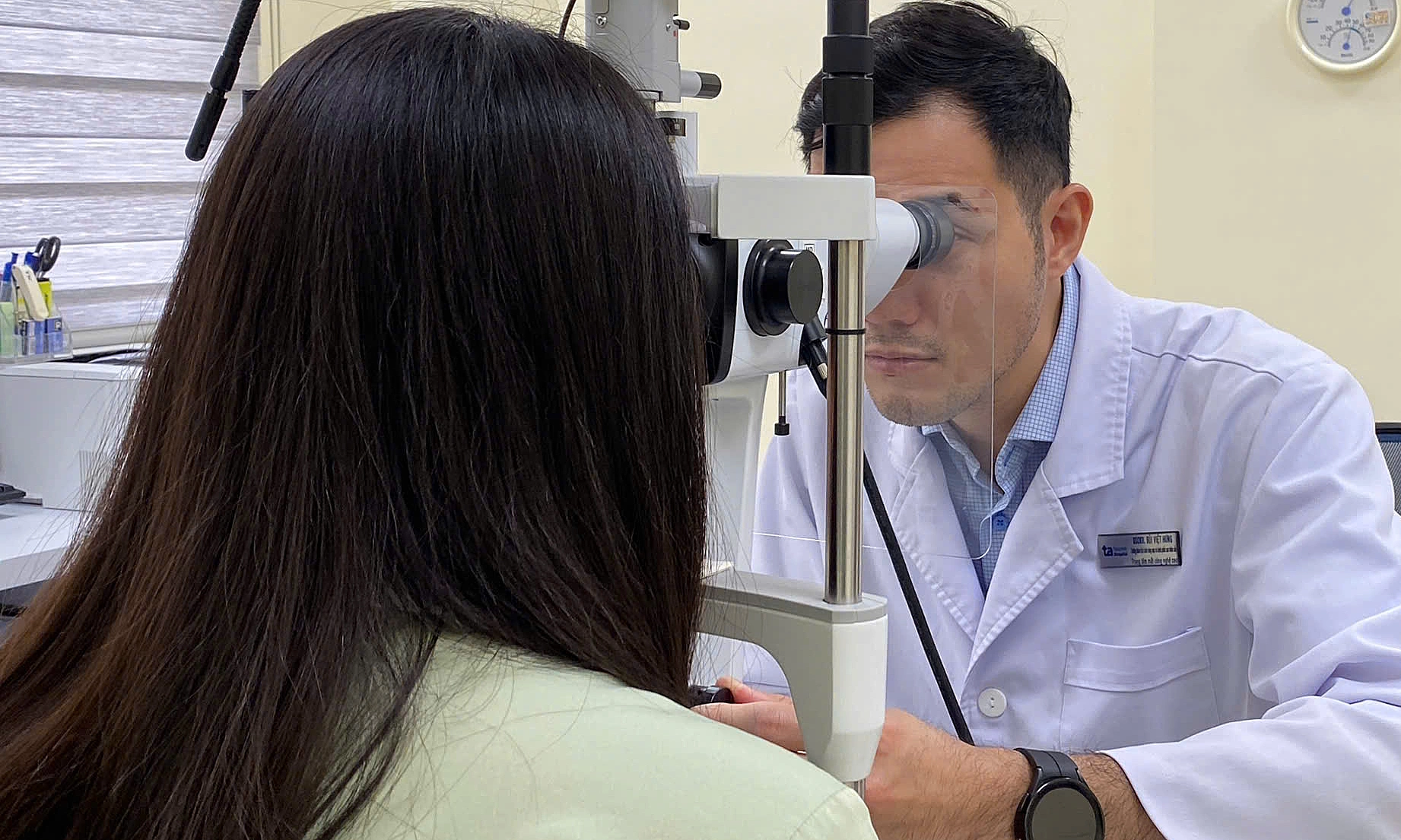
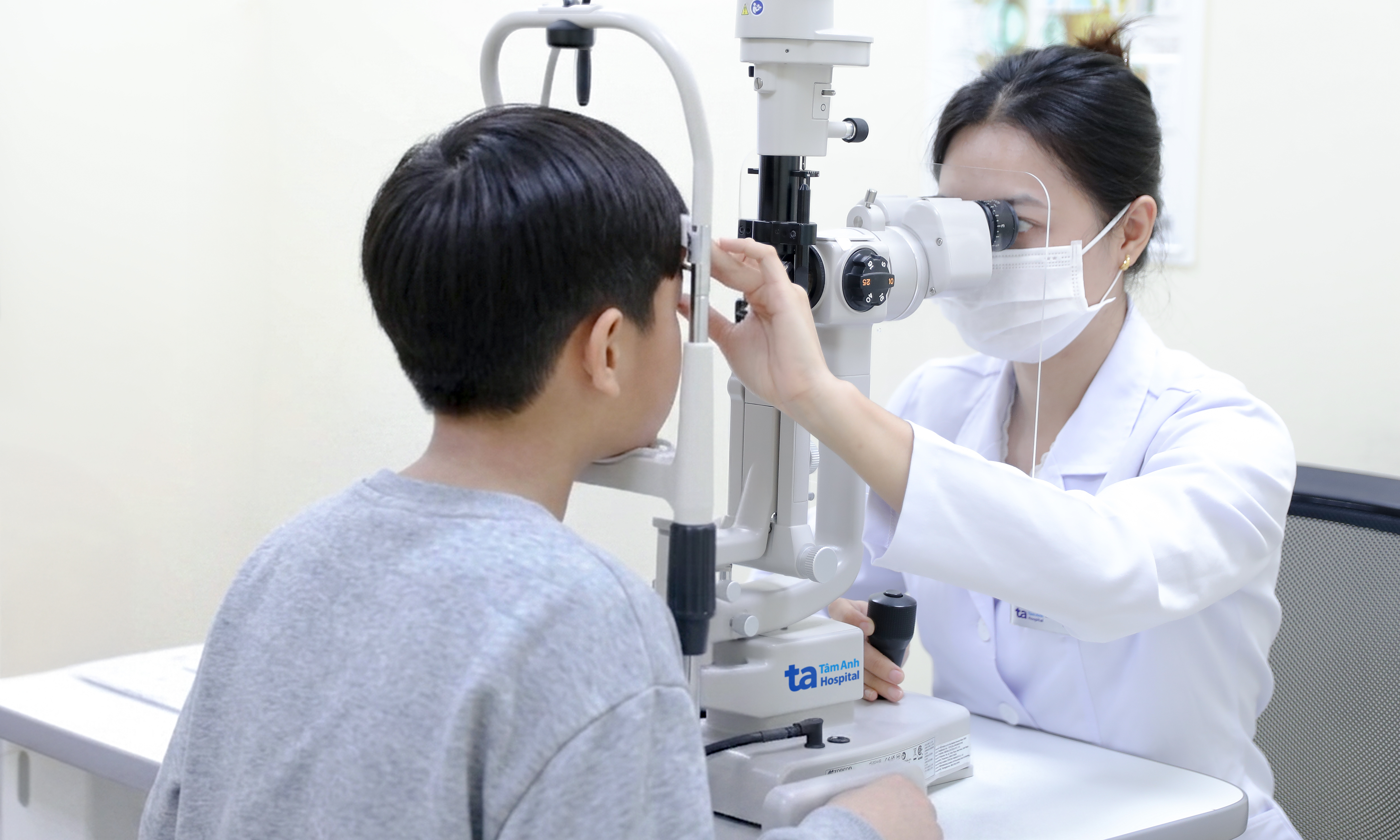
On 13/4, Nature Microbiology published the medical case known as "the Oslo patient." The man has been in sustained HIV remission for five years and no longer requires antiretroviral (ARV) drugs. This remarkable outcome is due to a new immune system from his donor that completely replaced his old blood system, sweeping away all traces of active viral DNA.
The turning point occurred when doctors at Oslo University Hospital performed a bone marrow transplant to treat myelodysplastic syndrome, a type of blood cancer. Initially, the medical team struggled to find a donor with an HIV-resistant mutation. They ultimately decided to use marrow from the patient's 60-year-old brother, with the sole goal of treating the cancer.
Unexpectedly, on the day of the surgery, the team discovered that the donor possessed both copies of the CCR5 delta 32 mutation. This rare gene automatically removes the CCR5 receptor on white blood cells, effectively closing the "gateway" for the pathogen and rendering the virus completely unable to attack the body.
Hematologist Anders Eivind Myhre described this scenario as extremely rare. He noted that the biological compatibility rate between siblings is only 25%, while the group of people carrying HIV-resistant mutations accounts for only about 1%. Infectious disease specialist Marius Trøseid likened the patient's experience to "winning the lottery twice," escaping both bone marrow cancer and HIV.
