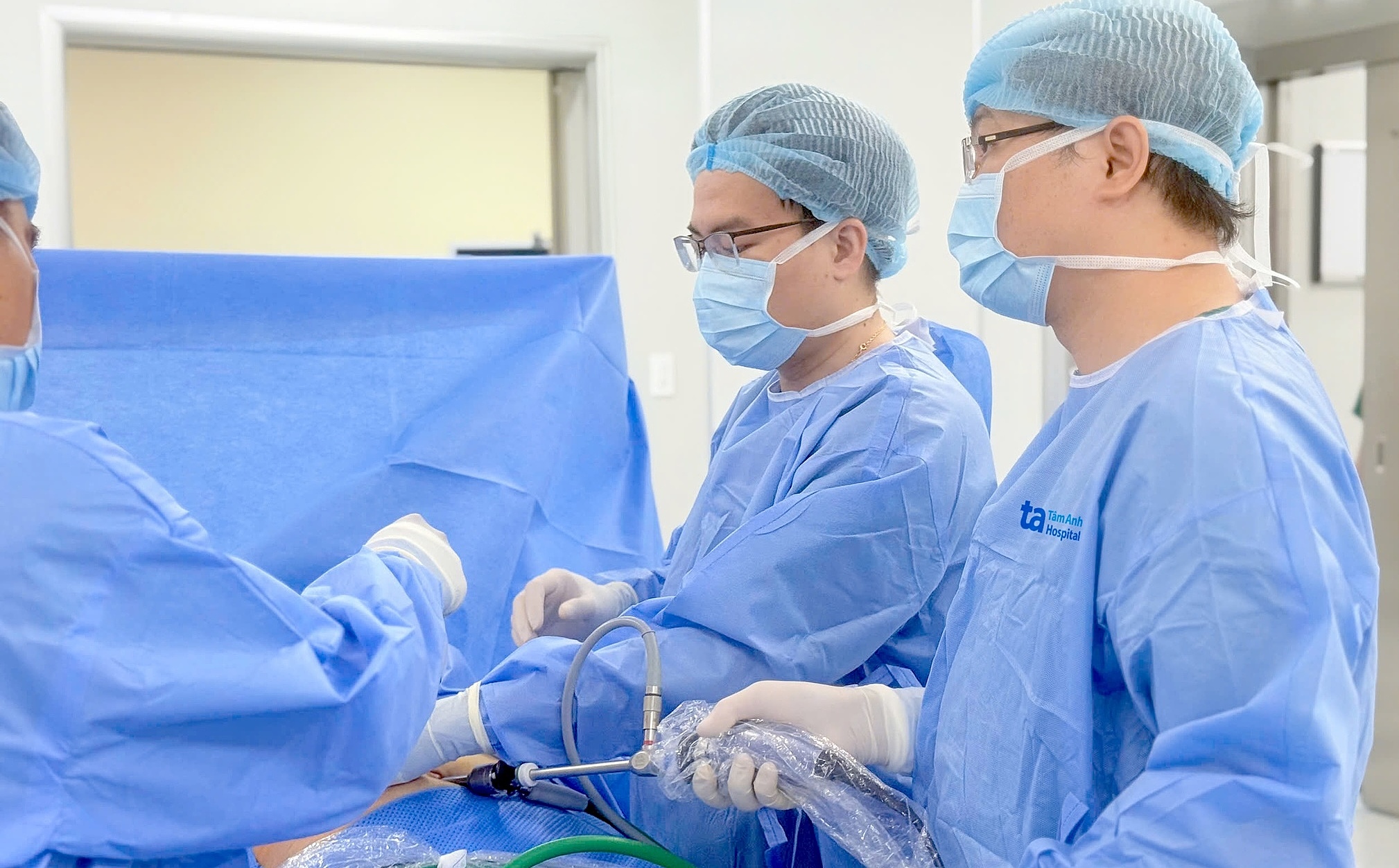 |
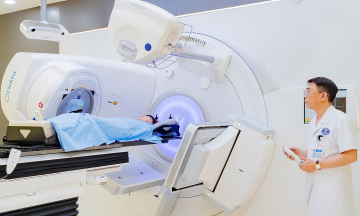
Doctors at Tam Anh General Hospital performing laparoscopic appendectomy for a patient. *Photo: Hospital provided*
Days Two-Three: Supplement Nutrition, Gradually Increase Consistency
Once bowel movements are more stable, patients can transition to a thicker diet while increasing protein intake to support recovery. Suitable dishes include porridge cooked with minced lean meat, soft-cooked fish, or protein-enriched soups. Vegetable broth and lactose-free milk can also be used to supplement energy and micronutrients, while limiting bloating. Patients should eat several small meals throughout the day, avoiding overeating at once to reduce pressure on the digestive system.
Days Four-Seven: Soft Diet, Balanced Nutrition
From day 4 onwards, as the digestive system becomes more stable, patients can transition to a soft, varied diet, prioritizing easily digestible options. Suitable choices include soft rice or mashed rice, soft-boiled chicken, soft-braised fish, and eggs. Vegetables like pumpkin, bok choy, and amaranth provide vitamins, minerals, and soluble fiber, aiding digestion and boosting immunity, but must be thoroughly cooked. Patients can add yogurt to improve gut microbiota, enhance digestion, and reduce the risk of constipation.
From Week Two: Return to Normal Diet
According to Doctor Tan, after about one week, most patients can return to a near-normal diet. However, it is essential to maintain a balanced, nutrient-rich menu to support complete recovery.
Meals should be diverse, including all food groups such as protein (meat, fish, eggs, tofu) for tissue regeneration; carbohydrates (rice, vermicelli, potatoes) for energy; and green vegetables and fruits for vitamins and fiber. Prioritize healthy fats from olive oil and avocados to aid in the absorption of fat-soluble vitamins. Soft fruits like bananas, papayas, and dragon fruits are suitable choices as they are easy to digest and rich in micronutrients.
Patients need to drink 1,5-2 liters of water daily to prevent constipation. Engage in light activity after one-two days, such as slow walking, to stimulate bowel movements and improve circulation. Avoid alcohol, fatty foods, and spicy foods during the initial weeks. Attend follow-up appointments, and monitor for unusual signs such as fever, increased pain, abdominal distension, diarrhea, or swelling and discharge from the incision.
Thao Nhi
| Readers can ask questions about digestive diseases here for doctors to answer. |