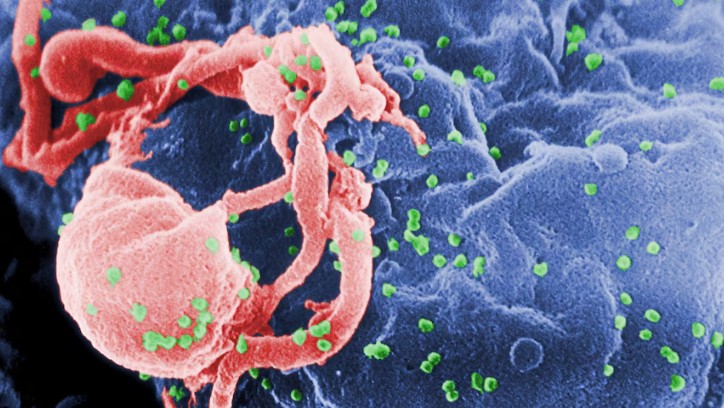 |
HIV virus particles under a scanning electron microscope. Photo: Reuters |
The Oslo patient was diagnosed with HIV in 2006 and began taking medication to control the pathogen in 2010. By 2018, he developed blood cancer and no longer responded to conventional therapies, necessitating the bone marrow transplant.
Two years after the pivotal surgery, he stopped ARV drugs. Recent in-depth tests confirmed the pathogen had completely disappeared from his intestinal tract, where the virus often hides most stubbornly. His antibodies and defense cells also no longer detected any threat from HIV, suggesting his body had erased all memory of the disease.
Despite these breakthrough results, the medical community cautions against widespread application of stem cell transplantation for HIV-infected individuals due to the very high risks involved. The process of "rebooting" the entire immune system makes patients susceptible to severe infections, pushing the mortality rate to 10-20% in the first year. Doctors currently perform this procedure only as a last resort to save the lives of blood cancer patients. The Oslo patient himself experienced a severe rejection phase before successfully recovering his health.
(According to Nature Microbiology, Live Science, Science Alert)